West Virginia has stayed in the headlines for a tough reason: it currently has the highest overdose death rate in the United States. The opioid crisis has hit every corner of the country, but the impact in West Virginia is especially intense, touching families and communities in deep and lasting ways. I want to break down what’s happening, why things have gotten so bad, and what efforts are underway to bring hope and help to the state.
Understanding the Overdose Death Rate in West Virginia
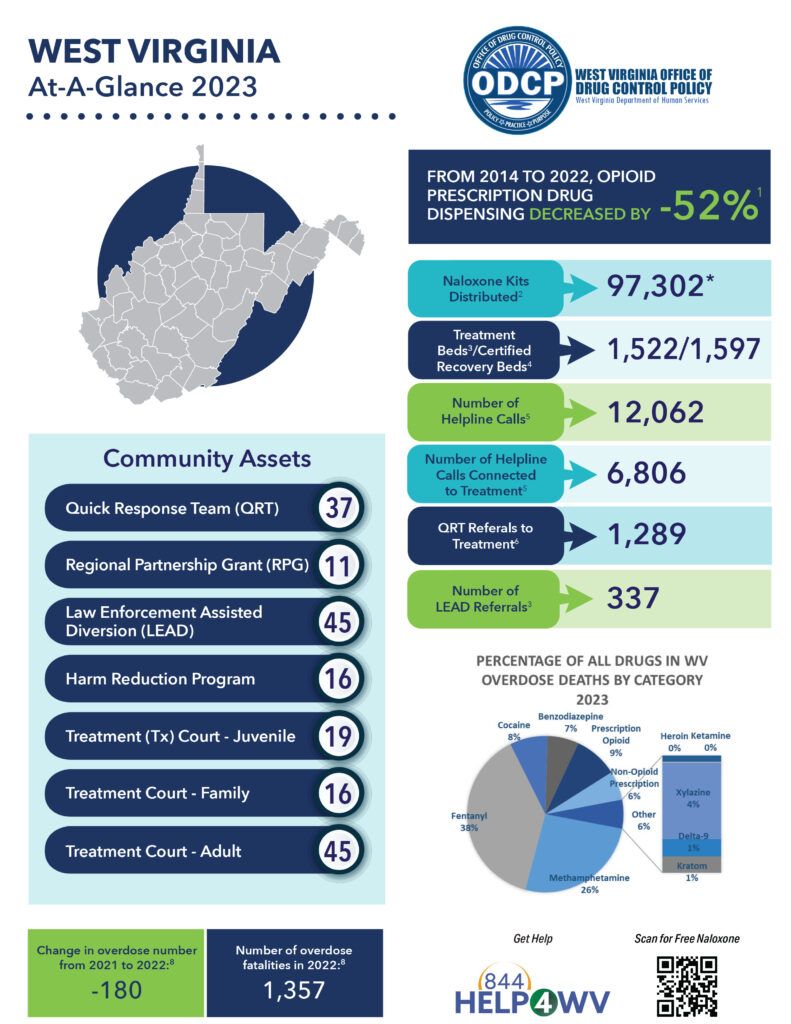
The numbers are hard to ignore. According to the Centers for Disease Control and Prevention (CDC), West Virginia’s overdose death rate is the highest in the nation, with recent figures putting it at about 81 deaths per 100,000 residents in one year. This is several times the national average. Opioids, especially synthetic drugs like fentanyl, are the main drugs driving these numbers; however, methamphetamine and other substances also play a role.
Drug overdoses don’t affect just one age group or economic class. In West Virginia, nearly every community has felt the sting, from rural villages in the mountains to busier city areas. Many families are dealing with loss, and entire neighborhoods work hard to respond. With a population of just under 2 million, each overdose death leaves a mark that’s felt far beyond numbers on a page. Drug-related loss does not exist in a vacuum; it echoes throughout extended families and local businesses, too, creating a cycle of grief the whole state must face.
Why West Virginia Is Hit So Hard
There isn’t one single reason West Virginia has been hit so much harder than other states, but several factors combine to create this difficult reality.
- Economic Switch Ups: The decline of industries like coal mining and manufacturing led to job losses and a sense of instability in many towns. When people are anxious about their future or struggling financially, drug use sometimes fills the gap.
- Prescription Patterns: In the early 2000s, painkillers were prescribed widely in West Virginia. For a while, the number of pills distributed was unbelievably high compared to other states. Many people became dependent, and when tighter controls shut off that flow, some turned to illegal opioids.
- Geography and Isolation: With many remote areas and a lack of easy access to healthcare, it’s pretty tough for some folks to get regular medical help or support for addiction. Long distances and rural settings can mean services are hard to reach.
- Social and Family Factors: Generational poverty and family disruption can add to a feeling of hopelessness or disconnect, sometimes fueling substance use as a form of escape or coping.
This combination stacks up and creates a serious challenge. The drug overdose crisis in West Virginia is part of a larger trend happening nationwide, but the numbers are especially high here because of how these factors mix together. Long-term poverty, the decline of key industries, and relative isolation set the stage for the crisis. While the opioid epidemic has swept through all states, West Virginia’s particular mix of social, economic, and geographic hurdles makes it a hotspot for overdose deaths.
How the Crisis Impacts Everyday Life
When overdose deaths climb this high, life changes for everyone in the region. Here are just a few ways I’ve noticed the issue touching regular folks and communities all over West Virginia:
- Loss in Families: Almost everyone knows someone who’s struggled with addiction or lost their life. The grief and shock ripple through whole families and friend groups, often leading to long-term emotional strain and hardship.
- Healthcare Stretched Thin: Hospitals, emergency rooms, and paramedics are constantly responding to overdoses, sometimes seeing the same people over and over. Resources for other health needs get squeezed.
- Schools and Children: Kids are deeply affected, whether through losing a parent, being raised by grandparents, or seeing the effects of addiction in their communities. These kids often need extra support from counselors, teachers, and sometimes social services just to feel safe.
- Workforce and Local Economy: Employers struggle to find people who can pass drug tests, making it tough for businesses to operate and driving economic hardship higher. Job loss and poverty worsen the impact, and a smaller, struggling workforce can undermine town stability in the long term.
These challenges may sound overwhelming, but people in West Virginia are resilient. There are plenty of stories about neighbors rallying together, organizations stepping up, and small acts of support making a big difference. Community events, local church drives, and volunteer-run recovery groups are stepping up in dozens of counties, determined to keep hope alive.
What Drugs Are Driving the Crisis?
Opioids lead the way, but it’s not just one drug at fault. Here’s a breakdown of substances that show up most often in overdose statistics in West Virginia:
- Fentanyl: This extremely powerful synthetic opioid is responsible for a large number of overdose deaths because it’s easy to overdose, and it often shows up mixed with other street drugs.
- Prescription Painkillers: Oxycodone and hydrocodone were prescribed heavily for years, setting the stage for opioid dependency.
- Methamphetamine: While not always causing fatal overdoses on its own, “meth” use has increased a lot, creating more layers of risk, especially when mixed with opioids.
- Heroin: Some folks who got addicted to prescription opioids switched to heroin after prescriptions dried up.
Often, people who overdose have more than one drug in their system. That’s because drugs like fentanyl are sometimes mixed into other substances without the user knowing, making each dose potentially deadly. This unintentional mixing creates a hidden danger, as users often don’t realize how strong or risky a batch really is.
Responding to the Overdose Epidemic
Communities, health workers, and leaders all across West Virginia are working hard to turn the tide. These are some of the main responses happening right now:
- Naloxone Distribution: Naloxone, often called Narcan, can reverse opioid overdoses if given in time. Making Narcan widely available is saving lives. First responders, family members, and even community organizations carry it constantly and offer brief trainings so more people know how to use it.
- Treatment Expansion: Increasing treatment options, including medication-assisted treatment (MAT) like suboxone and methadone, gives people a better shot at recovery. More clinics and user-friendly programs are popping up, though demand is still higher than supply in most towns.
- Peer Recovery Networks: Folks who have lived through addiction are using their experience to help others start their recovery. Peer coaches, recovery groups, and support centers add hope and connection for those just starting out.
- Community Coalitions and Education: Schools, churches, and local groups are offering prevention education, family support, and safe spaces for open conversations about substance use.
It’s an uphill battle, but all of these actions give more people a legitimate shot at help and hope. On top of that, families, nonprofit groups, and government measures have all stepped up in recent years to fast-track the deployment of proven interventions and raise awareness about substance risks.
What’s Getting in the Way of Recovery?
Despite new efforts to make it easy for people to find help, plenty of barriers make it tough for people in West Virginia to get or stick with support for substance use disorders.
- Stigma: Fear of being judged or blamed stops some folks from seeking help, whether from friends, family, or healthcare providers. This stigma can extend to employment, law enforcement, and even within medical settings, keeping people isolated.
- Lack of Access: Even with recent improvements, many places still have long waitlists or require long drives for treatment. Transportation and cost are major hurdles, especially in rural areas where the nearest clinic may be over an hour away, and public transportation is limited.
- Mental Health Challenges: Depression, anxiety, and trauma often go hand in hand with addiction. There usually aren’t enough mental health services to go around, and many areas compete for just a handful of providers.
- Legal Issues: People with a criminal record or on probation sometimes avoid treatment out of legal fears, while others cycle in and out of jail with little access to recovery programs.
Understanding these hurdles helps explain why simply “wanting to get clean” isn’t always enough. The system needs to keep stretching to meet people where they are, reducing barriers for those most in need.
For example, some new programs are experimenting with telehealth mental health support and mobile clinics that travel to rural areas. Supporters hope this will shrink waiting lists and open doors for more folks in outlying communities who need help.
Big and Small Solutions: What’s Working?
I’ve noticed some of the most encouraging stories come from homegrown solutions and collaborations between groups in West Virginia. Here are a few highlights worth mentioning:
- Quick Response Teams: Paramedics, police, and addiction counselors sometimes team up and visit people who recently survived overdoses, offering a bridge to treatment or support within hours or days of the event. This fast follow-up increases the odds that someone will accept help while things are still fresh.
- Safe Needle Programs: These reduce disease risk and offer a point of contact for folks who might not otherwise be in touch with healthcare workers. Even when controversial, these programs create space to talk about treatment and hand out naloxone as well.
- Community Resource Centers: Spaces where people can access hygiene products, food, health screenings, and recovery support all in one place offer lifelines, especially in smaller towns. These centers also help kids impacted by addiction, giving them a safe spot to talk or get after-school meals.
- Youth Prevention Programs: Early education and positive activities for teens help push back against risk, aiming to change things for the next generation. After-school clubs, mentoring, and sports all keep kids engaged and connected.
Other states are adopting some of these strategies, showing that West Virginia isn’t just dealing with this crisis. It’s also putting out creative ideas that make a real difference for residents and could help nationwide.
Not every program succeeds on the first try, but leaders are eager to learn. Across towns big and small, there’s a sense that, working together, neighbors can spark slow but real progress against the overdose epidemic that has defined a generation.
Frequently Asked Questions
If you’re looking for simple, straightforward answers about the overdose crisis in West Virginia, here are a few questions I hear a lot:
Why is fentanyl so dangerous compared to other drugs?
Answer: Fentanyl is 50 to 100 times stronger than morphine, and even a tiny amount can cause an unpredictable, sometimes deadly, overdose; when mixed with other drugs, it takes only a small amount to be fatal.
Can someone recover from opioid addiction in West Virginia?
Answer: Absolutely, though obstacles like access and stigma exist. Many people in the state are in long-term recovery with the help of treatment programs, peer support, and community organizations. With enough encouragement, support, and persistence, recovery is possible for anyone.
How can I help if someone I care about is using drugs?
Answer: Showing support and understanding, carrying naloxone, and connecting with local resources are good places to start. Offering steady, nonjudgmental help can make a huge difference in encouraging someone to take the first step toward healing.
Looking Forward to West Virginia
The overdose crisis in West Virginia is daunting, but the determination to push back is strong. Community spirit, new approaches to treatment, and ongoing education are moving the needle in the right direction. Anyone wanting to help can contribute in various ways, from supporting local organizations to simply offering kindness to those affected. The state’s road to recovery is long, but every small step matters—and the people here refuse to give up.
For updates, resources, or to get involved, sites like the West Virginia Office of Drug Control Policy and the CDC offer reliable information and support options for anyone ready to stand with West Virginia.
Video: HIGHEST OVERDOSE DEATH RATE IN THE U S