Cannabinoid Hyperemesis Syndrome is an increasingly recognized condition in which chronic cannabis use leads to recurrent nausea, severe vomiting, and abdominal discomfort—a paradox given cannabis’s reputation for relieving nausea. Many individuals experience repeated cycles of symptoms without immediately connecting them to cannabis use, often resulting in delayed diagnosis and frequent healthcare visits. As cannabis becomes more widely used and accepted, understanding this condition is essential for both individuals and healthcare providers. Recognizing the pattern early can prevent unnecessary suffering and guide more effective management.
Cannabis-Induced Vomiting: When a “Relaxing” Drug Triggers Severe Nausea
What is happening?
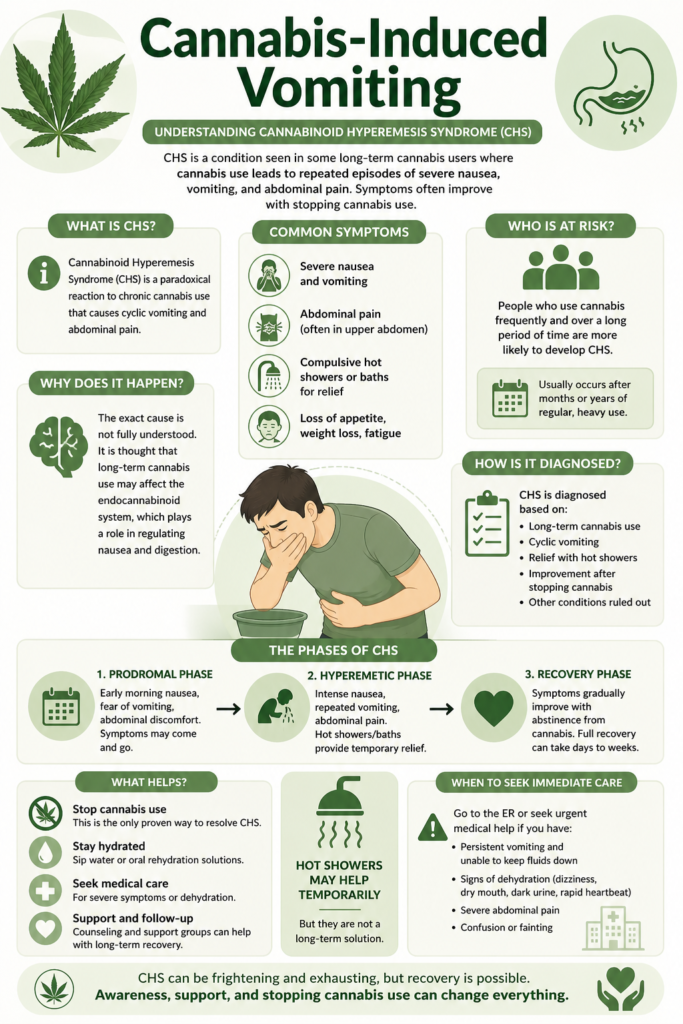
Cannabinoid Hyperemesis Syndrome is a condition seen in some long-term cannabis users where the body paradoxically reacts with recurrent nausea, intense vomiting, and abdominal pain. It often surprises people because cannabis is commonly associated with reducing nausea, not causing it.
🔍 What it looks like
People experiencing CHS often describe:
- Cycles of uncontrollable vomiting
- Persistent nausea that doesn’t respond to typical remedies
- Abdominal cramping or burning pain
- A strong urge to take hot showers or baths for temporary relief
- Symptoms that come and go but worsen over time
🧠 Why does it happen?
The exact mechanism isn’t fully understood, but researchers believe:
- Chronic cannabis use may disrupt the body’s endocannabinoid system
- It may affect how the brain and gut regulate nausea and digestion
- Over time, the body’s response flips—from anti-nausea to pro-vomiting
⚠️ Why it’s often missed
CHS is frequently misdiagnosed as:
- Food poisoning
- Stomach flu
- Anxiety-related nausea
Because many people (and even some clinicians) don’t immediately connect heavy cannabis use with vomiting, diagnosis can take time.
🚨 When it becomes serious
Repeated vomiting can lead to:
- Dehydration
- Electrolyte imbalances
- Weight loss
- Hospital visits for IV fluids
In severe cases, complications can escalate quickly if untreated.
💡 What actually helps
- Stopping cannabis use is the most effective and often necessary treatment
- Supportive care (fluids, anti-nausea meds) may help short-term
- Some people benefit from addiction or behavioral support programs
Hot showers may provide temporary relief—but they don’t treat the underlying issue.
🧠 A different way to think about it
CHS highlights an important point: substances that feel helpful at first can change the body’s response over time. What starts as a coping tool—whether for stress, sleep, or appetite—can evolve into something that worsens physical health.
✍️ Conclusion
If someone is dealing with repeated, unexplained vomiting and uses cannabis regularly, it’s worth considering CHS early. Recognizing the pattern can prevent months (or years) of confusion—and lead to faster recovery.
Taking Control of Cannabis-Induced Vomiting: Self-Management Strategies for Understanding and Relief
Understanding the condition
Cannabinoid Hyperemesis Syndrome is a paradoxical reaction in some regular cannabis users, where instead of relieving nausea, cannabis begins to trigger cycles of severe vomiting, abdominal pain, and distress. Learning to recognize and manage it early can make a major difference in recovery.
🔍 Recognizing the pattern
Self-management starts with awareness. Many people notice:
- Repeated vomiting episodes that come in cycles
- Temporary relief with hot showers or baths
- Symptoms that worsen with continued cannabis use
- Periods of feeling normal between episodes
Tracking these patterns is often the first step toward clarity.
🧠 Strategy 1: Build awareness through tracking
Keep a simple daily log of:
- Cannabis use (amount, type, frequency)
- Nausea or vomiting episodes
- Triggers (stress, food, sleep changes)
- Relief methods (showers, medications)
This helps connect cause and effect—and can be powerful when discussing symptoms with a clinician.
⚖️ Strategy 2: Test the relationship with cannabis
The most reliable way to understand CHS is to pause cannabis use and observe what happens:
- Symptoms often improve within days to weeks
- Returning to use frequently brings symptoms back
This “trial and response” approach can confirm the diagnosis in real life.
💧 Strategy 3: Manage symptoms safely
During active episodes:
- Prioritize hydration (water, electrolyte drinks)
- Eat small, bland meals if tolerated
- Use prescribed anti-nausea medications if available
- Rest and avoid triggers
Hot showers can provide temporary relief—but rely on them cautiously, as excessive heat exposure can cause dehydration.
🧩 Strategy 4: Understand your “why.”
For many people, cannabis use is tied to:
- Stress or anxiety relief
- Sleep support
- Coping with emotional discomfort
Identifying these underlying needs makes it easier to replace cannabis with healthier coping strategies.
🧠 Strategy 5: Replace, don’t just remove
Instead of only stopping cannabis, build alternatives:
- Stress management (breathing exercises, movement)
- Sleep routines (consistent timing, reduced screen use)
- Emotional support (therapy, peer support)
This reduces the likelihood of returning to use.
🚨 When to seek help
Self-management is helpful, but medical care is important if you experience:
- Inability to keep fluids down
- Signs of dehydration (dizziness, dry mouth, dark urine)
- Severe abdominal pain
- Repeated ER visits for vomiting
✍️ Conclusion
CHS can feel confusing—especially when something once used for relief becomes the cause of distress. Self-management is about connecting the dots, understanding your body’s signals, and making informed changes. With awareness and the right support, recovery is very achievable.
Supporting a Loved One with Cannabis-Induced Vomiting: Family Strategies for Understanding and Care
Understanding the condition together
Cannabinoid Hyperemesis Syndrome can be confusing for families. A substance often associated with relaxation and nausea relief can, over time, lead to cycles of severe vomiting, abdominal pain, and repeated distress. For loved ones, the challenge is not just managing symptoms—but understanding what’s really happening.
🔍 What families may observe
Family members often notice:
- Repeated vomiting episodes with no clear cause
- Frequent hot showers or baths for relief
- Emergency room visits without lasting answers
- Frustration, denial, or confusion around cannabis use
Recognizing these patterns can help families connect symptoms to CHS earlier.
🧠 Strategy 1: Learn before reacting
Start with shared understanding:
- CHS is not widely known, even in healthcare settings
- Symptoms are real, physical, and often severe
- Cannabis may feel helpful to the person—even if it’s contributing to the problem
Approaching the situation with knowledge reduces blame and improves communication.
💬 Strategy 2: Communicate without confrontation
How you talk about it matters:
- Use observations, not accusations (“I’ve noticed you get sick after using”)
- Stay curious rather than judgmental
- Avoid ultimatums early on
This keeps the conversation open instead of pushing the person away.
⚖️ Strategy 3: Gently connect the dots
Many people with CHS don’t immediately believe cannabis is the cause. Families can:
- Encourage pattern tracking (symptoms vs. use)
- Suggest a trial break from cannabis as an experiment
- Share reliable information rather than opinions
Let the evidence build naturally rather than forcing conclusions.
💧 Strategy 4: Support during episodes
When symptoms are active:
- Help maintain hydration (small sips, electrolyte drinks)
- Provide a calm, low-stimulation environment
- Monitor for warning signs (dehydration, confusion, severe pain)
- Assist with getting medical care if needed
Even a simple presence can reduce distress during intense episodes.
🧩 Strategy 5: Address the bigger picture
Cannabis use is often tied to:
- Stress or anxiety
- Sleep problems
- Emotional coping
Families can support healthier alternatives by:
- Encouraging routines and structure
- Supporting therapy or counseling
- Promoting non-substance coping strategies
The goal isn’t just stopping cannabis—it’s replacing what it was doing.
🚨 Strategy 6: Know when to step in
Seek medical help if your loved one:
- Can’t keep fluids down
- Shows signs of dehydration
- Has severe or worsening abdominal pain
- Needs repeated urgent care visits
CHS can escalate quickly without proper care.
❤️ A balanced approach
Supporting someone with CHS requires a mix of:
- Empathy (understanding their experience)
- Patience (change may take time)
- Clarity (recognizing the role cannabis may play)
✍️ Conclusion
Family support can be a turning point. When loved ones shift from frustration to informed support, it becomes easier for the person experiencing CHS to recognize patterns, feel understood, and take steps toward recovery.
Connecting the Dots: Community Resource Strategies for Understanding Cannabis-Induced Vomiting
Why community support matters
Cannabinoid Hyperemesis Syndrome is often misunderstood, misdiagnosed, or overlooked. Many people cycle through emergency visits without clear answers. Community resources—when used effectively—can bridge the gap between confusion and clarity, helping individuals recognize patterns, access care, and move toward recovery.
🔍 What communities can help identify
Across community settings, patterns often emerge:
- Recurrent vomiting episodes with unclear cause
- Temporary relief behaviors (like frequent hot showers)
- Ongoing cannabis use despite worsening symptoms
- Repeated urgent care or ER visits
When multiple systems “see” the same pattern, recognition becomes faster.
🏥 Strategy 1: Use local healthcare access points
Community-based healthcare can be a first line of insight:
- Primary care clinics can track symptoms over time
- Urgent care and ER providers can identify recurring visits
- Pharmacists can flag ineffective nausea treatments
Encourage continuity—seeing the same provider helps connect the dots.
🧠 Strategy 2: Leverage behavioral health services
Because cannabis use is often tied to coping:
- Counselors and therapists can explore underlying stress, anxiety, or sleep issues
- Substance use programs can provide nonjudgmental education and support
- Integrated care settings can address both physical and behavioral aspects
This is where understanding shifts from “just symptoms” to whole-person care.
👥 Strategy 3: Engage peer and support groups
Community groups offer something unique:
- Shared experiences from others who’ve had CHS
- Validation that symptoms are real and recognizable
- Practical advice on what helped (and what didn’t)
Hearing “this happened to me too” can be more convincing than clinical explanations alone.
🌐 Strategy 4: Use credible educational resources
Online information can either help or confuse. Focus on:
- Reputable medical organizations
- Public health resources
- Educational materials from treatment centers
Avoid relying solely on anecdotal or unverified sources—CHS is still evolving in public awareness.
🧩 Strategy 5: Coordinate care across systems
The most effective approach is connected:
- Share information between providers (with consent)
- Keep records of symptoms, visits, and cannabis use patterns
- Advocate for yourself or your loved one when patterns are missed
Fragmented care often delays diagnosis—coordination speeds it up.
⚖️ Strategy 6: Reduce stigma through community awareness
Stigma can prevent people from seeking help. Communities can:
- Normalize conversations about substance use and health
- Educate that CHS is a medical condition, not a moral failing
- Encourage early help-seeking without judgment
This creates an environment where people feel safer asking questions.
🚨 When community resources aren’t enough
Even with strong support, medical care is critical if:
- Vomiting is persistent or severe
- Hydration can’t be maintained
- Symptoms escalate quickly
Community resources should complement, not replace, medical treatment.
✍️ Closing perspective
Understanding CHS doesn’t usually happen in one place—it happens across clinics, conversations, and community connections. When these resources work together, they help individuals move from repeated crises to informed decisions and recovery.
Frequently Asked Questions
Here are some common questions:
1. What is cannabis-induced vomiting?
Cannabis-induced vomiting is most commonly linked to Cannabinoid Hyperemesis Syndrome, a condition where long-term cannabis use leads to recurrent nausea, severe vomiting, and abdominal pain, despite cannabis often being used to reduce nausea.
2. Why does cannabis cause vomiting instead of preventing it?
Although cannabis can reduce nausea in the short term, chronic use may disrupt the body’s endocannabinoid system, which helps regulate digestion and nausea. Over time, this can flip the effect, leading to increased nausea and vomiting instead of relief.
3. Who is most at risk for CHS?
People who:
- Use cannabis frequently (daily or near-daily)
- Have used cannabis long-term (months to years)
- Use high-potency THC products
Not everyone who uses cannabis develops CHS, but the risk increases with frequency and duration.
4. What are the main symptoms?
- Cycles of intense vomiting
- Persistent nausea
- Abdominal pain
- Temporary relief with hot showers or baths
- Symptoms that come and go over time
5. Why do hot showers help?
Hot showers or baths may temporarily relieve symptoms by affecting temperature regulation and nerve pathways linked to nausea. However, this is only short-term relief—not a cure.
6. How is CHS diagnosed?
There’s no single test. Diagnosis is based on:
- Symptom patterns (cyclic vomiting)
- History of cannabis use
- Improvement after stopping cannabis
Doctors often rule out other causes first.
7. What is the treatment?
The most effective treatment is:
- Stopping cannabis use completely
Supportive care may include:
- IV fluids for dehydration
- Anti-nausea medications
- Rest and monitoring
8. Will symptoms go away after stopping cannabis?
Yes, in most cases:
- Symptoms improve within days to weeks after stopping
- Returning to cannabis often causes symptoms to come back
9. Can CHS become dangerous?
Yes. Severe vomiting can lead to:
- Dehydration
- Electrolyte imbalances
- Kidney problems (in rare cases)
Medical care is important if symptoms are severe or persistent.
10. Is this the same as food poisoning or stomach flu?
No. While symptoms can look similar, CHS is:
- Recurrent (comes back repeatedly)
- Linked to cannabis use
- Often relieved only by stopping cannabis
11. Why don’t more people know about CHS?
- It’s a relatively newly recognized condition
- Cannabis is widely believed to help with nausea
- Awareness is still growing among both the public and healthcare providers
12. What should someone do if they think they have CHS?
- Consider a trial break from cannabis
- Track symptoms and patterns
- Seek medical advice, especially if vomiting is severe
- Stay hydrated and monitor for warning signs
13. Can someone continue using cannabis in moderation?
For people with CHS, even small amounts can trigger symptoms again. Most evidence suggests complete cessation is necessary to prevent recurrence.
14. Is CHS related to addiction?
Not always, but frequent cannabis use may be tied to:
- Coping with stress or anxiety
- Sleep issues
- Habitual use patterns
In some cases, support for substance use may be helpful.
15. Is recovery possible?
Yes. With recognition and stopping cannabis use, most people experience full recovery and resolution of symptoms.
Conclusion
Cannabis-induced vomiting highlights the complex and sometimes unexpected ways the body responds to substances over time. While symptoms can be distressing and disruptive, they are also highly responsive to behavioral change, particularly cessation of cannabis use. Increased awareness, early recognition, and supportive care can significantly reduce complications and improve outcomes. By understanding CHS as a medical condition rather than a mystery or anomaly, individuals and communities can take informed steps toward prevention, timely treatment, and sustained recovery.
Video: Cannabis Induced Vomiting Gets Worse Every Time #CHS #warning