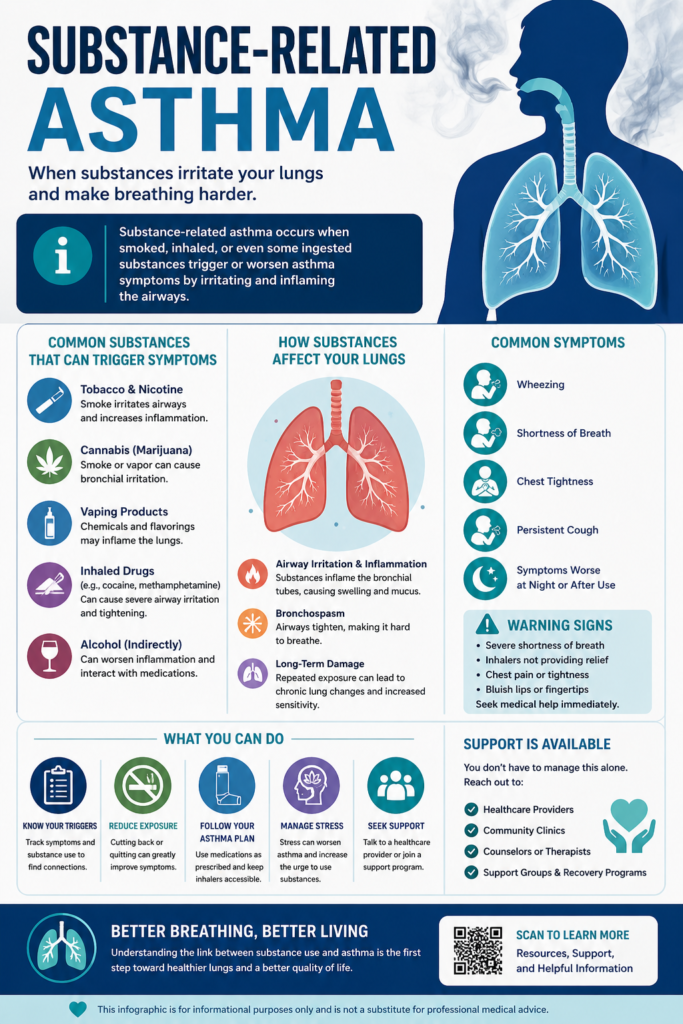
Substance-related asthma refers to breathing problems that resemble or worsen asthma due to the effects of substances entering the body, especially through smoking, vaping, or inhalation. While traditional asthma is often linked to allergens or environmental triggers, substance-related symptoms can be more unpredictable and harder to identify. This overlap can lead to confusion, delayed recognition, and treatments that don’t fully address the root cause. Understanding how substances impact the lungs is essential, particularly for individuals navigating both respiratory issues and substance use. By recognizing these connections, it becomes possible to move beyond symptom management and toward more effective, informed care.
Substance-Related Asthma: When Breathing Problems Aren’t Just Asthma
Breathing problems that look like asthma aren’t always caused by traditional triggers like allergies, exercise, or cold air. In some cases, substances—whether smoked, inhaled, or even ingested—can irritate the airways and create symptoms that closely resemble or worsen asthma. Understanding this connection is especially important for people who struggle with both respiratory issues and substance use.
What Is “Substance-Related Asthma”?
Substance-related asthma isn’t a formal diagnosis, but rather a pattern of asthma-like symptoms triggered or intensified by substance exposure. These symptoms can include:
- Wheezing
- Shortness of breath
- Chest tightness
- Persistent coughing
They may occur during use, shortly after, or as a long-term consequence of repeated exposure.
How Substances Affect the Lungs
Certain substances directly irritate the respiratory system or alter how the lungs function:
1. Airway Irritation and Inflammation
Smoke and vapors can inflame the bronchial tubes, narrowing the airways and making breathing more difficult. This mimics classic asthma physiology.
2. Bronchospasm
Some substances can trigger sudden tightening of airway muscles (bronchospasm), leading to acute wheezing or even asthma attacks.
3. Long-Term Lung Damage
Chronic use may lead to structural changes in the lungs, increasing sensitivity to triggers and making symptoms more persistent—even when not actively using.
Common Substances Linked to Asthma-Like Symptoms
- Tobacco and nicotine products – A major irritant and risk factor for chronic respiratory disease
- Cannabis smoke or vapor – Can inflame airways despite perceptions of being “natural.”
- Inhaled drugs (e.g., cocaine, methamphetamine) – Highly irritating and associated with acute respiratory distress
- Vaping products – Chemicals and flavoring agents may trigger airway inflammation
- Alcohol (indirectly) – Can worsen inflammation or interact with medications
Why This Gets Missed
Substance-related asthma can be overlooked for several reasons:
- Symptoms mimic traditional asthma
- Patients may underreport substance use
- Clinicians may not routinely screen for it
- Overlap with existing asthma diagnoses
This can lead to ineffective treatment, such as increasing inhaler use without addressing the underlying trigger.
The Overlap with Mental Health and Addiction
For individuals dealing with addiction, breathing symptoms can become part of a cycle:
- Stress or anxiety → substance use
- Substance use → worsened breathing
- Breathing issues → more anxiety or panic
- Increased distress → more substance use
This loop can make both respiratory symptoms and substance use harder to manage.
Key Signs It Might Be Substance-Related
- Symptoms flare up around times of use
- Asthma treatments are less effective than expected
- Symptoms persist despite avoiding typical triggers
- There’s a history of smoking, vaping, or inhaling substances
What Helps
1. Honest Assessment
Accurately identifying substance exposure is essential. Without it, treatment may miss the root cause.
2. Reducing or Eliminating Triggers
Cutting back—or ideally stopping—exposure can significantly improve symptoms.
3. Integrated Care
Addressing both respiratory health and substance use together leads to better outcomes than treating them separately.
4. Medical Support
A healthcare provider can help distinguish between primary asthma and substance-induced symptoms and adjust treatment accordingly.
Conclusion
Not all wheezing is asthma, and not all asthma is purely medical. When substances are involved, they can mimic, worsen, or even drive respiratory symptoms. Recognizing this link isn’t about blame—it’s about getting a clearer picture so the right kind of help can actually work.
If breathing issues don’t seem to respond to typical treatments, it may be worth asking a deeper question:
“What else could be affecting my lungs?”
Understanding and Managing Substance-Related Asthma: Practical Self-Management Strategies
Breathing problems linked to substance use can be confusing. Symptoms may look like classic asthma—wheezing, coughing, chest tightness—but the triggers and patterns don’t always follow the usual rules. If substances are part of the picture, managing symptoms effectively means looking beyond inhalers and taking a broader, more informed approach.
What Makes Substance-Related Asthma Different?
Unlike traditional asthma, where triggers are often environmental (like pollen or dust), substance-related asthma is tied to what enters the body—especially through inhalation. That means symptoms can be:
- Inconsistent (only appearing during or after use)
- More intense (due to chemical irritation)
- Less responsive to standard asthma treatments
Understanding your personal pattern is the first step toward control.
Step 1: Identify Your Triggers Honestly
Self-management starts with awareness.
Ask yourself:
- Do symptoms appear after smoking, vaping, or using certain substances?
- Do they worsen at specific times (e.g., at night, after social use)?
- Are inhalers less effective during those periods?
Keeping a simple symptom and use journal can help connect the dots:
- Time of symptoms
- Substance used (if any)
- Severity of breathing issues
- What helped (or didn’t)
Patterns often become clear within a couple of weeks.
Step 2: Understand What Your Body Is Telling You
Instead of viewing symptoms as random or “just asthma,” reframe them as signals:
- Wheezing → airway narrowing or irritation
- Chest tightness → inflammation or muscle constriction
- Shortness of breath → reduced airflow or oxygen exchange
When these symptoms follow substance use, your lungs are essentially saying:
“This is not working for me.”
Step 3: Reduce Exposure Gradually
For many people, stopping immediately isn’t realistic—but reducing exposure still helps.
Consider:
- Cutting down frequency or quantity
- Avoiding deep inhalation or combining substances
- Creating “no-use” days to observe symptom changes
Even small reductions can noticeably improve breathing.
Step 4: Build Alternative Coping Strategies
Substances are often used to manage stress, anxiety, or routine habits. Replacing them is key.
Try:
- Breathing exercises (ironically powerful for both anxiety and lung function)
- Light physical activity (like walking) to improve respiratory capacity
- Structured routines to reduce impulsive use
- Grounding techniques for stress or cravings
The goal isn’t perfection—it’s creating options.
Step 5: Use Medications More Strategically
If you’ve been prescribed inhalers or other asthma medications:
- Track when they work vs. when they don’t
- Notice if effectiveness drops after substance use
- Avoid relying on them to “override” exposure
Medications help—but they’re less effective when the trigger is ongoing.
Step 6: Pay Attention to Warning Signs
Certain symptoms should not be ignored:
- Rapid worsening of breathing
- Inhalers provide little or no relief
- Chest pain or severe tightness
- Frequent nighttime symptoms
These may indicate significant airway irritation or a more serious condition and require medical attention.
Step 7: Connect the Dots Between Breathing and Behavior
One of the most powerful insights is recognizing the cycle:
- Stress or habit → substance use
- Substance use → breathing problems
- Breathing problems → anxiety or panic
- Anxiety → more substance use
Breaking this loop—even at one point—can improve both respiratory health and overall well-being.
Conclusion
Managing substance-related asthma isn’t just about treating symptoms—it’s about understanding cause and effect in your own body. The more clearly you see the connection between substance use and breathing, the more control you gain.
You don’t have to figure everything out at once. Start with awareness, make small adjustments, and build from there. Over time, those small shifts can lead to easier breathing, better health, and more control over both your lungs and your choices.
Supporting a Loved One with Substance-Related Asthma: Family Strategies That Make a Difference
When breathing problems and substance use overlap, it can be hard for families to know what’s really going on—or how to help. Symptoms may look like asthma, but substances can trigger or worsen them in ways that aren’t always obvious. Support from family doesn’t mean controlling the situation—it means understanding, responding effectively, and creating an environment that supports both respiratory health and recovery.
Why Family Support Matters
Substance-related asthma often exists in a cycle:
- Substance use irritates the lungs
- Breathing problems increase stress or anxiety
- Stress can lead to more substance use
Family members are in a unique position to notice patterns, reduce triggers, and encourage healthier choices—often before a crisis happens.
1. Learn What Substance-Related Asthma Looks Like
Understanding the difference between typical asthma and substance-related symptoms helps families respond appropriately.
Look for patterns such as:
- Symptoms worsening after smoking, vaping, or substance use
- Inhalers not working as expected
- Breathing issues appear inconsistently
The goal isn’t to diagnose—it’s to recognize possible connections.
2. Create a Low-Judgment Environment
Shame and confrontation can quickly shut down communication. If your loved one feels judged, they’re less likely to be honest about substance use.
Instead:
- Ask open-ended questions: “I’ve noticed your breathing gets worse sometimes—have you noticed that too?”
- Focus on health, not blame
- Stay calm, even if you’re concerned
Support works best when it feels safe, not critical.
3. Focus on Observations, Not Accusations
Rather than saying:
- “Your substance use is causing this.”
Try:
- “I’ve noticed your breathing seems worse after certain situations. Do you think there could be a connection?”
This approach encourages insight rather than defensiveness.
4. Help Identify Triggers Together
Families can help track patterns by gently noting:
- When symptoms occur
- What was happening beforehand
- Whether substances may have been involved
You might suggest keeping a simple log together, which can:
- Build awareness
- Support medical conversations
- Reduce guesswork
5. Encourage (But Don’t Force) Healthier Choices
You can’t make someone stop using substances—but you can support change.
Helpful approaches:
- Encourage small reductions rather than demanding total abstinence
- Celebrate improvements in breathing or reduced use
- Offer alternatives (e.g., going for a walk instead of smoking together)
Progress is often gradual.
6. Support Medical and Mental Health Care
Substance-related asthma often involves both physical and psychological factors.
You can:
- Offer to attend medical appointments
- Help prepare questions (e.g., “Could substances be affecting these symptoms?”)
- Encourage mental health or addiction support if appropriate
Integrated care leads to better outcomes than treating symptoms alone.
7. Know the Warning Signs of Serious Breathing Problems
Families should be prepared to act if symptoms escalate:
- Severe shortness of breath
- Inhalers are not providing relief
- Bluish lips or fingertips
- Difficulty speaking due to breathlessness
In these cases, seek emergency care immediately.
8. Take Care of Yourself, Too
Supporting someone with both respiratory issues and substance use can be stressful.
Make sure you:
- Set healthy boundaries
- Seek support (friends, counseling, support groups)
- Avoid taking full responsibility for their choices
You’re a support system—not the solution.
Conclusion
Family support can be a powerful stabilizing force in substance-related asthma—but it works best when it’s informed, calm, and consistent. By focusing on patterns, encouraging awareness, and reducing judgment, families can help their loved ones better understand the connection between substance use and breathing.
Sometimes the most impactful thing you can do isn’t to fix the problem—it’s to help someone see it clearly for themselves.
Community Resources for Substance-Related Asthma: Finding Support Beyond the Clinic
When breathing problems are linked to substance use, the solution rarely sits in one place. Inhalers alone may not fix it, and willpower alone isn’t enough either. That’s where community resources come in—offering practical, social, and medical support that helps people better understand and manage substance-related asthma.
Why Community Support Matters
Substance-related asthma often falls through the cracks because it sits between two systems:
- Respiratory care (focused on asthma and lung health)
- Addiction and behavioral health services
Community resources help bridge that gap, providing real-world support where daily habits, stress, and environment play a major role.
1. Primary Care and Community Health Clinics
Local clinics are often the first step in connecting the dots.
They can:
- Evaluate breathing symptoms in context
- Screen for substance-related triggers
- Adjust medications based on real-life patterns
- Refer to specialists or support services
Many community clinics also offer sliding-scale or low-cost care, making them accessible even without insurance.
2. Pulmonary Rehabilitation Programs
Pulmonary rehab isn’t just for severe lung disease—it can help people with recurring asthma-like symptoms improve breathing control.
These programs focus on:
- Breathing techniques
- Exercise conditioning
- Education about lung function
- Symptom management strategies
They can be especially helpful when lung irritation from substances has reduced overall respiratory capacity.
3. Substance Use and Recovery Services
Understanding substance-related asthma requires addressing the substance use itself.
Community options include:
- Outpatient counseling
- Peer recovery groups
- Harm-reduction programs
- Intensive outpatient or residential programs (if needed)
These services help individuals:
- Recognize patterns between use and symptoms
- Develop coping alternatives
- Reduce or stop use in a structured way
4. Mental Health Services
Stress, anxiety, and depression often drive both substance use and breathing symptoms.
Community mental health resources can help by:
- Teaching emotional regulation skills
- Addressing underlying triggers for use
- Reducing anxiety-related breathing issues
This is key because shortness of breath can also be worsened by panic, creating a confusing overlap.
5. Smoking and Vaping Cessation Programs
Even reducing inhaled substances can significantly improve symptoms.
Many communities offer:
- Free quitlines
- Nicotine replacement therapy programs
- Group-based cessation support
- Coaching and relapse prevention tools
These programs are often underused—but highly effective.
6. Support Groups and Peer Networks
Sometimes the most powerful insights come from people with lived experience.
Support groups can:
- Normalize struggles with breathing and substance use
- Provide practical, real-life strategies
- Reduce isolation and shame
- Reinforce motivation for change
Hearing someone say, “My breathing improved when I cut back,” can be more impactful than clinical advice alone.
7. Educational Workshops and Public Health Programs
Local health departments and organizations often provide education on:
- Asthma management
- Environmental triggers
- Substance-related health risks
These programs help people understand:
- How substances affect the lungs
- Why symptoms may not respond to typical treatment
- What changes actually make a difference
8. Emergency and Urgent Care Awareness
Community education also includes knowing when to seek urgent help.
Important signs:
- Severe breathing difficulty
- Inhalers not working
- Rapid symptom escalation
Having access to urgent care—and knowing when to use it—can prevent serious complications.
9. Case Management and Integrated Programs
Some communities offer integrated care programs that combine:
- Medical care
- Behavioral health support
- Substance use treatment
Case managers can help:
- Coordinate appointments
- Navigate insurance or cost barriers
- Keep care consistent
This reduces the “fragmentation” that often makes substance-related asthma harder to manage.
Conclusion
Substance-related asthma isn’t just a medical issue—it’s a whole-life issue, shaped by habits, stress, environment, and access to care. Community resources provide the structure and support needed to understand those connections and make meaningful changes.
You don’t have to rely on one solution. The most effective approach is often a combination:
- Medical guidance
- Behavioral support
- Peer connection
- Practical lifestyle changes
The more pieces you connect, the clearer the picture becomes—and the easier it is to breathe again, both physically and mentally.
Frequently Asked Questions
Here are some common questions:
1. What is substance-related asthma?
Substance-related asthma refers to asthma-like symptoms triggered or worsened by substances, especially those that are smoked, vaped, or inhaled. These substances irritate the airways, causing inflammation, narrowing, and breathing difficulties similar to those of traditional asthma.
2. Is substance-related asthma the same as regular asthma?
Not exactly. While symptoms may look the same, the underlying trigger is different. Traditional asthma is often linked to allergens or genetics, while substance-related asthma is directly connected to chemical irritation or exposure.
3. What substances can trigger asthma-like symptoms?
Common triggers include:
- Tobacco and nicotine
- Cannabis (smoke or vapor)
- Vaping products
- Inhaled drugs (e.g., cocaine, methamphetamine)
- Environmental chemicals or fumes
- Alcohol (indirectly, through inflammation or medication interaction)
4. Can someone have both asthma and substance-related symptoms?
Yes. Many people have pre-existing asthma that is worsened by substance use. In these cases, substances act as powerful triggers, making symptoms more frequent or severe.
5. Why don’t inhalers always work?
Inhalers treat airway inflammation and bronchospasm, but if the irritation is ongoing (from continued substance use), the medication may not be as effective. It’s like treating symptoms while the trigger is still present.
6. How can I tell if my symptoms are substance-related?
Look for patterns:
- Symptoms appear during or after use
- Breathing worsens despite using medication
- Symptoms improve when you reduce or stop exposure
Tracking these patterns over time can provide important clues.
7. Can vaping be safer for asthma than smoking?
Not necessarily. While some people assume vaping is safer, it can still:
- Irritate the airways
- Cause inflammation
- Trigger wheezing and coughing
“Less harmful” does not mean safe for the lungs, especially if you’re sensitive.
8. Can substance-related asthma become permanent?
Repeated exposure can lead to long-term lung changes, increasing sensitivity and making symptoms more persistent—even when not actively using. Early awareness and reduction can help prevent this.
9. Is it possible to reverse the symptoms?
In many cases, yes—especially early on. Reducing or stopping exposure often leads to:
- Improved breathing
- Fewer symptoms
- Better response to treatment
However, long-term damage may not be fully reversible.
10. Why does anxiety make breathing feel worse?
Anxiety can cause:
- Rapid or shallow breathing
- Chest tightness
- Increased awareness of breathing
This can mimic or worsen asthma symptoms, creating a cycle between stress, substance use, and breathing problems.
11. What should I do if I think substances are affecting my breathing?
Start with:
- Noticing patterns between use and symptoms
- Reducing exposure if possible
- Keeping a symptom log
- Talking to a healthcare provider honestly
You don’t need to have everything figured out—awareness is the first step.
12. When is it an emergency?
Seek immediate medical help if you experience:
- Severe shortness of breath
- Inhalers not working
- Chest pain or tightness
- Bluish lips or fingertips
- Difficulty speaking due to breathlessness
These can signal a serious respiratory issue.
13. Can treatment address both asthma and substance use?
Yes. The most effective approach is integrated care, which may include:
- Medical treatment for breathing
- Support for substance use (counseling, groups, etc.)
- Mental health support
Treating both together leads to better outcomes.
14. Is this something people commonly overlook?
Yes. Substance-related asthma is often missed because:
- Symptoms look like typical asthma
- Substance use may not be discussed openly
- The connection isn’t always obvious
This is why awareness—both personal and clinical—is so important.
15. What’s the most important takeaway?
If breathing problems don’t fully make sense or don’t respond to treatment, it’s worth asking:
“Could something I’m using be affecting my lungs?”
That question alone can lead to clearer answers—and better breathing.
Conclusion
Substance-related asthma highlights the importance of looking at breathing problems through a broader lens. When substances contribute to airway irritation and inflammation, simply treating symptoms may not be enough. Real progress comes from identifying patterns, reducing exposure, and addressing the behavioral and environmental factors involved. Whether through self-awareness, family support, or community resources, a more integrated approach can lead to better outcomes. Ultimately, understanding the link between substance use and respiratory health empowers individuals to make changes that support easier breathing and improved overall well-being.
Video: Substance-Related Asthma Is More Common Than You Think #facts #awareness