Anxiety is often misunderstood as just worry or stress, but at a deeper level, it is a powerful internal state that drives behavior. When anxiety becomes persistent or overwhelming, it creates an urgent need for relief—both mentally and physically. In this state, the brain prioritizes immediate comfort over long-term well-being, making individuals more vulnerable to using substances or behaviors as a form of escape. Over time, what begins as a way to cope can evolve into a pattern of dependence. Understanding how anxiety controls addiction is essential because it shifts the focus from simply stopping the behavior to addressing the underlying emotional force that sustains it.
When Anxiety Takes Control: How It Drives Addiction
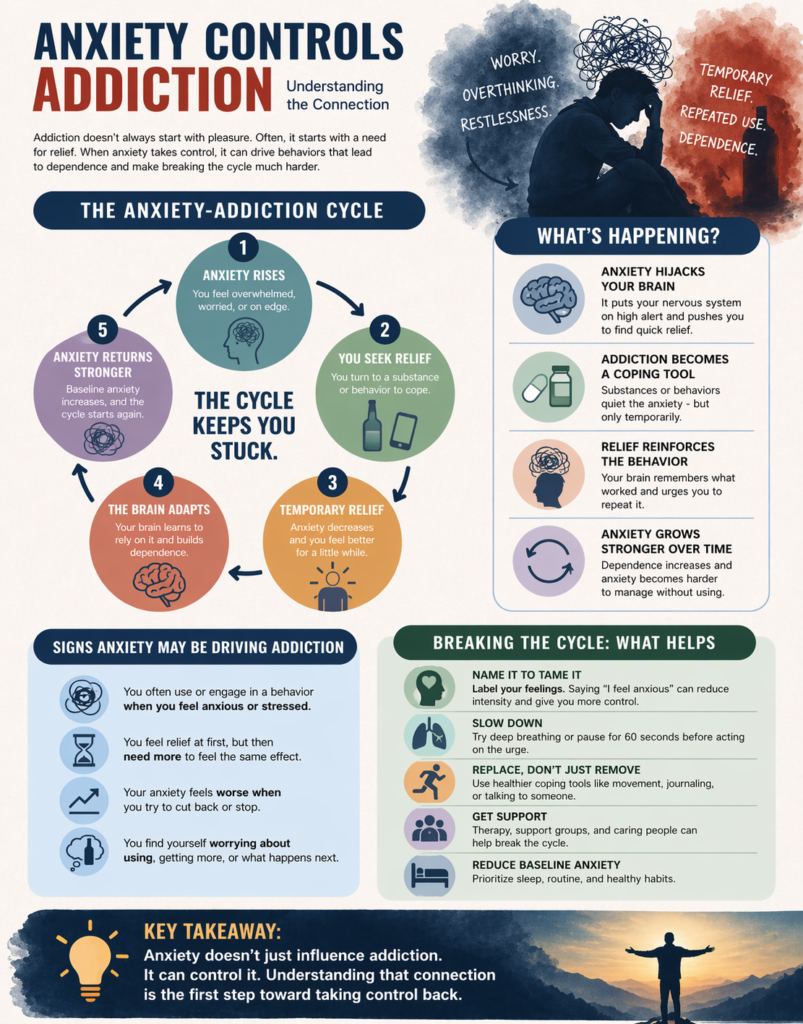
Anxiety doesn’t just feel uncomfortable—it demands relief. And in a world full of quick fixes, that demand can quietly shape behavior in ways that lead straight into addiction.
At its core, anxiety is a state of heightened alertness. Your brain is scanning for danger, your body is tense, and your thoughts often spiral toward worst-case scenarios. This isn’t just “stress”—it’s a physiological and psychological state that pushes you to do something, anything, to make it stop.
That urgency is where addiction often begins.
The Search for Relief
When anxiety becomes overwhelming, the brain looks for the fastest way to regulate itself. Substances and behaviors—like alcohol, nicotine, overeating, scrolling, or even overworking—can provide immediate relief. They dampen the intensity, even if only temporarily.
That relief is powerful. It teaches the brain a simple equation:
anxiety → use something → feel better
The problem is that this equation doesn’t solve anxiety. It trains dependence.
The Reinforcement Loop
Over time, the brain starts to rely on that external “solution.” This creates a feedback loop:
- Anxiety rises
- You use something to cope
- Relief follows
- The brain remembers and repeats
Eventually, the behavior is no longer a choice—it’s a conditioned response. What started as coping becomes compulsion.
This is why many people don’t recognize addiction right away. It doesn’t always begin with pleasure. Often, it begins with relief.
Why Anxiety Makes Addiction Stronger
Anxiety strengthens addiction in a few key ways:
- It increases sensitivity to discomfort, making relief feel more necessary
- It narrows focus, so short-term relief outweighs long-term consequences
- It creates avoidance patterns, where anything that reduces distress becomes prioritized
In other words, anxiety doesn’t just trigger addictive behavior—it reinforces it.
The Illusion of Control
Ironically, the very thing used to manage anxiety often makes it worse over time. Substances and avoidance behaviors can:
- Disrupt sleep
- Increase baseline anxiety levels
- Reduce emotional tolerance
This creates a cycle where anxiety grows stronger, not weaker—requiring more of the same behavior to cope.
What feels like control is often the loss of it.
Breaking the Cycle
If anxiety is driving addiction, then addressing anxiety directly is essential. That doesn’t mean eliminating anxiety completely—it means changing your relationship with it.
Some evidence-based approaches include:
- Affect labeling (naming what you feel) to reduce intensity
- Cognitive-behavioral strategies to challenge anxious thinking
- Exposure techniques to reduce avoidance patterns
- Healthier regulation tools like movement, breathing, and structured routines
These strategies don’t provide instant relief in the same way—but they build something more sustainable: tolerance, awareness, and control.
Final Thought
Addiction isn’t always about chasing a high. More often, it’s about escaping a feeling.
When anxiety is in the driver’s seat, addiction becomes the vehicle. Understanding that connection is one of the first steps toward breaking the cycle—and finding a different way to cope.
Breaking the Anxiety–Addiction Cycle: Practical Self-Management Tools
Understanding that anxiety often drives addiction is a powerful insight—but insight alone doesn’t create change. What matters next is learning how to manage anxiety in real time, before it turns into the urge to escape.
Addiction, in many cases, isn’t about seeking pleasure. It’s about regulating discomfort. When anxiety spikes, the brain looks for immediate relief, and if it has learned that a substance or behavior provides that relief, it will push you in that direction automatically.
Self-management strategies work by interrupting that automatic pattern and replacing it with a more sustainable one.
Step One: Recognize the Pattern
Before you can change anything, you have to see it clearly.
Start by identifying your personal anxiety–addiction loop:
- What situations trigger your anxiety?
- What thoughts show up in those moments?
- What do you typically turn to for relief?
This isn’t about judgment—it’s about mapping the process. Once you can see the sequence, you create a space to intervene.
Step Two: Slow the Moment Down
Anxiety creates urgency. It tells you that you need relief now. One of the most effective ways to disrupt this is to slow the process down.
Simple techniques include:
- Taking a few controlled breaths
- Pausing for even 60–90 seconds before acting
- Physically changing your environment (standing up, walking, stepping outside)
This doesn’t eliminate anxiety, but it reduces its intensity enough to give you a choice.
Step Three: Label What You’re Feeling
One of the most overlooked tools is also one of the most effective: putting your feelings into words.
Instead of saying “I’m stressed,” get specific:
- “I feel overwhelmed and tense.”
- “I feel restless and on edge.”
- “I feel worried about losing control.”
This process—often called affect labeling—helps reduce emotional intensity by engaging more rational parts of the brain. It turns a vague, overwhelming state into something more defined and manageable.
Step Four: Replace, Don’t Just Remove
Trying to eliminate a coping behavior without replacing it usually fails. The brain still wants relief—it just doesn’t know where to get it.
Instead, build alternative responses that regulate anxiety without reinforcing dependence:
- Movement (walking, stretching, exercise)
- Sensory grounding (cold water, deep pressure, focused attention)
- Structured distractions (tasks that require focus but aren’t overwhelming)
- Talking to someone or writing things out
The goal isn’t perfection—it’s giving your brain another option.
Step Five: Build Tolerance to Discomfort
This is where real change happens.
Anxiety becomes less controlling when you learn that you can experience it without immediately escaping it. This doesn’t mean forcing yourself to suffer—it means gradually increasing your ability to sit with discomfort.
Over time, this rewires the brain:
- Anxiety no longer equals danger
- Discomfort no longer demands immediate action
- Urges become temporary, not commands
This shift reduces the power anxiety has over your behavior.
Step Six: Reduce Baseline Anxiety
If your overall anxiety level is high, you’ll be more vulnerable to the cycle.
Daily habits that help regulate baseline anxiety include:
- Consistent sleep
- Regular physical activity
- Limiting stimulants like caffeine
- Creating predictable routines
These may seem simple, but they directly affect how reactive your nervous system is.
Final Thought
When anxiety controls addiction, the goal isn’t just to stop the behavior—it’s to understand what’s driving it and respond differently.
Self-management is about building awareness, creating space between feeling and action, and developing new ways to regulate distress. It’s not instant, and it’s not always easy, but it’s how control gradually shifts back to you.
The moment you recognize, “This is anxiety pushing me,” is the moment you begin to take that control back.
Supporting Through the Cycle: How Families Can Help When Anxiety Drives Addiction
When someone you care about is struggling with addiction, it’s easy to focus only on the behavior—what they’re using, how often, and the consequences that follow. But in many cases, addiction isn’t just about the substance or habit. It’s about anxiety.
Understanding that anxiety often drives addictive behavior can change how families respond. Instead of seeing only poor choices or lack of willpower, you begin to see a pattern: distress, urgency, and a learned need for relief. That shift in perspective is where more effective support begins.
See the Behavior for What It Is
Addiction frequently functions as a coping mechanism. When anxiety spikes, the person may feel overwhelmed, restless, or emotionally flooded. The substance or behavior becomes a means of regulating that intensity.
This doesn’t make the behavior harmless—but it does make it understandable.
When families recognize that addiction is often an attempt to manage internal distress, responses can shift from:
- “Why are you doing this?”
to - “What are you feeling right now?”
That one change can open the door to more productive conversations.
Avoid the Trap of Misguided “Tough Love”
Many families are told that being stricter, more confrontational, or more controlling will force change. In reality, these approaches can sometimes increase anxiety, making the cycle worse.
When anxiety rises, the urge to escape rises with it.
This doesn’t mean there should be no boundaries. It means that how those boundaries are communicated matters. Support that feels like rejection, shame, or pressure can unintentionally reinforce the very behavior it’s trying to stop.
Communicate in a Way That Reduces Anxiety
The goal of communication isn’t just to express concern—it’s to lower defensiveness and create safety.
Helpful approaches include:
- Speaking calmly and directly rather than emotionally escalating
- Focusing on observations instead of accusations
- Using language like “I’m concerned about how you’re feeling” instead of “You need to stop.”
When anxiety decreases, the person is more able to reflect, listen, and consider change.
Encourage Healthier Coping—Without Forcing It
You can’t control someone else’s behavior, but you can influence the environment around them.
Families can:
- Encourage professional help (therapy, counseling, support groups)
- Model healthy coping strategies themselves
- Offer alternatives during stressful moments (walks, conversations, shared activities)
The key is to offer, not force. Pressure often increases resistance, especially when anxiety is already high.
Set Boundaries That Support, Not Punish
Boundaries are essential—but they should be clear, consistent, and grounded in self-respect rather than punishment.
For example:
- “I’m here to support you, but I can’t support behaviors that harm you or the household.”
- “I’m willing to help you get support, but I won’t ignore what’s happening.”
Healthy boundaries reduce chaos without increasing emotional intensity. They create structure, which can actually lower anxiety over time.
Take Care of Your Own Emotional Health
Supporting someone through addiction is stressful. Families often experience their own anxiety, frustration, and burnout.
Managing your own emotional state is not selfish—it’s necessary.
This might include:
- Seeking your own support (therapy, groups, education)
- Learning about anxiety and addiction dynamics
- Setting limits on what you can and cannot control
When you are more regulated, your support becomes more effective.
Final Thought
When anxiety is driving addiction, the goal isn’t just to stop the behavior—it’s to understand what’s underneath it.
Families play a powerful role, not by controlling or fixing, but by creating an environment that reduces anxiety, supports healthier coping, and encourages change without escalating the cycle.
You don’t have to have perfect answers. But understanding the connection between anxiety and addiction allows you to respond in a way that helps, rather than unintentionally harms.
And sometimes, that shift makes all the difference.
Healing Together: Community Resources for Anxiety and Addiction
Addiction is often treated as an individual problem—something a person must overcome through willpower or personal change. But when anxiety is driving that addiction, the picture becomes more complex. Anxiety thrives in isolation, uncertainty, and lack of support. That’s why community resources are not just helpful—they’re essential.
Understanding how anxiety fuels addiction helps communities respond more effectively. Instead of focusing solely on stopping behavior, community strategies aim to reduce underlying distress and provide healthier, more accessible ways to cope.
Why Community Matters
Anxiety narrows a person’s world. It can lead to withdrawal, avoidance, and disconnection. Addiction often fills that gap, offering temporary relief and a sense of control.
Community resources work in the opposite direction. They:
- Increase connection
- Provide structure and consistency
- Offer alternative coping tools
- Reduce stigma and isolation
In short, they address both the emotional and environmental factors that sustain the anxiety–addiction cycle.
Expanding Access to Mental Health Support
One of the most effective community strategies is improving access to mental health care. When anxiety goes untreated, people are more likely to self-medicate.
Communities can support this by:
- Offering low-cost or sliding-scale counseling services
- Integrating mental health care into primary care settings
- Providing school- and workplace-based support programs
Making help accessible reduces the need to rely on harmful coping mechanisms.
Peer Support and Shared Experience
There is something powerful about being understood by someone who has been through a similar experience.
Peer support groups—whether focused on anxiety, addiction, or both—provide:
- Validation (“I’m not the only one”)
- Practical coping strategies
- Accountability in a non-judgmental setting
These spaces reduce shame, which is a major driver of both anxiety and addictive behavior.
Education and Awareness
Misunderstanding addiction as purely a choice or moral failing increases stigma and prevents people from seeking help.
Community education efforts can:
- Explain the link between anxiety and addiction
- Teach early warning signs of self-medication
- Promote healthier coping strategies
When communities understand the “why” behind behavior, responses become more supportive and less reactive.
Creating Safe and Structured Environments
Not everyone has access to a stable, low-stress environment—and that matters.
Community programs can help by offering:
- Safe spaces for youth and adults
- Structured activities (sports, art, volunteering)
- Opportunities for routine and purpose
Structure reduces uncertainty, which in turn lowers baseline anxiety.
Crisis Support and Early Intervention
When anxiety becomes overwhelming, immediate support can prevent escalation into harmful behaviors.
Communities can provide:
- Crisis hotlines and text services
- Walk-in mental health centers
- Mobile crisis response teams
Early intervention helps break the cycle before addiction becomes more deeply established.
Reducing Barriers to Recovery
Even when people want help, barriers like cost, transportation, and stigma can get in the way.
Effective community strategies address these barriers by:
- Offering transportation assistance
- Providing childcare during treatment
- Creating inclusive, non-judgmental spaces
The easier it is to access support, the more likely people are to use it.
Final Thought
When anxiety controls addiction, the solution isn’t just individual—it’s collective.
Communities can reduce isolation, increase access to care, and create environments that support healthier coping. By addressing the anxiety underneath addiction, rather than just the behavior itself, communities can play a critical role in long-term recovery.
No one overcomes this cycle entirely alone. And they shouldn’t have to.
Frequently Asked Questions
Here are some common questions:
1. How does anxiety lead to addiction?
Anxiety creates a strong internal discomfort that the brain wants to escape. When a person discovers that a substance or behavior (like alcohol, vaping, or scrolling) reduces that feeling—even temporarily—the brain learns to repeat it. Over time, this pattern becomes automatic, turning coping into dependence.
2. Is addiction always about pleasure?
No. Many people assume addiction is about chasing a “high,” but in reality, it is often about escaping discomfort. For individuals with anxiety, the goal is usually relief, not pleasure.
3. Why does the relief from substances not last?
The relief is temporary because it doesn’t address the root cause—anxiety. Once the effect wears off, anxiety often returns stronger, which leads to repeated use and reinforces the cycle.
4. What is the anxiety–addiction cycle?
It’s a repeating loop:
- Anxiety increases
- A substance or behavior is used for relief
- Temporary relief occurs
- The brain learns this pattern
- Anxiety returns, often stronger
This loop makes it harder to stop over time.
5. Can anxiety make addiction harder to quit?
Yes. Anxiety increases cravings and makes discomfort feel more intense. When someone tries to stop, they may experience heightened anxiety, which pushes them back toward the behavior for relief.
6. What are the signs that anxiety is driving addiction?
- Using something mainly when feeling stressed or overwhelmed
- Feeling relief at first, then needing more over time
- Increased anxiety when trying to stop
- Constant worry about access, use, or consequences
7. Is self-medication the same as addiction?
Not exactly. Self-medication is using substances or behaviors to cope with emotions. It can lead to addiction if it becomes the primary or repeated way of managing anxiety.
8. Why does the brain rely on these behaviors so quickly?
The brain is wired for efficiency. If something quickly reduces discomfort, it tags it as a “solution.” Anxiety speeds up this learning process because the need for relief feels urgent.
9. Can you break the cycle without addressing anxiety?
It’s much harder. If anxiety remains untreated, the urge to escape it will continue. Long-term change usually requires learning healthier ways to manage anxiety directly.
10. What are healthier alternatives to cope with anxiety?
- Naming and understanding emotions
- Breathing and grounding techniques
- Physical movement
- Talking to someone or journaling
- Structured routines and sleep habits
These don’t provide instant relief like substances do, but they promote long-term regulation.
11. How can family or friends help?
They can:
- Focus on understanding, not just behavior
- Communicate calmly and without judgment
- Encourage support and healthy coping
- Set clear, supportive boundaries
Reducing anxiety in the environment can reduce the need for escape.
12. Is recovery possible if anxiety is the main driver?
Yes. In fact, recognizing anxiety as the root can make recovery more effective. When people learn to manage anxiety in healthier ways, the need for addictive behaviors often decreases.
13. Why does anxiety sometimes get worse after stopping a substance?
Because the brain has become used to external regulation. When that is removed, anxiety can temporarily spike until the brain relearns how to regulate itself naturally.
14. What is the most important takeaway?
Addiction is often less about the substance and more about what it does for the person emotionally. When anxiety is understood and managed, the cycle of addiction becomes easier to break.
Conclusion
Recognizing the role anxiety plays in addiction changes how we approach both prevention and recovery. Addiction is not always about seeking pleasure—it is often about avoiding discomfort. When anxiety remains unaddressed, the cycle of temporary relief and repeated use continues. Breaking that cycle requires more than willpower; it requires awareness, healthier coping strategies, and supportive environments that reduce emotional distress. By focusing on anxiety as a driving force, individuals, families, and communities can respond more effectively—creating pathways toward long-term stability rather than short-term escape.
Video: