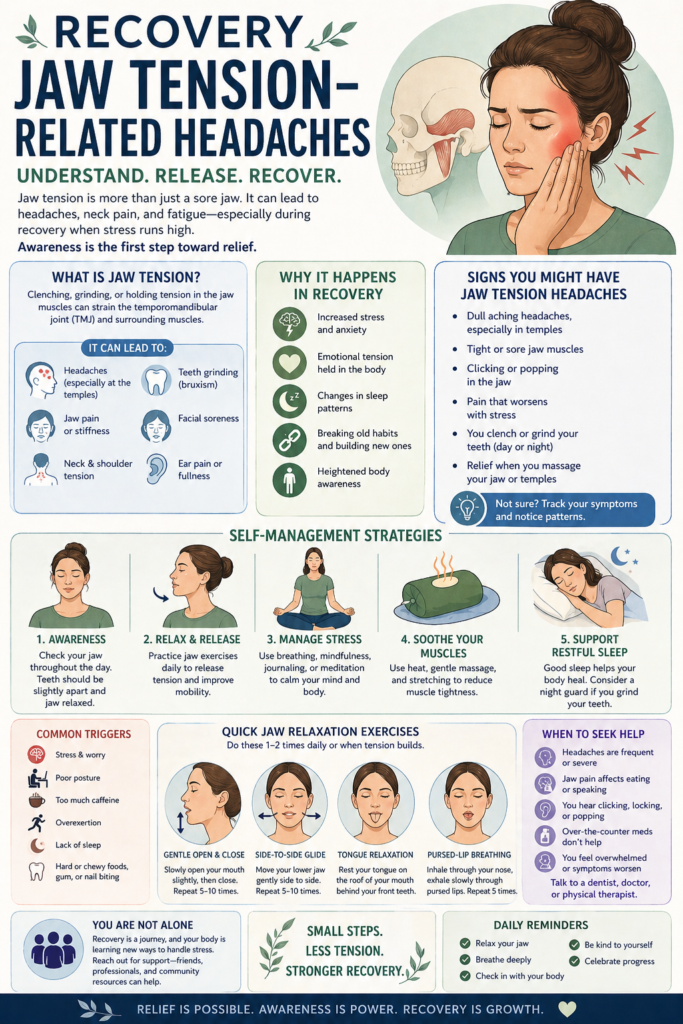
Recovery jaw tension–related headaches are a common yet often overlooked experience, especially for individuals navigating physical and emotional adjustment. During recovery, the body can become more sensitive to stress, and without familiar coping mechanisms, that stress is often held physically, frequently in the jaw. This can lead to clenching, teeth grinding, and muscle strain associated with conditions like Temporomandibular Joint Dysfunction. Because these behaviors are usually unconscious, the resulting headaches may feel confusing or disconnected from any clear cause. Understanding this mind-body connection is an important first step toward recognizing patterns, reducing tension, and managing symptoms more effectively.
Unclenching the Pain: Recovery Jaw Tension–Related Headaches Explained
Headaches during recovery can be frustrating, especially when they seem to appear without a clear cause. One often-overlooked source is jaw tension—a subtle yet powerful physical response to stress. Many people in recovery unknowingly clench their jaw, grind their teeth, or hold tension in their facial muscles, leading to persistent headaches that can feel confusing and exhausting.
Understanding this connection is key. Jaw tension–related headaches are not just physical—they are deeply tied to how the body processes stress, emotion, and change during recovery.
What Are Jaw Tension–Related Headaches?
Jaw tension headaches are typically linked to strain in the temporomandibular joint (TMJ) and surrounding muscles. This condition is often referred to as temporomandibular joint dysfunction (TMD).
When the jaw muscles are overused or constantly tightened, it can lead to:
- Dull, aching pain around the temples
- Tightness in the face or jaw
- Headaches that radiate from the jaw to the head
- Clicking or discomfort when opening the mouth
Why Jaw Tension Increases in Recovery
Recovery—whether from substance use, chronic stress, or emotional strain—places the body in a state of adjustment. This can lead to:
1. Increased Stress Sensitivity
Your nervous system may be more reactive, making you more likely to hold tension physically.
2. Unconscious Clenching (Bruxism)
Grinding or clenching the teeth—especially at night—is common and often unnoticed.
3. Emotional Suppression
Unprocessed emotions can show up physically, often in the jaw, neck, and shoulders.
4. Sleep Disruptions
Poor sleep patterns can worsen muscle tension and increase headache frequency.
Signs Your Headaches May Be Jaw-Related
You might notice:
- Headaches that worsen with stress
- Jaw soreness or stiffness
- Teeth sensitivity or grinding
- Neck and shoulder tightness
- Relief when massaging the jaw or temples
These patterns suggest the source may be muscular rather than neurological.
Self-Management Strategies for Relief
1. Build Awareness of Jaw Tension
Start noticing your jaw throughout the day:
- Is it clenched or relaxed?
- Are your teeth touching when they don’t need to be?
A relaxed jaw should have a small space between the teeth.
2. Practice Jaw Relaxation Techniques
Try:
- Letting your tongue rest gently on the roof of your mouth
- Slightly parting your lips
- Gently stretching your jaw side to side
These small adjustments reduce muscle strain.
3. Address Stress at the Source
Since jaw tension is often stress-driven, reducing stress is essential:
- Mindfulness or meditation
- Deep breathing exercises
- Journaling or emotional processing
Managing stress reduces the body’s need to “hold” tension.
4. Use Heat and Gentle Massage
Applying warmth can relax tight muscles:
- Use a warm compress on the jaw area
- Gently massage temples, cheeks, and jawline
This improves circulation and reduces stiffness.
5. Improve Sleep Habits
- Maintain a consistent sleep schedule
- Avoid stimulants before bed
- Consider a mouth guard if grinding occurs at night
Better sleep supports muscle recovery and reduces clenching.
6. Watch Daily Habits
Small habits can increase jaw strain:
- Chewing gum excessively
- Clenching during focus or stress
- Poor posture (especially forward head position)
Adjusting these reduces ongoing tension.
When to Seek Professional Help
Consider consulting a professional if:
- Headaches are frequent or worsening
- Jaw pain interferes with eating or speaking
- You suspect severe grinding (bruxism)
- Over-the-counter methods aren’t helping
Dentists, physical therapists, or healthcare providers can offer targeted treatment.
The Bigger Picture: Listening to the Body
Jaw tension–related headaches are a reminder that the body stores stress in physical ways. In recovery, this mind-body connection becomes even more important.
The goal is to shift from:
- Unconscious tension → Awareness
- Chronic clenching → Intentional relaxation
- Pain → Prevention
Final Thought
Recovery is not just about breaking habits—it’s about learning how your body responds to stress and how to care for it differently. Jaw tension may be silent, but its effects are not.
By bringing awareness to this hidden pattern, you can reduce headaches, release built-up tension, and move toward a more comfortable, balanced recovery experience.
Unclenching Control: Self-Management Strategies for Recovery Jaw Tension–Related Headaches
Headaches during recovery can feel unpredictable—especially when they don’t seem tied to obvious triggers. One of the most overlooked causes is jaw tension, a physical response to stress that often goes unnoticed. Clenching your jaw, grinding your teeth, or holding subtle facial tension throughout the day can gradually build into persistent headaches.
The good news is that these headaches are highly manageable. With the right self-management strategies, you can learn to recognize, reduce, and prevent jaw tension before it turns into pain.
Why Self-Management Matters
In recovery, your body is relearning how to regulate stress without old coping mechanisms. This often shows up physically—especially in the jaw.
Self-management helps you:
- Catch tension early before it escalates
- Reduce headache frequency and intensity
- Improve awareness of your body’s stress signals
- Build healthier, long-term coping patterns
1. Increase Awareness of Jaw Position
Most jaw tension is unconscious.
Check in throughout the day:
- Are your teeth touching? (They shouldn’t be at rest)
- Is your jaw tight or relaxed?
- Are you clenching during focus or stress?
A relaxed jaw = lips closed, teeth slightly apart, tongue resting gently.
2. Practice Daily Jaw Relaxation
Simple exercises can release built-up tension.
Try:
- Slowly opening and closing your mouth
- Moving your jaw side to side gently
- Letting your tongue rest on the roof of your mouth
Doing this regularly prevents stiffness from building.
3. Interrupt the Clenching Cycle
Clenching often becomes a habit loop.
Break it by:
- Setting reminders to relax your jaw
- Pairing relaxation with daily activities (e.g., every time you check your phone)
- Using a cue phrase like: “Relax my jaw.”
Awareness + repetition = habit change.
4. Manage Stress at the Source
Jaw tension is often a physical expression of stress.
Reduce overall tension through:
- Mindfulness or meditation
- Deep breathing exercises
- Journaling emotions instead of holding them in
When stress decreases, so does clenching.
5. Use Heat and Self-Massage
Relieving muscle tension directly can reduce headaches.
Try:
- Applying a warm compress to the jaw
- Gently massaging the jawline and temples
- Using circular motions with light pressure
This improves circulation and relaxes tight muscles.
6. Improve Posture and Body Alignment
Poor posture—especially forward head position—adds strain to the jaw.
Focus on:
- Keeping your head aligned over your shoulders
- Relaxing your shoulders downward
- Avoiding long periods of slouching
Better posture reduces overall muscle tension.
7. Address Nighttime Grinding (Bruxism)
Many people clench or grind their teeth during sleep without realizing it.
Helpful steps:
- Establish a calming bedtime routine
- Avoid caffeine or stimulants at night
- Consider a mouth guard if recommended
Improving sleep reduces overnight strain on the jaw.
8. Track Patterns and Triggers
Keeping track helps you identify what worsens tension.
Note:
- When headaches occur
- Stress levels at the time
- Activities or habits beforehand
Patterns make prevention easier.
The Bigger Shift: From Tension to Control
Over time, these strategies help you shift from:
- Unconscious clenching → Intentional relaxation
- Reactive pain → Preventive awareness
- Physical stress → Managed response
Final Thought
Jaw tension–related headaches are your body’s way of signaling that something needs attention—not just physically, but emotionally. In recovery, learning to listen to these signals is a powerful step forward.
With consistent self-management, you can reduce pain, increase awareness, and create a more relaxed, balanced state—one where your body no longer carries stress silently in your jaw.
Supporting Relief Together: Family Strategies for Recovery Jaw Tension–Related Headaches
Jaw tension–related headaches can be difficult to recognize, especially during recovery when physical symptoms often overlap with emotional stress. Many individuals don’t realize they are clenching their jaw, grinding their teeth, or holding tension in their face until headaches become frequent or persistent.
For families, this can be confusing—headaches may seem sudden or unexplained. But with awareness and supportive strategies, families can play a key role in helping their loved one identify triggers, reduce tension, and build healthier coping patterns.
Why Family Support Matters
During recovery, the body is relearning how to process stress. Without prior coping mechanisms, tension may manifest physically—especially in the jaw.
Family support can help:
- Increase awareness of hidden tension patterns
- Reduce stress in the environment
- Reinforce healthy habits and relaxation techniques
- Provide emotional stability during discomfort
1. Recognize the Subtle Signs of Jaw Tension
Many signs are easy to miss.
Look for:
- Frequent headaches or temple pain
- Jaw clenching or teeth grinding (especially at night)
- Facial tightness or rubbing the jaw
- Neck and shoulder stiffness
Gently noticing these patterns can help bring awareness without pressure.
2. Encourage Awareness Without Criticism
Statements like:
- “You’re clenching again” (can feel critical)
Instead try:
- “I’ve noticed your jaw seems tight—are you feeling tense?”
The goal is support, not correction. Awareness should feel safe, not stressful.
3. Create a Low-Stress Home Environment
Stress is one of the main drivers of jaw tension.
Families can help by:
- Reducing unnecessary conflict
- Maintaining consistent routines
- Encouraging downtime and relaxation
A calm environment reduces the body’s need to “hold” tension.
4. Model Relaxation and Healthy Coping
People often learn by observation.
You can model:
- Relaxed posture (shoulders down, jaw loose)
- Calm breathing during stress
- Taking breaks instead of pushing through tension
This provides a real-life example of how to manage stress differently.
5. Support Healthy Daily Habits
Small habits can significantly reduce physical tension.
Encourage:
- Consistent sleep schedules
- Balanced meals and hydration
- Breaks during long periods of focus
Stability in daily life supports muscle relaxation and recovery.
6. Help Identify Triggers Together
Jaw tension often follows patterns.
You can gently explore:
- When do headaches happen most?
- What situations increase stress?
- Are there habits (like clenching during focus) involved?
Shared awareness makes prevention easier.
7. Encourage Gentle Relief Techniques
Support doesn’t mean doing everything—it means encouraging helpful practices.
Suggest:
- Warm compresses for the jaw
- Gentle self-massage
- Jaw relaxation exercises
Offer reminders casually, without pressure.
8. Be Patient With the Process
Jaw tension is often a long-standing habit. It won’t disappear overnight.
Avoid:
- Frustration if symptoms persist
- Expecting quick fixes
Instead:
- Stay consistent
- Be supportive
- Focus on gradual improvement
The Bigger Picture: From Tension to Support
Family involvement can help shift the experience from:
- Unnoticed tension → Shared awareness
- Stressful environment → Calm space
- Isolation → Support and understanding
These changes create conditions where healing is more likely.
Final Thought
Recovery is not just emotional—it’s physical. Jaw tension–related headaches are one way the body expresses stress when it hasn’t yet found new ways to release it.
Families don’t need to solve the problem. Simply being aware, supportive, and consistent can make a meaningful difference. Sometimes, the most powerful support is helping someone feel safe enough to finally relax—not just emotionally, but physically too.
Connected Care: Community Resource Strategies for Recovery Jaw Tension–Related Headaches
Jaw tension–related headaches can be frustrating, especially in recovery when physical symptoms often reflect deeper emotional and neurological adjustments. What may seem like a simple headache is frequently linked to chronic jaw clenching, muscle strain, and unprocessed stress. Because these patterns are often unconscious, many individuals struggle to manage them on their own.
This is where community resources become essential. They provide education, professional guidance, and supportive environments that help individuals better understand and manage the connection between stress, jaw tension, and headaches.
Why Community Support Matters
During recovery, the body is relearning how to regulate stress without previous coping mechanisms. This can lead to:
- Increased muscle tension (especially in the jaw)
- Heightened stress sensitivity
- Physical symptoms like headaches
Community resources help by:
- Offering specialized care and expertise
- Providing supportive and validating environments
- Teaching practical tools for long-term relief
1. Dental and TMJ Specialists
Jaw tension is often linked to temporomandibular joint dysfunction (TMD) and bruxism (teeth grinding).
Dental professionals can:
- Assess jaw alignment and muscle strain
- Provide mouth guards for nighttime grinding
- Offer treatment plans to reduce long-term damage
Professional evaluation helps address the physical root of the problem.
2. Physical Therapy and Bodywork Services
Jaw tension rarely exists in isolation—it often involves the neck, shoulders, and posture.
Physical therapists can:
- Teach targeted stretching and strengthening exercises
- Address posture-related strain
- Provide manual therapy for muscle relief
This approach treats the body as a connected system.
3. Mental Health and Counseling Services
Jaw tension is frequently a physical expression of stress and emotional pressure.
Therapists can help:
- Identify stress triggers and emotional patterns
- Develop healthier coping mechanisms
- Reduce the underlying causes of tension
This is especially important in recovery, where emotional regulation is evolving.
4. Stress Management and Mindfulness Programs
Programs focused on relaxation can significantly reduce unconscious clenching.
These may include:
- Meditation or mindfulness training
- Yoga or gentle movement classes
- Guided relaxation techniques
Reducing overall stress lowers the body’s tendency to hold tension.
5. Support Groups and Recovery Communities
Connecting with others in recovery provides:
- Shared understanding of stress-related symptoms
- Practical coping strategies
- Emotional support and accountability
These environments normalize experiences and reduce isolation.
6. Wellness and Holistic Health Resources
Complementary approaches can support relaxation and muscle recovery.
Examples include:
- Massage therapy
- Acupuncture
- Relaxation-focused wellness services
These methods help release built-up physical tension.
7. Educational Workshops and Resources
Understanding the connection between stress and physical symptoms is empowering.
Workshops can provide:
- Information on jaw health and tension patterns
- Techniques for self-awareness and prevention
- Tools for long-term self-management
Knowledge turns confusion into clarity.
8. Crisis and Emotional Support Services
When stress becomes overwhelming, immediate support is important.
In the U.S., the 988 Suicide & Crisis Lifeline provides 24/7 emotional support via call or text (988).
These services:
- Help de-escalate intense stress
- Provide immediate emotional grounding
- Offer guidance in difficult moments
Building a Personalized Support Network
You don’t need every resource—just the ones that fit your needs.
A balanced support system might include:
- Medical/dental care: for physical symptoms
- Therapy: for emotional triggers
- Wellness programs: for stress reduction
- Peer support: for connection and understanding
Layering support creates a stronger foundation for recovery.
The Bigger Picture: Treating the Whole System
Jaw tension–related headaches are not just a physical issue—they reflect the interaction between:
- Body (muscle tension)
- Mind (stress and emotion)
- Environment (daily pressures and triggers)
Community resources address all three.
Final Thought
Recovery is not meant to be navigated alone. Jaw tension–related headaches are often a signal that the body is holding more than it can comfortably manage.
Community resources provide the tools, support, and understanding needed to release that tension—both physically and emotionally. With the right network, what once felt like persistent pain can become an opportunity for awareness, relief, and long-term balance.
Frequently Asked Questions
Here are some common questions:
1. What are jaw tension–related headaches?
These are headaches caused by tight or overworked jaw muscles, often linked to clenching or grinding the teeth. They are commonly associated with Temporomandibular Joint Dysfunction (TMD), which affects the jaw joint and surrounding muscles.
2. Why are these headaches common during recovery?
During recovery, your body is adjusting to stress without previous coping mechanisms. This can lead to:
- Increased muscle tension
- Heightened stress sensitivity
- Unconscious jaw clenching
The jaw often becomes a place where stress is physically held.
3. What do jaw tension headaches feel like?
They typically feel like:
- Dull, aching pain in the temples
- Tightness around the jaw or face
- Pain that spreads to the head, neck, or shoulders
- Pressure rather than sharp pain
4. How can I tell if my headache is jaw-related?
You may notice:
- Jaw soreness or stiffness
- Clicking or popping when opening your mouth
- Teeth grinding (especially at night)
- Relief when massaging your jaw or temples
These are strong indicators that the source is muscular.
5. What is bruxism, and how is it related?
Bruxism is the habit of grinding or clenching your teeth, often during sleep. It is a major contributor to jaw tension and headaches, especially during stressful periods like recovery.
6. Are these headaches dangerous?
They are usually not dangerous, but they can become chronic and uncomfortable if not addressed. Persistent symptoms should be evaluated by a healthcare or dental professional.
7. How can I relieve jaw tension quickly?
Simple techniques include:
- Gently massaging your jaw and temples
- Applying a warm compress
- Letting your jaw relax (teeth slightly apart)
- Practicing slow, controlled breathing
These help release immediate tension.
8. Can stress alone cause jaw tension headaches?
Yes. Stress is one of the main triggers. It can lead to:
- Muscle tightening
- Increased clenching
- Reduced awareness of body tension
Managing stress often reduces headache frequency.
9. Why do I clench my jaw without noticing?
Jaw clenching is often unconscious. It can happen when:
- Concentrating
- Feeling anxious or overwhelmed
- Sleeping
Building awareness is key to changing the habit.
10. How can I prevent these headaches?
Prevention strategies include:
- Checking your jaw position throughout the day
- Practicing relaxation techniques
- Improving posture
- Reducing stress triggers
- Getting adequate sleep
Consistency is more important than intensity.
11. Can posture affect jaw tension?
Yes. Poor posture—especially forward head position—can strain the jaw, neck, and shoulders, increasing tension and contributing to headaches.
12. Should I use a mouth guard?
If you grind your teeth at night, a dentist may recommend a mouth guard. It can:
- Protect your teeth
- Reduce strain on jaw muscles
- Help prevent morning headaches
13. When should I seek professional help?
Consider professional support if:
- Headaches are frequent or worsening
- Jaw pain affects eating or speaking
- You hear persistent clicking or locking
- Self-care strategies aren’t helping
Dentists, physical therapists, or healthcare providers can offer targeted treatment.
14. What’s the most important takeaway?
Jaw tension–related headaches are your body’s way of signaling stored stress.
Managing them effectively means:
- Increasing awareness
- Reducing physical tension
- Addressing emotional stress
You’re not just treating headaches—you’re learning how your body holds and releases stress during recovery.
Conclusion
Jaw tension–related headaches in recovery are not just a physical inconvenience—they are signals that the body is processing stress in a tangible way. By increasing awareness of these patterns and learning to respond with relaxation, stress management, and supportive strategies, individuals can begin to reduce both the frequency and intensity of headaches. Over time, this awareness fosters a shift from unconscious tension to intentional control, allowing the body to release stress more safely and effectively. With consistent attention and care, recovery can become not only a process of change, but also one of greater physical ease, balance, and self-understanding.
Video: That Headache? Your Body’s Screaming for Help #jawtension #stress #recovery