Addiction is often mistaken for poor judgment or a lack of willpower, but this view misses a critical reality: it is as much a physical condition as it is a psychological one. It changes brain chemistry, disrupts the nervous system, and alters how the body processes stress, reward, and everyday functioning. What may look like repeated bad choices from the outside is often driven by deeply rooted physiological changes that make stopping feel not only difficult but also physically unsettling. To truly understand addiction—and respond to it effectively—we must move beyond blame and recognize the real, lived experience happening within the body.
The Physical Reality of Addiction: When the Body Becomes the Battlefield
Addiction is often described as a mental struggle—a failure of willpower, a cycle of poor decisions, or a psychological dependence. But this framing misses something critical: addiction is deeply physical. It lives in the body just as much as it lives in the mind.
To understand addiction fully, you have to understand what it does beneath the surface—inside the brain, the nervous system, and even the cells themselves.
🧠 The Brain on Addiction
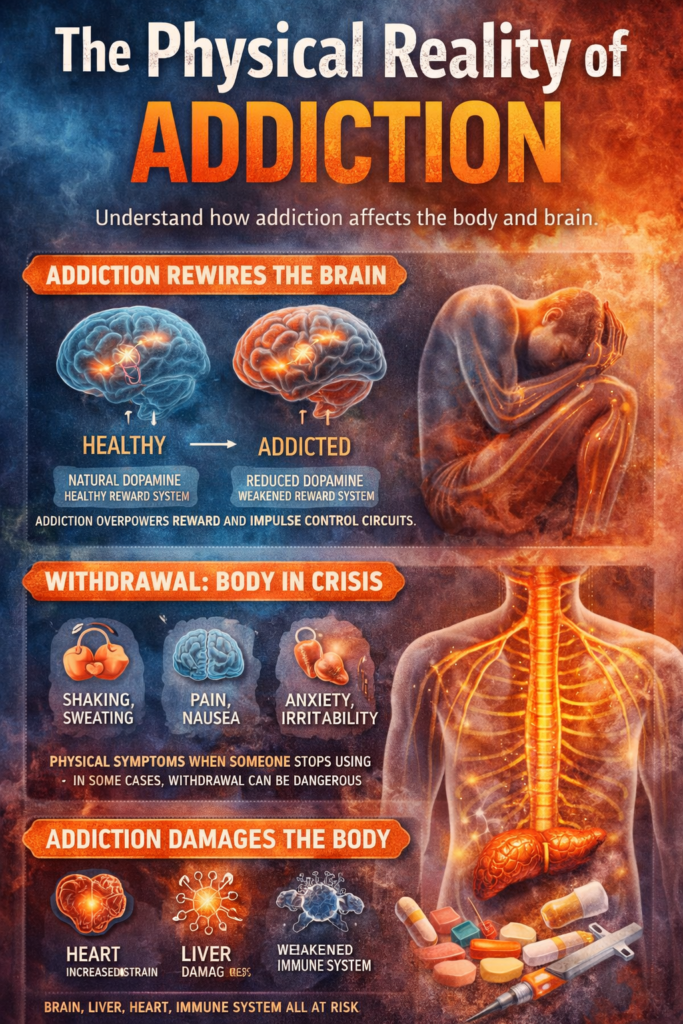
At its core, addiction rewires the brain’s reward system. Substances and behaviors flood the brain with dopamine—the chemical associated with pleasure and reinforcement.
Over time:
- The brain produces less natural dopamine
- Receptors become less sensitive
- Every day pleasures feel flat or meaningless
This is why addiction isn’t just about “wanting” something—it’s about needing it to feel normal.
The prefrontal cortex (responsible for decision-making and impulse control) also becomes less effective. Meanwhile, the limbic system (emotion and reward) becomes more dominant. The result? Cravings overpower logic.
⚡ Withdrawal: When the Body Pushes Back



When someone stops using, the body doesn’t simply “reset.” It reacts—often intensely.
Withdrawal symptoms can include:
- Sweating, shaking, nausea
- Insomnia and exhaustion
- Anxiety, irritability, depression
- Physical pain that feels flu-like—or worse
These symptoms aren’t imagined. They’re the body struggling to rebalance after adapting to a substance. In some cases (like alcohol or benzodiazepines), withdrawal can even be life-threatening.
This is one reason quitting isn’t just a decision—it’s a physiological process.
🫀 The Body Keeps the Score

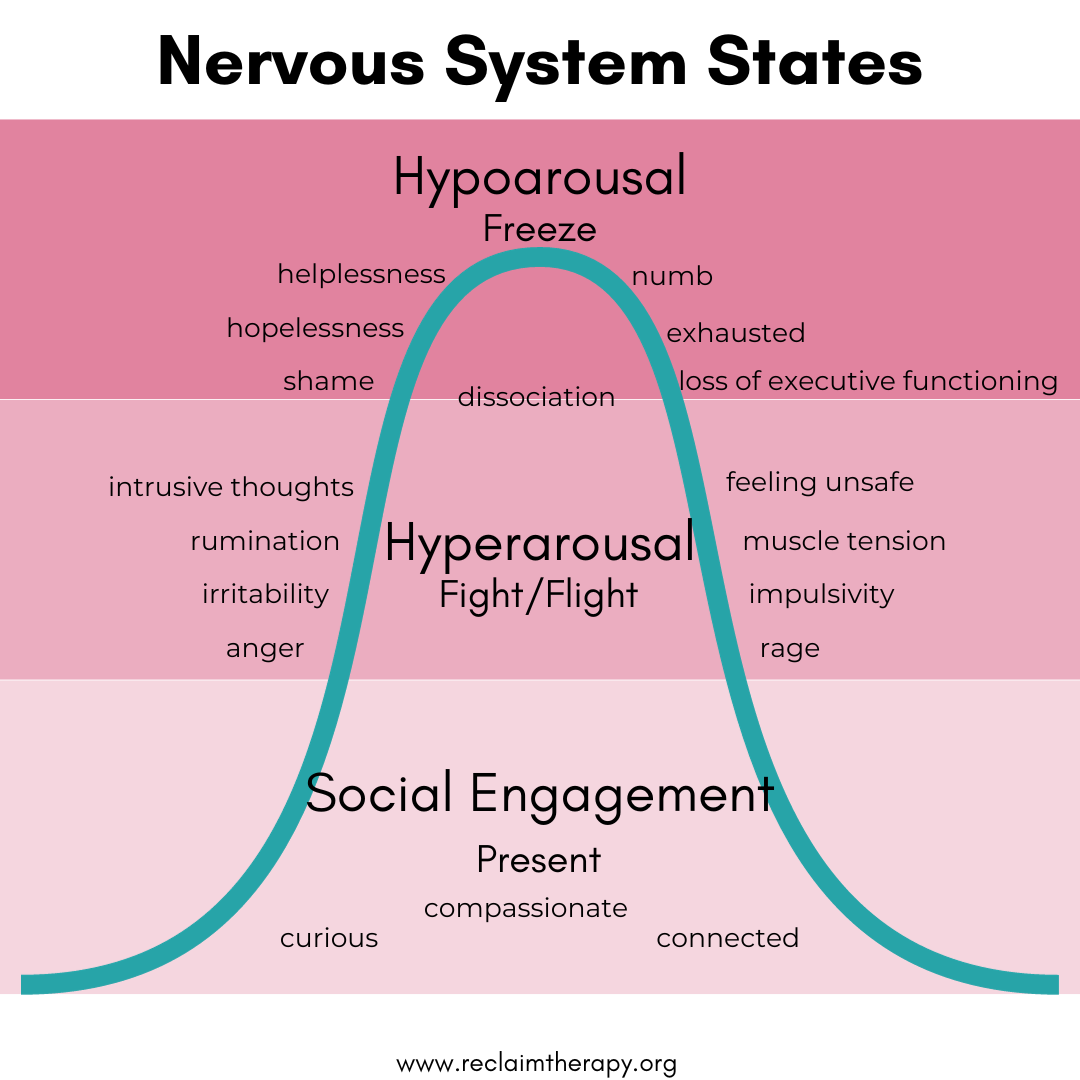
Addiction affects far more than the brain. It impacts the entire body:
- Heart: increased strain, irregular rhythms
- Liver: damage from toxins (especially alcohol)
- Sleep cycles: disrupted or fragmented
- Hormones: chronic stress response (elevated cortisol)
- Immune system: weakened over time
The nervous system becomes dysregulated, often stuck in fight-or-flight. This is why many people in addiction feel constantly on edge—or completely shut down.
🔁 Why It Feels Impossible to Stop
Understanding the physical side of addiction helps explain a painful truth: stopping isn’t just about “trying harder.”
When the brain has adapted, and the body depends on a substance to function, quitting can feel like:
- Losing your only source of relief
- Fighting your own biology
- Existing in a body that no longer feels stable
This isn’t a weakness. It’s physiology.
🌱 Healing Is Physical Too
The hopeful part? Recovery is also physical.
As sobriety continues:
- Dopamine systems begin to rebalance
- Sleep slowly restores
- The nervous system becomes more regulated
- The body relearns how to feel pleasure naturally
But this takes time. And during that time, support, structure, and compassion are essential.
💬 Final Thoughts
Addiction is not just in someone’s head—it’s in their brain, their body, their nervous system. It’s lived, felt, and endured physically.
When we start to see addiction this way, something shifts. Judgment gives way to understanding. Shame gives way to compassion.
Because recovery isn’t just about changing your mind—it’s about healing your body.
Learning Your Body Again: Self-Management Strategies for Understanding the Physical Reality of Addiction
Addiction isn’t just something you think about—it’s something you feel. In your chest, your gut, your sleep, your energy, your cravings.
If recovery is going to last, it’s not enough to “stay strong.” You have to learn how your body works again—how it reacts, what it needs, and what it’s trying to tell you.
Self-management isn’t about control in a harsh, rigid way. It’s about awareness, regulation, and rebuilding trust with your own body.
🧠 Start With Body Awareness, Not Judgment
One of the most powerful skills in recovery is interoception—your ability to notice internal body signals.
Instead of immediately reacting to a craving or discomfort, pause and ask:
- What am I actually feeling in my body right now?
- Is this tension, emptiness, restlessness, fatigue?
- Where do I feel it?
This shift—from reacting to observing—creates space. And that space is where change begins.
⚡ Learn Your Triggers as Physical Signals


Triggers aren’t just thoughts like “I want to use.” They often show up physically first:
- Tight chest
- Restlessness
- Sudden fatigue or agitation
- That “buzz” or urge in your body
These are early warning signals.
A practical strategy:
- Treat cravings like waves (often called urge surfing)
- Notice them rise, peak, and pass—without acting on them
Cravings are temporary, even when they feel overwhelming.
🫁 Regulate the Nervous System (Not Just Your Thoughts)
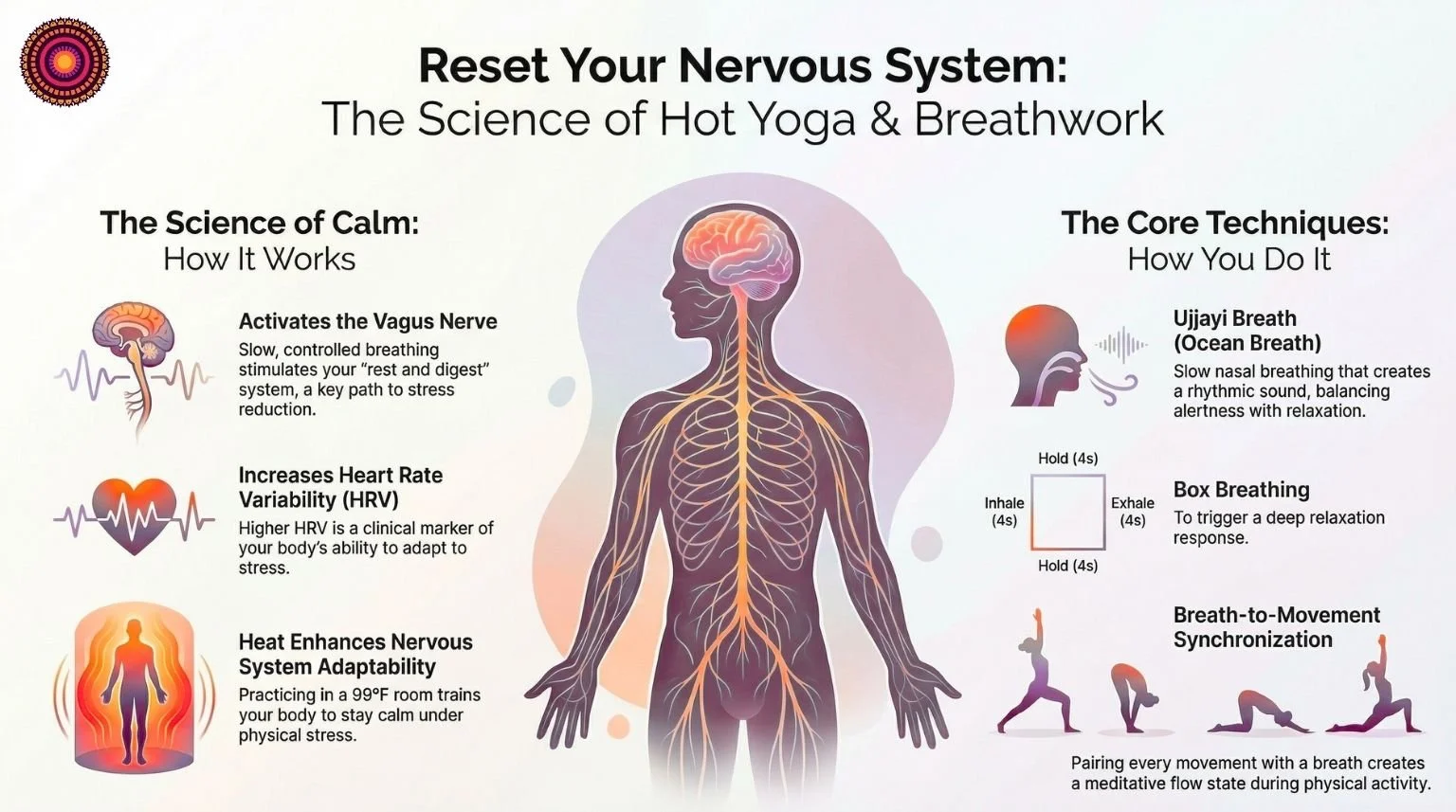

Addiction dysregulates the nervous system. So recovery has to re-regulate it.
Instead of trying to “think your way out” of distress, use the body:
Simple tools:
- Slow breathing (inhale 4, exhale 6)
- Cold water on your face or hands
- Grounding (naming 5 things you see, 4 you feel, etc.)
- Gentle movement (walking, stretching)
These techniques signal safety to your body, which reduces the intensity of cravings and emotional spikes.
🛌 Stabilize the Basics First



Recovery is built on physical stability.
Focus on:
- Sleep → even if imperfect, aim for consistency
- Nutrition → regular meals stabilize blood sugar and mood
- Hydration → dehydration can mimic anxiety and cravings
- Routine → predictability helps the nervous system relax
These may seem basic, but they are foundational. A dysregulated body struggles to make clear decisions.
🔁 Track Patterns, Not Perfection
Instead of asking, “Did I mess up?” ask:
- When are cravings strongest?
- What was happening in my body before that?
- What helped—even a little?
Keep it simple: a few notes each day can reveal patterns over time.
Self-management is not about being perfect. It’s about becoming informed.
🌱 Rebuild Trust With Your Body
For many people, addiction creates a disconnect:
- You stop trusting your feelings
- Your body feels unpredictable or unsafe
Recovery is the process of reconnecting.
Each time you:
- Notice, instead of React
- Regulate instead of escape
- Care for your body instead of overriding it
…you rebuild that trust.
💬 Final Thoughts
Understanding the physical reality of addiction changes everything.
It moves recovery from “Why can’t I just stop?” to
“What is my body going through—and how can I support it?”
Self-management isn’t about controlling yourself into sobriety.
It’s about learning your signals, supporting your system, and working with your body instead of against it.
Because healing doesn’t just happen in the mind—
It happens in the body, one regulated moment at a time.
Loving Someone Through It: Family Support Strategies for Understanding the Physical Reality of Addiction
When someone you love is struggling with addiction, it’s easy to interpret their behavior as choices—bad decisions, broken promises, or lack of effort.
But addiction is not just behavioral. It is physical. It affects the brain, the nervous system, and the body in ways that make stopping incredibly difficult—even when someone truly wants to.
Understanding this changes how families respond. It shifts the focus from control and frustration to support and strategy.
🧠 Learn What’s Happening in Their Body
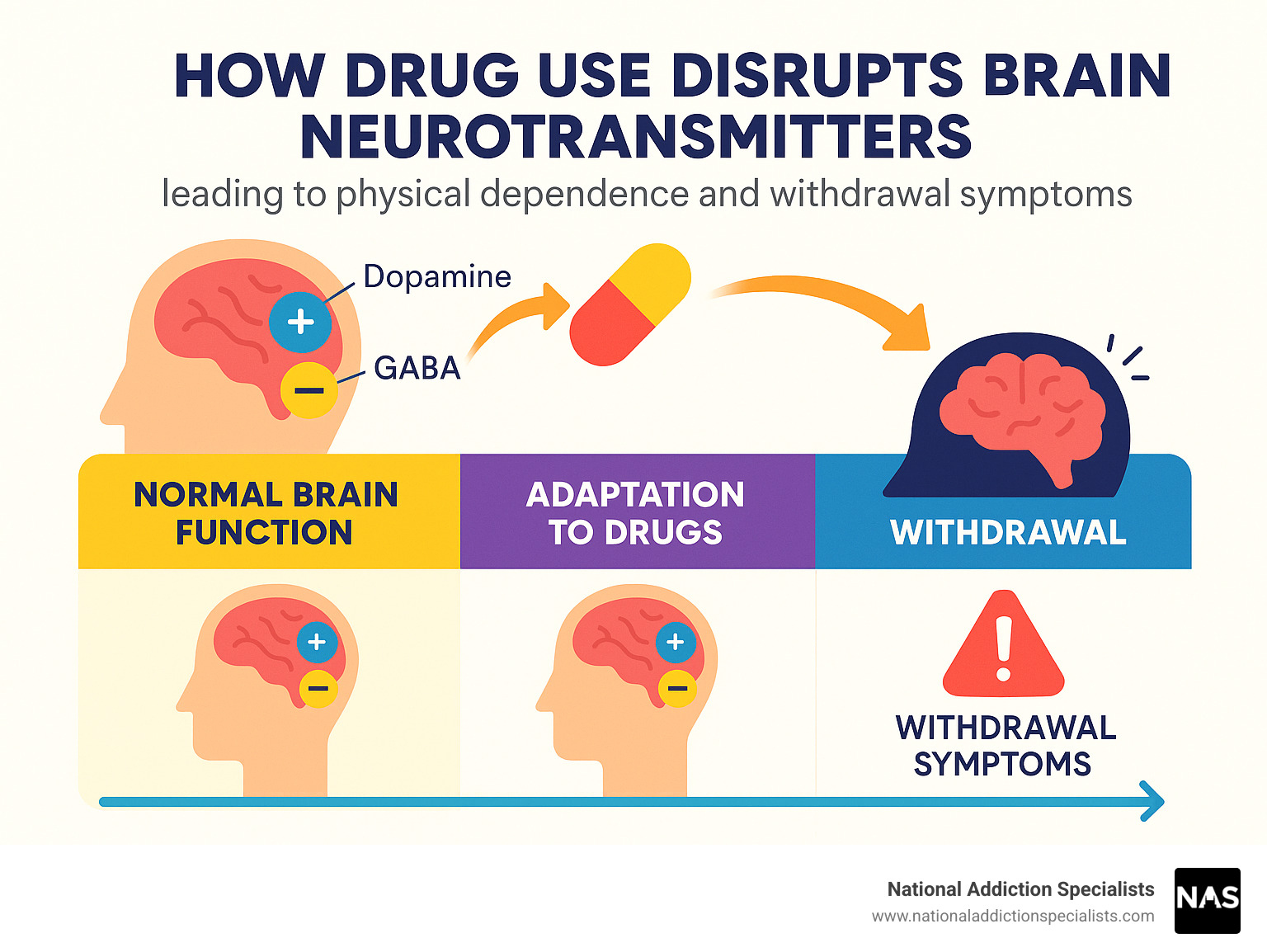
Addiction alters:
- Dopamine systems → reducing natural pleasure and motivation
- Impulse control → making it harder to resist cravings
- Stress response → keeping the body in survival mode
This means your loved one may not be choosing in the way it looks from the outside.
Family strategy:
Educate yourself about the physical side of addiction. When you understand the biology, it becomes easier to respond with clarity instead of anger.
⚡ Recognize Withdrawal as a Physical Crisis
Withdrawal can look like:
- Irritability or emotional outbursts
- Physical illness (nausea, shaking, exhaustion)
- Anxiety, panic, or depression
In some cases, it can be dangerous.
Family strategy:
Don’t personalize withdrawal behavior. The body is under stress. Support may look like:
- Encouraging medical help when needed
- Offering calm, low-stimulation environments
- Being present without escalating conflict
🫁 Help Regulate, Don’t Escalate
When someone is dysregulated, logic doesn’t work well. Their nervous system is in fight, flight, or shutdown.
Family strategy: co-regulation
- Speak calmly and slowly
- Avoid lectures during emotional intensity
- Reduce chaos (noise, arguments, pressure)
- Model steadiness instead of reacting impulsively
Your calm can help stabilize their system—this is called co-regulation.
🚧 Set Boundaries That Support, Not Punish
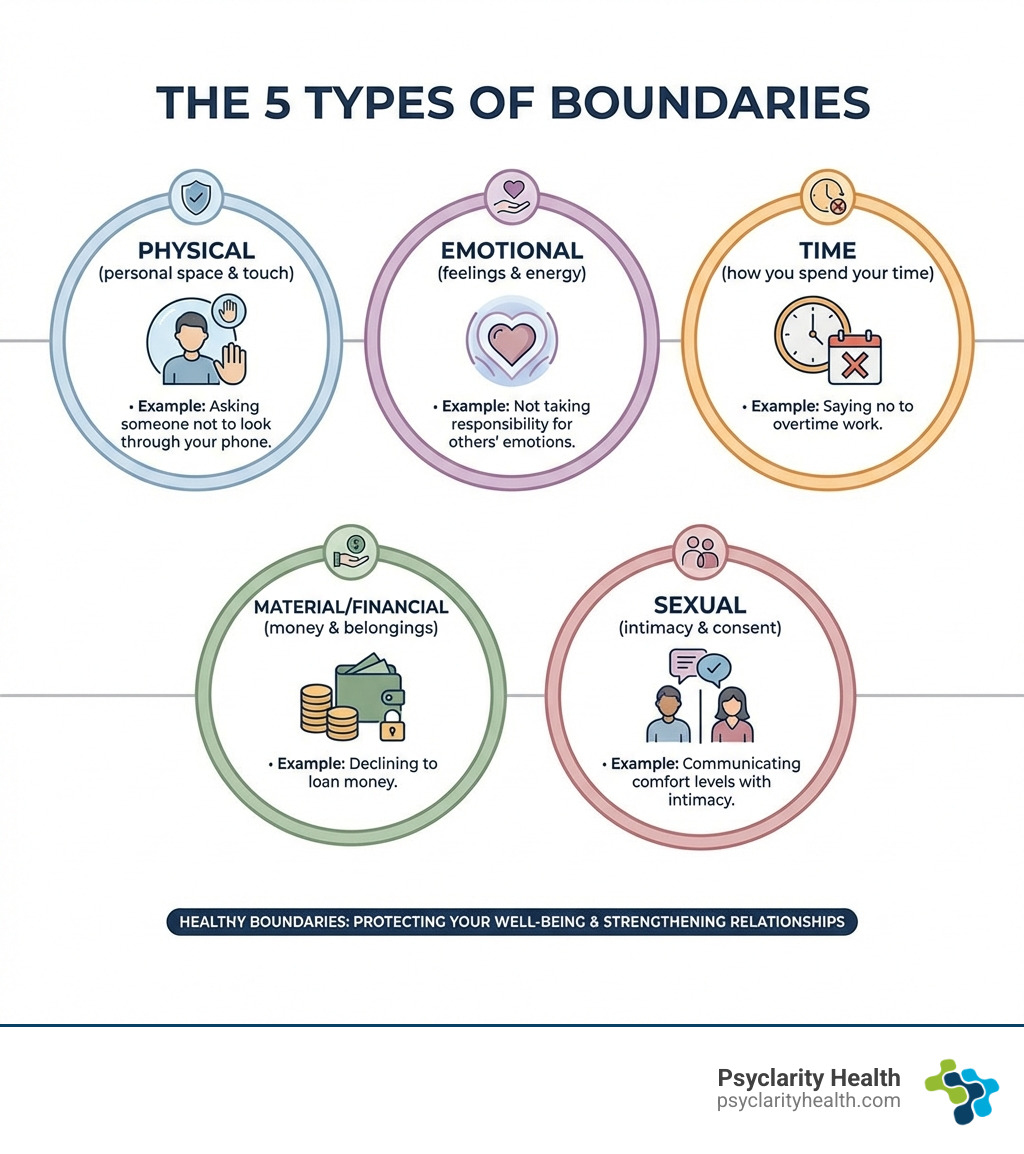
Understanding addiction physically doesn’t mean accepting harmful behavior.
Healthy boundaries might include:
- Not enabling substance use
- Protecting your time, energy, and safety
- Being clear about what you can and cannot support
Key shift:
Boundaries are not about control—they are about stability for everyone involved.
🔁 Support the Body, Not Just the Behavior
Recovery isn’t just “stop using.” It’s rebuilding physical stability.
Family strategy:
- Encourage regular meals and hydration
- Support sleep routines
- Suggest gentle activities (walks, fresh air)
- Celebrate small physical improvements
These basics help regulate the body, which makes emotional and behavioral change more possible.
💬 Communicate With Reality in Mind
Instead of:
- “Why can’t you just stop?”
Try:
- “I can see this is really hard on your body. How can I support you right now?”
Instead of:
- “You’re not trying hard enough.”
Try:
- “I know this isn’t just willpower. I’m here with you.”
Language matters. It can either increase shame or reduce it.
🌱 Take Care of Yourself Too
Supporting someone in addiction is exhausting—physically and emotionally.
You also need:
- Rest
- Support (friends, therapy, groups)
- Space to step back when needed
You cannot regulate someone else if you are completely depleted.
💬 Final Thoughts
When families understand the physical reality of addiction, everything shifts.
It becomes less about “What’s wrong with them?”
and more about “What are they going through—and how can I respond effectively?”
Support doesn’t mean fixing or rescuing.
It means showing up informed, grounded, and consistent.
Because healing happens best in environments that feel safe—
not perfect, but steady, informed, and human.
Beyond Willpower: How Community Resources Support the Physical Reality of Addiction
Addiction is often framed as a personal battle—something to be fought with determination, discipline, and inner strength. But this view leaves out a critical truth: addiction is physical, and physical problems require real, external support.
No one is expected to heal a broken bone alone. The same logic applies here. Recovery from addiction often requires structured, community-based resources that help stabilize the body while the mind catches up.
Understanding and using these resources isn’t a sign of weakness—it’s a strategy grounded in reality.
🏥 Medical Support: Stabilizing the Body First
Because addiction alters brain chemistry and bodily function, medical support is often the first step.
Community resources may include:
- Detox centers with medical supervision
- Outpatient or inpatient treatment programs
- Medication-assisted treatment (MAT)
These services help manage withdrawal safely and reduce physical cravings, giving the body a chance to stabilize.
Key idea: Recovery isn’t just about stopping—it’s about safely transitioning the body.
💊 Medication-Assisted Treatment (MAT): Supporting Brain Chemistry
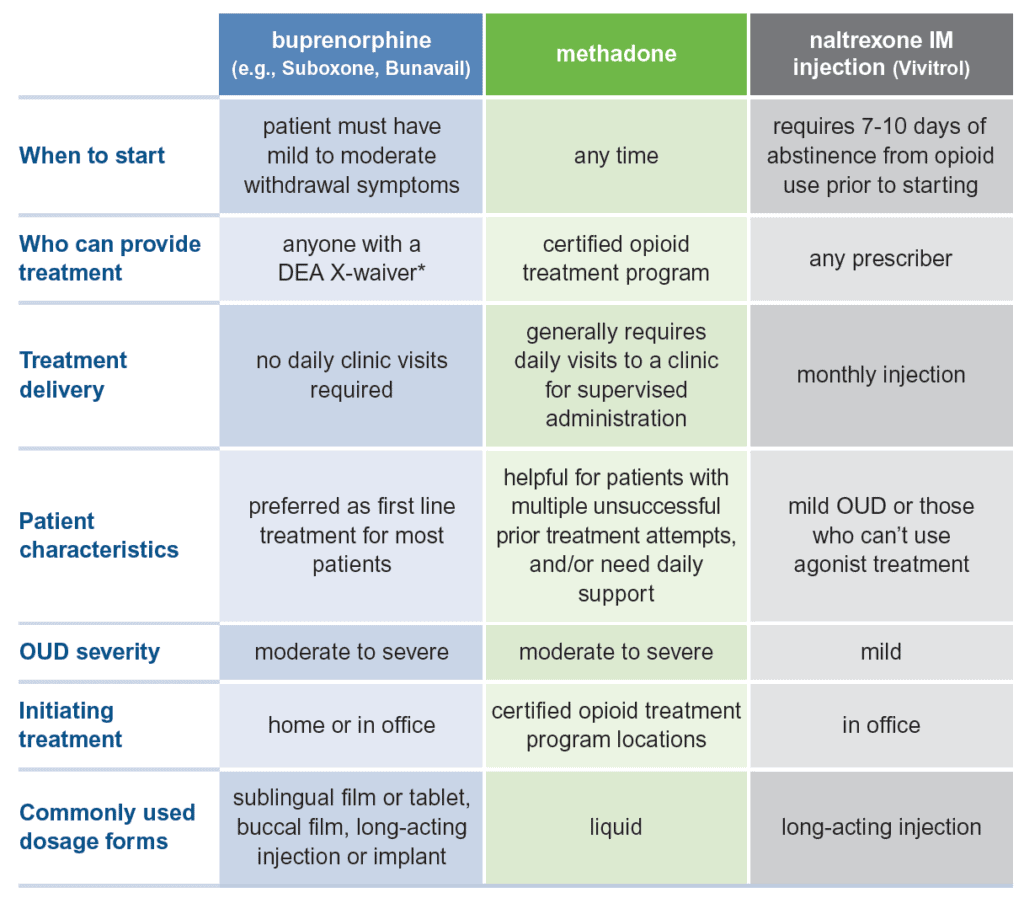
For some individuals, medications like buprenorphine, methadone, or naltrexone can:
- Reduce cravings
- Prevent withdrawal symptoms
- Normalize brain function over time
This isn’t “replacing one drug with another”—it’s treating a physiological condition.
Community strategy:
Reduce stigma around MAT and help people access providers who offer it. It can dramatically improve stability and survival.
🧠 Behavioral Health Services: Rewiring the System
While addiction is physical, the brain also needs retraining.
Community resources include:
- Individual therapy (like CBT or trauma-informed care)
- Group therapy programs
- Intensive outpatient programs (IOPs)
These services help people:
- Understand triggers
- Build coping strategies
- Reconnect thoughts, emotions, and physical responses
🤝 Peer Support: Regulation Through Connection
Isolation fuels addiction. Connection helps regulate it.
Peer support groups (like 12-step programs or non-12-step alternatives) offer:
- Shared experience
- Accountability
- Emotional regulation through connection
Being around others who understand reduces shame—and helps the nervous system feel safer.
🏠 Recovery-Friendly Environments

The body cannot heal in chaos.
Community-based supports like:
- Sober living homes
- Recovery community centers
- Job training and employment programs
- Access to food, transportation, and healthcare
…create stability. And stability is what allows the nervous system—and the brain—to recover.
🔁 Coordinated Care: When Resources Work Together
The most effective approach isn’t one resource—it’s a network:
- Medical care for the body
- Therapy for behavior and thought patterns
- Peer support for connection
- Stable environments for daily life
When these systems work together, recovery becomes more sustainable because it addresses the full physical reality of addiction.
🌱 Redefining Strength
Using community resources is not “needing help too much.”
It’s recognizing that addiction affects:
- Biology
- Environment
- Behavior
- Connection
And no single person can manage all of that alone.
💬 Final Thoughts
When we understand addiction as physical, the solution becomes clearer:
People need support systems, not just self-control.
Community resources exist to:
- Stabilize the body
- Reduce harm
- Create structure
- Support long-term healing
Recovery doesn’t happen in isolation.
It happens in systems of care, connection, and consistency.
Because healing the body requires more than willpower—
It requires support that meets it where it actually is.
Frequently Asked Questions
Here are some common questions:
1. Is addiction really a physical condition or just mental?
Addiction is both physical and psychological, but the physical component is often underestimated. Repeated substance use changes brain chemistry, especially in the dopamine system, making the body dependent on the substance to feel normal. Over time, this creates real physiological changes—not just habits or thoughts.
2. Why do people feel physically sick when they stop using?
This is called withdrawal. The body adapts to the presence of a substance, so when it’s removed, the system becomes unstable. Symptoms like nausea, sweating, shaking, anxiety, and pain are the body’s way of trying to rebalance itself. In some cases (like alcohol withdrawal), it can be dangerous without medical support.
3. Why can’t someone just “use willpower” to stop?
Because addiction affects the brain’s decision-making and reward systems. The prefrontal cortex (responsible for judgment and impulse control) weakens, while craving and reward circuits strengthen. This makes stopping feel like fighting against your own biology—not just making a choice.
4. Does addiction affect the whole body or just the brain?
Addiction impacts the entire body, including:
- Heart (increased strain)
- Liver (especially with alcohol use)
- Sleep cycles (disruption and insomnia)
- Hormones (chronic stress response)
- Immune system (weakened over time)
It’s a full-body condition, not just a brain issue.
5. What do cravings actually feel like physically?
Cravings are often bodily sensations, not just thoughts. People may feel:
- Tightness in the chest
- Restlessness or agitation
- A “pull” or urgency in the body
- Increased heart rate
Understanding cravings as physical sensations can help people manage them more effectively.
6. How long does it take for the body to recover?
Recovery varies, but generally:
- Days to weeks: acute withdrawal improves
- Weeks to months: sleep and mood begin stabilizing
- Months to years: brain chemistry and stress systems continue to heal
Healing is gradual because the body needs time to rebalance.
7. Is relapse a failure or part of the physical process?
Relapse is often part of the chronic nature of addiction. Because the brain has been rewired, triggers and stress can reactivate cravings. It doesn’t mean someone failed—it often means the body and brain need more support, structure, or time.
8. Can the brain and body fully heal from addiction?
Yes—significant healing is possible. The brain can rewire itself (neuroplasticity), and the body can recover many functions over time. However, some vulnerabilities may remain, which is why ongoing support and awareness are important.
9. Why does stress make addiction worse?
Stress activates the body’s fight-or-flight system, which is already dysregulated in addiction. Substances often become a way to calm or escape that stress. When stress increases, cravings often intensify because the body seeks relief.
10. What helps the body heal during recovery?
Physical recovery is supported by:
- Consistent sleep
- Proper nutrition and hydration
- Medical or therapeutic support
- Movement and nervous system regulation (like breathing or grounding)
- Social connection
These help restore balance to the systems affected by addiction.
11. Why does someone feel “empty” or numb in early sobriety?
Because the brain’s dopamine system has been overstimulated and then depleted. Without substances, the brain may temporarily struggle to produce normal levels of pleasure. This is a biological adjustment period, not a permanent state.
12. How can understanding the physical side of addiction help?
It reduces shame and misunderstanding. Instead of asking, “What’s wrong with me?” or “Why won’t they stop?” the question becomes:
“What is the body going through, and what does it need to heal?”
This shift leads to more effective, compassionate recovery strategies.
Conclusion
Recognizing the physical reality of addiction changes the way we think about recovery. It shifts the narrative from blame to understanding, from willpower to support, and from quick fixes to long-term healing. When we see addiction as something that affects the entire body, it becomes clear why recovery requires time, structure, and compassion. Healing is not simply about making better decisions—it is about restoring balance to systems that have been pushed out of equilibrium. By approaching addiction with this deeper awareness, we create space for more effective care, stronger support systems, and a more humane response to those navigating recovery.
Video: