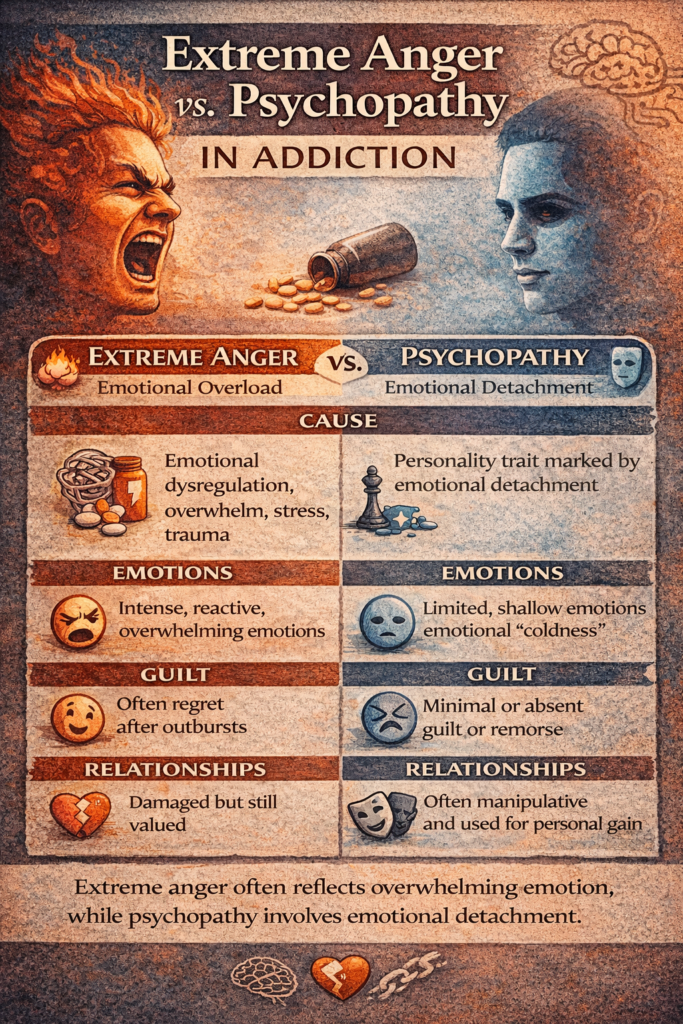
Addiction can significantly alter emotional expression and behavior, sometimes leading to intense anger, impulsivity, or emotional detachment. These changes can be confusing and concerning, often raising questions about whether such behaviors reflect deeper personality traits, such as psychopathy. However, extreme anger and psychopathy are fundamentally different psychological phenomena. While extreme anger in addiction is typically rooted in emotional overwhelm, stress, and difficulty regulating feelings, psychopathy is characterized by a persistent pattern of emotional detachment, lack of empathy, and manipulative behavior. Understanding this distinction is essential for accurately interpreting behavior, reducing stigma, and ensuring that individuals receive appropriate support and treatment.
Extreme Anger vs. Psychopathy in Addiction: Understanding the Difference
Addiction often brings intense emotional and behavioral changes, including outbursts of anger, impulsivity, and strained relationships. These reactions can sometimes be misunderstood, especially when individuals display extreme anger or appear emotionally detached. In some cases, people may even question whether these behaviors resemble psychopathy.
However, extreme anger and psychopathy are not the same, and understanding the difference is critical for both effective treatment and compassionate support. While both can involve harmful behaviors, they stem from very different psychological processes.
Understanding Extreme Anger in Addiction
Extreme anger in addiction is typically rooted in emotional dysregulation—the inability to manage intense feelings effectively.
Common causes include:
- Frustration from cravings or withdrawal
- Underlying mental health conditions (e.g., anxiety, depression)
- Trauma or unresolved emotional pain
- Stress and life instability
In this context, anger is often reactive and emotionally driven. It may appear explosive, unpredictable, or disproportionate, but it usually reflects internal distress rather than a lack of emotion.
What Is Psychopathy?
Psychopathy is a personality construct characterized by:
- Lack of empathy
- Shallow or absent emotional responses
- Manipulative or deceitful behavior
- Reduced guilt or remorse
Unlike anger in addiction, psychopathy is not primarily about emotional overwhelm—it is about emotional detachment and reduced emotional depth.
Key Differences Between Extreme Anger and Psychopathy
1. Emotional Experience
- Extreme Anger: Intense, overwhelming emotions
- Psychopathy: Limited or shallow emotional experience
2. Motivation Behind Behavior
- Extreme Anger: Reaction to stress, pain, or frustration
- Psychopathy: Often goal-oriented or manipulative
3. Presence of Guilt or Remorse
- Extreme Anger: Individuals often feel regret after outbursts
- Psychopathy: Minimal or no remorse
4. Relationship to Others
- Extreme Anger: Relationships may be damaged, but still valued
- Psychopathy: Relationships may be used for personal gain
Why the Confusion Happens
In addiction, behaviors such as:
- Aggression
- Irritability
- Emotional withdrawal
- Risk-taking
can resemble traits associated with psychopathy. However, these behaviors are often temporary and situational, influenced by substance use, withdrawal, or emotional distress.
This is an important distinction—incorrect labeling can lead to stigma and inappropriate treatment approaches.
The Role of Brain and Behavior Changes
Addiction affects areas of the brain responsible for:
- Impulse control
- Emotional regulation
- Decision-making
These changes can increase irritability and reduce emotional control, making anger more intense and frequent. However, this is different from the core personality traits associated with psychopathy.
Implications for Treatment and Support
Understanding the difference between extreme anger and psychopathy has important implications:
- For extreme anger:
- Focus on emotional regulation skills
- Address underlying trauma or mental health issues
- Use therapy approaches like CBT or DBT
- For psychopathic traits (when present):
- Treatment may focus on behavioral management
- Structured interventions and long-term strategies are often needed
An accurate understanding ensures individuals receive appropriate and effective care.
The Importance of Avoiding Mislabeling
Mislabeling someone as “psychopathic” when they are experiencing emotional dysregulation can:
- Increase stigma
- Reduce empathy from others
- Discourage individuals from seeking help
It is essential to view behaviors in context rather than assigning fixed labels.
Moving Toward a More Nuanced Understanding
Addiction is complex, and so are the behaviors that come with it. Extreme anger often reflects pain, overwhelm, and difficulty coping, not a lack of humanity or empathy.
Final Thought
Not all intense or harmful behavior in addiction comes from the same place.
Extreme anger is often the expression of too much emotion, while psychopathy is associated with too little emotional connection.
Understanding this difference allows for more accurate, compassionate, and effective responses—
Because behind the behavior is not just a label but a person trying to cope, survive, and ultimately heal.
Managing the Mind: Self-Strategies for Understanding Anger vs. Psychopathy in Addiction
In addiction, intense emotions and behavioral changes can often feel confusing—not only to others, but to the individual experiencing them. Extreme anger, impulsivity, and emotional withdrawal may raise concerns about deeper personality traits, including psychopathy. However, these experiences are often rooted in emotional dysregulation rather than emotional absence.
Understanding the difference between extreme anger and psychopathy is essential for self-awareness. More importantly, learning how to manage these reactions can empower individuals to take control of their emotional responses and support their recovery journey.
Building Awareness of Emotional Experience
The first step in self-management is recognizing what you are actually feeling. Extreme anger often masks deeper emotions such as:
- Hurt
- Fear
- Shame
- Frustration
Instead of identifying only the anger, ask:
- What am I really feeling underneath this?
This helps distinguish emotional overload (anger) from emotional detachment (psychopathy).
Recognizing Triggers and Patterns
Anger in addiction is often triggered by specific situations, such as:
- Cravings or withdrawal symptoms
- Conflict with others
- Feelings of loss of control
- Stress or overwhelm
Tracking these triggers through journaling or reflection helps identify patterns and anticipate reactions before they escalate.
Pausing Before Reacting
One of the most effective self-management strategies is learning to pause.
When you feel anger rising:
- Take a few deep breaths
- Step away from the situation
- Delay your response
This pause creates a gap between emotion and action, allowing for more thoughtful and controlled behavior.
Differentiating Reaction vs. Intention
Extreme anger is often reactive, while psychopathic behavior tends to be more calculated. Ask yourself:
- Am I reacting impulsively, or am I intentionally trying to manipulate?
This question builds insight into your behavior and reinforces awareness of your emotional state.
Practicing Emotional Regulation Skills
Managing anger requires developing tools to regulate emotions effectively.
Helpful strategies include:
- Mindfulness or grounding exercises
- Physical activity to release tension
- Deep breathing or progressive muscle relaxation
These techniques reduce emotional intensity and improve control.
Challenging Cognitive Distortions
Anger is often fueled by distorted thinking patterns, such as:
- “They’re against me.”
- “This always happens.”
- “I can’t handle this.”
Self-management involves questioning these thoughts:
- Is this completely true?
- Is there another way to view this situation?
Reframing thoughts can reduce emotional escalation.
Reconnecting with Empathy
One key difference between anger and psychopathy is the presence of empathy. Even during intense anger, empathy can still be accessed.
Practice:
- Considering the other person’s perspective
- Reflecting on how your actions affect others
- Asking, “How would I feel in their position?”
This strengthens emotional awareness and reduces harmful reactions.
Taking Responsibility Without Self-Judgment
After an episode of anger, it’s important to reflect without harsh self-criticism.
Instead of:
- “I’m a bad person.”
Shift to:
- “I had a strong reaction—what can I learn from it?”
This promotes growth rather than shame, which can otherwise reinforce negative patterns.
Seeking Support and Skill Development
Self-management does not mean managing everything alone. Professional support can provide structured tools for emotional regulation, such as:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavior Therapy (DBT)
- Anger management programs
These approaches help build long-term emotional skills.
The Shift from Reactivity to Control
Understanding the difference between extreme anger and psychopathy allows individuals to move away from fear-based labels and toward practical self-awareness.
Final Thought
Extreme anger in addiction is often a sign of overwhelming emotion, not a lack of feeling. Recognizing this distinction is empowering—it means the emotion can be understood, managed, and changed.
Self-management is not about eliminating anger, but about learning how to respond to it differently.
Because recovery is not just about stopping behaviors—
It’s about learning to understand and regulate the emotions behind them.
Understanding the Difference: Family Strategies for Managing Anger vs. Psychopathy in Addiction
Families often face confusion and emotional distress when a loved one struggling with addiction displays intense anger, aggression, or emotional distance. These behaviors can be alarming, sometimes leading to fears that the individual lacks empathy or is beyond help. However, it is critical to understand that extreme anger and psychopathy are not the same, and misinterpreting one for the other can affect how families respond.
In many cases, extreme anger in addiction is rooted in emotional overwhelm, stress, and underlying pain—not a lack of feeling. Recognizing this distinction allows families to respond with greater clarity, compassion, and effectiveness.
Understanding Anger as Emotional Overload
Extreme anger in addiction is often a response to:
- Internal distress (shame, guilt, frustration)
- Withdrawal symptoms or cravings
- Difficulty managing emotions
Families can reframe anger as emotional overload, rather than intentional harm or lack of care. This perspective helps reduce fear and promotes more supportive responses.
Avoiding Mislabeling and Assumptions
Labeling a loved one as “psychopathic” can create distance and reduce empathy. While some behaviors may appear cold or detached, they are often temporary and influenced by addiction.
Instead of labeling, families can ask:
- What might they be feeling underneath this behavior?
- Is this reaction situational or consistent over time?
This approach encourages understanding rather than judgment.
Responding to Anger with Calm and Consistency
When faced with intense anger, reacting with equal intensity can escalate the situation. Families can support by:
- Remaining calm and composed
- Avoiding arguments during heightened emotional moments
- Giving space when needed
Consistency helps create a sense of safety and reduces the likelihood of further escalation.
Setting Clear and Healthy Boundaries
Support does not mean accepting harmful behavior. Families must establish boundaries that protect their well-being while maintaining care.
Healthy boundaries may include:
- Refusing to engage in aggressive or abusive interactions
- Communicating limits clearly and respectfully
- Following through with consequences when necessary
Boundaries provide structure and reinforce accountability.
Encouraging Emotional Expression in Healthy Ways
Individuals struggling with anger often lack the tools to express emotions constructively. Families can encourage:
- Open conversations during calm moments
- Expression of feelings without judgment
- Use of alternative outlets (e.g., exercise, journaling)
This helps shift anger from destructive expression to constructive communication.
Recognizing Signs of Empathy
Even during periods of intense anger, individuals often still demonstrate empathy in subtle ways, such as:
- Showing regret after an outburst
- Expressing concern for others at times
- Wanting to repair relationships
Recognizing these moments reinforces the understanding that the individual is not emotionally detached but struggling to regulate emotions.
Seeking Professional Guidance
Families do not have to navigate this alone. Professional support can provide clarity and tools for both the individual and the family.
Helpful resources include:
- Family therapy
- Addiction counseling
- Anger management programs
These supports help families respond more effectively and reduce emotional strain.
Taking Care of the Family System
Supporting someone with addiction and intense anger can be exhausting. Families must also prioritize their own well-being.
This includes:
- Seeking personal support (therapy or support groups)
- Practicing self-care
- Setting emotional boundaries
A healthy family system is better equipped to provide support.
The Power of Understanding Over Fear
Distinguishing between extreme anger and psychopathy allows families to move away from fear-based reactions and toward informed, compassionate support.
Final Thought
What may look like emotional coldness is often emotional overload.
What may feel like rejection is often an internal struggle.
Families play a vital role in recognizing this difference—not to excuse harmful behavior, but to respond in ways that promote understanding, accountability, and healing.
Because behind the anger is not a lack of humanity—
but a person struggling to manage emotions they don’t yet understand or control.
And with the right support, that can change.
Community Matters: Strategies to Understand Anger vs. Psychopathy in Addiction
In communities, addiction is often misunderstood—especially when individuals display extreme anger, aggression, or emotional detachment. These behaviors can be alarming and are sometimes misinterpreted as signs of psychopathy. However, this confusion can lead to stigma, fear-based responses, and missed opportunities for effective support.
Understanding the difference between extreme anger (emotional overload) and psychopathy (emotional detachment) is essential at the community level. When communities are informed, they can respond with strategies that promote safety, compassion, and recovery rather than judgment and exclusion.
Promoting Public Education and Awareness
One of the most important community strategies is increasing awareness about the psychological differences between anger and psychopathy in addiction.
Communities can:
- Host workshops on addiction and emotional regulation
- Provide educational campaigns that explain behavioral differences
- Partner with schools and organizations to teach mental health literacy
Education reduces fear and helps people respond based on understanding rather than assumptions.
Reducing Stigma Through Accurate Information
Mislabeling individuals as “dangerous” or “psychopathic” can lead to isolation and discrimination. Community efforts should focus on:
- Promoting person-centered language
- Challenging stereotypes about addiction and aggression
- Encouraging empathy in public discourse
Reducing stigma creates an environment where individuals feel safer seeking help.
Training Community Professionals
Many frontline professionals—such as healthcare workers, educators, and law enforcement—interact with individuals experiencing addiction-related anger. Proper training can improve responses and outcomes.
Training should include:
- Recognizing emotional dysregulation vs. personality traits
- De-escalation techniques
- Trauma-informed care approaches
Well-trained professionals can respond effectively without escalating situations.
Providing Accessible Mental Health and Anger Management Services
Communities must ensure access to services that address emotional regulation and behavioral concerns.
Key resources include:
- Anger management programs
- Individual and group therapy
- Crisis intervention services
These services help individuals develop skills to manage anger and reduce harmful behaviors.
Creating Safe Spaces for Expression and Support
Safe, supportive environments allow individuals to express emotions without fear of judgment. Community-based programs can offer:
- Peer support groups
- Drop-in counseling centers
- Recovery-focused community spaces
These spaces reduce isolation and provide opportunities for healthy emotional expression.
Encouraging Peer Support and Mentorship
Peer support is particularly effective in addressing anger in addiction. Individuals with lived experience can:
- Model emotional regulation strategies
- Provide relatable guidance
- Reduce feelings of isolation
Mentorship programs help individuals feel understood and supported.
Implementing De-escalation and Conflict Resolution Programs
Communities can reduce harm by promoting de-escalation strategies in public and organizational settings.
This includes:
- Conflict resolution workshops
- Training in communication skills
- Programs that teach emotional regulation techniques
These initiatives help prevent situations from escalating into harmful encounters.
Collaborating Across Community Systems
Effective support requires coordination between:
- Healthcare providers
- Social services
- Schools and workplaces
- Law enforcement
Collaboration ensures that individuals receive consistent and comprehensive support, rather than fragmented responses.
Encouraging Early Intervention
Recognizing and addressing emotional dysregulation early can prevent escalation. Community strategies include:
- Screening programs in schools and clinics
- Outreach initiatives for at-risk individuals
- Early access to counseling and support services
Early intervention improves long-term outcomes and reduces the likelihood of severe behavioral issues.
The Role of Community in Changing Narratives
Communities shape how behaviors are interpreted. By shifting the narrative from “dangerous behavior” to “understandable response to distress,” communities can foster more constructive and supportive approaches.
Final Thought
Extreme anger in addiction is often a signal of distress, not a sign of emotional absence. When communities understand this distinction, they move from fear and judgment to informed action and compassionate support.
Because communities don’t just respond to behavior—
They shape how it is understood.
And when understanding improves,
So does the path to recovery.
Frequently Asked Questions
Here are some common questions:
1. What is the difference between extreme anger and psychopathy in addiction?
Extreme anger is typically a result of emotional overload and poor regulation, while psychopathy involves emotional detachment, lack of empathy, and shallow emotional responses.
2. Why do people with addiction experience extreme anger?
Extreme anger can stem from:
- Withdrawal symptoms
- Stress and frustration
- Underlying trauma or mental health issues
- Difficulty managing emotions
It is usually a reaction to internal distress.
3. Does extreme anger mean someone lacks empathy?
No. Individuals experiencing extreme anger often still have empathy but may struggle to express it during emotional overwhelm. They may feel guilt or regret after outbursts.
4. What are the key traits of psychopathy?
Psychopathy is characterized by:
- Lack of empathy
- Minimal guilt or remorse
- Manipulative behavior
- Shallow emotional responses
These traits are typically consistent over time, not just situational.
5. Why can addiction-related behavior be mistaken for psychopathy?
Addiction can cause:
- Irritability
- Emotional withdrawal
- Impulsive or harmful behavior
These can resemble psychopathic traits, but they are often temporary and context-driven.
6. How does the brain play a role in anger during addiction?
Addiction affects brain areas involved in:
- Emotional regulation
- Impulse control
- Decision-making
This can increase emotional intensity and reduce the ability to manage anger effectively.
7. Do people with extreme anger feel remorse?
Yes. Most individuals with anger issues in addiction feel guilt or regret after their behavior, which is a key difference from psychopathy.
8. Can someone have both addiction and psychopathic traits?
Yes, it is possible, but it is less common. Proper assessment by professionals is needed to distinguish between personality traits and addiction-related behaviors.
9. How can someone tell if their anger is a problem?
Signs include:
- Frequent outbursts
- Difficulty controlling reactions
- Damage to relationships
- Regret after episodes
These indicate a need for emotional regulation support.
10. How is extreme anger treated in addiction recovery?
Treatment may include:
- Therapy (CBT or DBT)
- Anger management programs
- Addressing underlying trauma or mental health issues
11. Can psychopathy be treated the same way as anger issues?
No. Psychopathy requires different approaches, often focusing on behavioral management and long-term structured interventions, rather than emotional regulation alone.
12. How should families respond to extreme anger?
Families should:
- Stay calm and avoid escalation
- Set clear boundaries
- Encourage professional help
- Do not take the behavior personally
13. Why is it harmful to label someone as “psychopathic”?
Mislabeling can:
- Increase stigma
- Reduce empathy from others
- Lead to inappropriate treatment approaches
Understanding behavior in context is more helpful.
14. What role does empathy play in distinguishing the two?
Empathy is a key difference:
- Extreme anger: Empathy is present but overwhelmed
- Psychopathy: Empathy is significantly reduced or absent
15. What is the most important takeaway?
The key takeaway is that extreme anger in addiction is usually a sign of too much emotion, not too little. Recognizing this helps guide more effective and compassionate responses.
Conclusion
Distinguishing between extreme anger and psychopathy in addiction is crucial for fostering both effective intervention and compassionate understanding. Misinterpreting emotionally driven reactions as signs of psychopathy can lead to unnecessary labeling, increased stigma, and less effective support strategies. In reality, extreme anger often reflects underlying distress, trauma, or impaired emotional regulation—factors that can be addressed through appropriate care and intervention. By recognizing the difference, individuals, families, and communities can respond with greater clarity and empathy, supporting recovery in ways that focus on healing rather than judgment. Ultimately, understanding the roots of behavior is a key step toward meaningful change and long-term recovery.
Video: