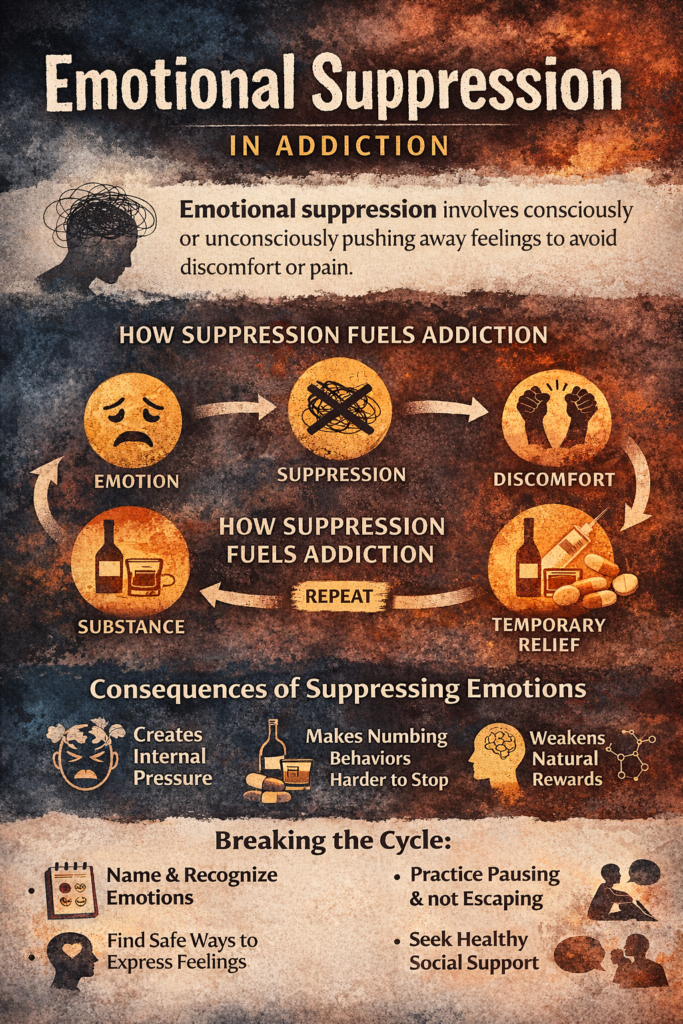
Emotional suppression plays a central but often overlooked role in addiction. Rather than openly experiencing and processing feelings, individuals may push emotions out of awareness—consciously or unconsciously—as a way to cope with stress, trauma, or overwhelming internal states. While this strategy can create short-term relief, it often leads to a buildup of unresolved emotional tension. Over time, substances or addictive behaviors can become substitutes for emotional regulation, offering temporary escape from what has been left unaddressed. Understanding emotional suppression is essential to understanding addiction itself, because the behavior is often less about seeking pleasure and more about avoiding what feels too difficult to face.
Emotional Suppression in Addiction: The Feelings We Avoid and the Habits That Follow
Addiction rarely begins with the substance itself—it often begins with a feeling that someone didn’t know how, or didn’t feel safe enough, to experience.
Emotional suppression is the process of consciously or unconsciously pushing away feelings. Instead of being allowed to be felt, processed, and understood, emotions are minimized, ignored, or buried. On the surface, this can look like control. In reality, it often creates pressure beneath that control—pressure that eventually seeks a release.
For many people struggling with addiction, that release becomes a substance or behavior.
Why We Suppress Emotions
Emotional suppression doesn’t come out of nowhere. It’s usually learned.
Some people grow up in environments where emotions are dismissed—“stop crying,” “you’re overreacting,” “just deal with it.” Others experience trauma, where feeling too much becomes overwhelming or even unsafe. Over time, the brain adapts by reducing emotional awareness as a form of protection.
In psychological terms, this is a form of avoidance-based coping. It works in the short term by reducing discomfort, but it comes with a cost: the emotion doesn’t disappear—it just goes underground.
What Happens in the Brain
When emotions are suppressed, the brain doesn’t simply “turn them off.” Instead, several things happen:
- The emotional centers (like the amygdala) remain active
- Stress hormones such as cortisol can stay elevated
- The prefrontal cortex works overtime to maintain control
- Emotional awareness becomes less clear over time
This creates a state of internal tension—feeling something without fully knowing or processing it. Many describe it as numbness, irritability, or a vague sense that something is “off.”
How Suppression Fuels Addiction
Substances and addictive behaviors often step in where emotional processing is missing.
- Alcohol may dampen anxiety or sadness
- Opioids can create a sense of warmth or relief
- Stimulants may override feelings of emptiness or fatigue
- Compulsive behaviors (like gambling or scrolling) can distract from internal discomfort
In this way, addiction becomes less about pleasure and more about regulation. It’s not just chasing a high—it’s escaping what hasn’t been felt.
Over time, the brain begins to associate relief with the substance, reinforcing the cycle:
emotion → suppression → discomfort → substance → temporary relief → repeat
The Paradox of Numbness
One of the most difficult parts of emotional suppression is that it doesn’t just block painful emotions—it blunts positive ones too.
People may say:
- “I don’t feel sad, but I don’t feel happy either.”
- “I just feel flat.”
- “Nothing really affects me anymore.”
This emotional narrowing can deepen reliance on substances, because the natural reward system becomes less responsive. What once brought joy no longer does, making artificial relief feel even more necessary.
Recovery: Learning to Feel Again
Recovery isn’t just about stopping a substance—it’s about rebuilding the ability to experience emotions safely.
This doesn’t mean being overwhelmed by feelings. It means gradually increasing emotional tolerance and awareness.
Some key parts of this process include:
- Recognizing emotions (naming what you feel)
- Allowing discomfort without immediate escape
- Understanding the meaning behind emotions
- Developing healthier regulation strategies
Therapies like cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), and trauma-informed approaches often focus heavily on these skills.
A Different Perspective
What if emotional suppression isn’t a flaw—but a strategy that once made sense?
For many, it was a way to survive. The problem isn’t that the brain learned to suppress emotions—it’s that the strategy continued long after it was needed.
Addiction, in this light, isn’t just self-destruction. It’s often self-protection—misguided, costly, but rooted in an attempt to cope.
Closing Thought
You can’t selectively numb emotions. When you push down pain, you also push down clarity, connection, and relief.
Recovery begins not with forcing yourself to feel everything at once, but with creating enough safety to feel something—even if it’s small, even if it’s unclear.
Because the feelings we avoid don’t disappear.
They wait—until we’re ready to understand them.
Managing What You Feel: Self-Strategies for Emotional Suppression in Addiction Recovery
Emotional suppression doesn’t just disappear when someone decides to stop using a substance. In many cases, it becomes more noticeable.
Without the buffer of alcohol, drugs, or compulsive behaviors, emotions that were once muted can begin to surface—sometimes slowly, sometimes all at once. For people in recovery, this can feel confusing or even overwhelming. You may not know what you’re feeling, only that something doesn’t feel right.
This is where self-management becomes essential—not to control emotions, but to understand and work with them.
Why Self-Management Matters
In addiction, substances often act as a shortcut for emotional regulation. When that shortcut is removed, there’s a gap.
Self-management strategies help fill that gap by:
- Increasing awareness of internal states
- Reducing the urge to escape discomfort
- Building tolerance for difficult emotions
- Creating safer ways to process what’s been suppressed
This isn’t about perfection—it’s about developing a different relationship with your internal experience.
1. Name What You Can (Even If It’s Vague)
One of the first challenges with emotional suppression is identifying emotions at all.
Instead of forcing precision, start simple:
- “I feel off.”
- “Something feels heavy.”
- “I’m irritated, but I don’t know why.”
Labeling emotions—even loosely—activates areas of the brain that help regulate them. Over time, this builds emotional clarity.
2. Use the Pause Instead of the Escape
When discomfort shows up, the instinct may be to distract, numb, or avoid.
A self-management alternative is the intentional pause:
- Take a breath
- Notice what’s happening in your body
- Delay reacting for even 30–60 seconds
This creates space between feeling and action. That space is where change begins.
3. Track Patterns, Not Just Moments
Suppressed emotions often show up indirectly—through irritability, fatigue, cravings, or restlessness.
Keeping a simple daily log can help:
- What did I feel today?
- When did cravings increase?
- What was happening before that?
Over time, patterns emerge. You begin to see that emotions aren’t random—they’re connected to experiences, thoughts, and unmet needs.
4. Build a Safe Outlet for Expression
Suppression thrives in silence. Expression doesn’t have to be dramatic—it just has to exist.
Some options:
- Writing thoughts without filtering
- Talking to someone you trust
- Engaging in creative outlets (music, art, movement)
The goal isn’t to “fix” the feeling, but to let it move rather than stay stuck.
5. Differentiate Between Feeling and Acting
A key part of recovery is learning that:
Feeling something does not mean you have to act on it.
You can feel:
- Angry without reacting impulsively
- Sad without withdrawing completely
- Anxious without escaping
This distinction reduces fear around emotions. They become experiences—not threats.
6. Regulate the Body to Support the Mind
Suppressed emotions often live in the body as tension, fatigue, or restlessness.
Simple regulation strategies include:
- Slow, steady breathing
- Walking or light movement
- Grounding techniques (noticing your surroundings)
- Prioritizing sleep and nutrition
When the body is calmer, emotions become more manageable.
7. Expect Discomfort—Not Danger
One of the biggest barriers to facing suppressed emotions is the belief that they will be overwhelming or unmanageable.
In reality, most emotions rise, peak, and fall—like waves.
Reminding yourself:
- “This is uncomfortable, but not harmful.”
- “I can stay with this for a moment longer.”
builds emotional tolerance over time.
A Shift in Perspective
Emotional suppression isn’t something to “get rid of” overnight. It’s a pattern that once served a purpose.
Self-management is about replacing that pattern—not with avoidance, but with awareness and choice.
You’re not trying to feel everything all at once.
You’re learning that you can feel—without needing to escape.
Closing Thought
Recovery isn’t just about removing a substance. It’s about developing the ability to stay present with yourself—especially when it’s uncomfortable.
The more you understand your suppressed emotions, the less power they have to drive behavior in the background.
Because when emotions are acknowledged,
they no longer have to be numbed.
Supporting What Isn’t Said: Family Strategies for Emotional Suppression in Addiction
One of the most confusing parts of supporting someone with addiction is not what they say, but what they don’t.
Many individuals struggling with addiction also struggle with emotional suppression. They may avoid talking about feelings, shut down during difficult conversations, or insist they’re “fine” even when it’s clear something is wrong. For families, this silence can feel like distance, resistance, or even rejection.
But often, it’s none of those things.
It’s protection.
Understanding Emotional Suppression in a Family Context
Emotional suppression is rarely as intentional as it appears. It’s not about refusing to communicate—it’s about not knowing how, or not feeling safe enough to try.
In some cases, the person may not even fully recognize what they’re feeling. Emotions show up indirectly—through irritability, withdrawal, defensiveness, or substance use.
For families, understanding this shift is critical:
The issue isn’t just communication—it’s emotional accessibility.
Why Family Support Matters
Recovery doesn’t happen in isolation. The emotional environment around a person can either reinforce suppression or gently challenge it.
Supportive family dynamics can:
- Reduce shame around emotions
- Increase a sense of safety
- Encourage gradual openness
- Lower the need for avoidance of substances
But this kind of support requires a different approach than simply asking someone to “open up.”
1. Create Safety Before Expecting Honesty
People are more likely to express emotions when they feel safe—not judged, corrected, or overwhelmed.
This means:
- Listening without immediately giving advice
- Avoiding criticism or interrogation
- Allowing silence without pressure
Sometimes, safety sounds like:
- “You don’t have to explain everything—I’m here when you’re ready.”
- “I’m not here to judge you. I just want to understand.”
2. Don’t Force Emotional Expression
Pushing someone to talk before they’re ready can increase shutdown.
Instead of:
- “Why won’t you just tell me what’s wrong?”
Try:
- “I can see something’s going on. If you ever want to talk, I’m here.”
This keeps the door open without making it feel like a demand.
3. Learn to Read Indirect Signals
When emotions are suppressed, they often show up as behavior:
- Irritability may signal frustration or fear
- Withdrawal may reflect overwhelm or shame
- Anger can mask sadness or vulnerability
Responding to the underlying emotion—not just the behavior—can shift the interaction:
- “You seem really stressed lately. I’m here if you need support.”
4. Model Healthy Emotional Expression
Family members don’t need to be perfect—but they can be examples.
Expressing your own emotions in a calm, regulated way shows that feelings are manageable:
- “I felt worried when I didn’t hear from you.”
- “I’m frustrated, but I want to talk this through.”
This normalizes emotional expression without forcing it.
5. Separate the Person from the Behavior
Addiction and emotional suppression can lead to actions that are hurtful or confusing.
Support doesn’t mean ignoring boundaries—but it does mean maintaining perspective:
- The behavior may be problematic
- The person is still deserving of understanding
Balancing accountability with empathy helps reduce shame, which is often a driver of suppression.
6. Encourage, Don’t Control
Families often want to fix the situation—to push for treatment, change, or openness.
But control can backfire, increasing resistance or deeper suppression.
Encouragement sounds like:
- “I think talking to someone could really help—you deserve that support.”
Control sounds like:
- “You need to do this or else.”
The difference matters.
7. Take Care of Yourself Too
Supporting someone through addiction and emotional suppression can be emotionally draining.
Family members need their own support systems:
- Therapy or counseling
- Support groups
- Personal boundaries and time for rest
You cannot create a healthy emotional environment if you are consistently overwhelmed.
A Different Way to See It
What looks like silence may actually be someone doing their best to hold themselves together.
Emotional suppression isn’t about shutting others out—it’s often about trying not to fall apart.
When families shift from:
- “Why won’t they talk?”
to - “What might make it safer for them to feel?”
The entire dynamic can change.
Closing Thought
You can’t force someone to express what they don’t yet understand.
But you can create an environment where understanding becomes possible.
Because sometimes, the most powerful support isn’t in getting someone to speak—
It’s in showing them they’re safe enough to try.
From Isolation to Connection: Community Support for Suppressed Emotions in Recovery
Emotional suppression thrives in isolation.
When feelings are pushed down long enough, people often begin to disconnect—not just from their emotions, but from others. Addiction can deepen that disconnection, creating a cycle where substances replace both emotional processing and meaningful connection.
This is where community becomes more than helpful—it becomes essential.
Community resources offer something that individuals and families alone often cannot: shared understanding, structured support, and a sense that you’re not navigating this alone.
Why Community Matters in Emotional Suppression
Suppressed emotions don’t just need awareness—they need safe environments to be expressed and understood.
Community-based support can:
- Normalize emotional experiences
- Reduce shame and stigma
- Provide language for feelings that are hard to identify
- Offer real-life examples of others working through similar struggles
In many cases, hearing someone else articulate a feeling you couldn’t name is the first step toward recognizing your own.
1. Peer Support Groups: Shared Experience, Shared Language
Support groups—such as 12-step programs or non-12-step alternatives—create a space where emotional honesty is encouraged, but not forced.
Benefits include:
- Listening without pressure to speak
- Learning emotional vocabulary through others’ stories
- Realizing that suppressed feelings are common, not personal failures
For many, the simple act of saying “me too” begins to break down emotional barriers.
2. Group Therapy: Guided Emotional Exploration
Unlike peer groups, group therapy is facilitated by a trained professional who helps guide emotional awareness and interaction.
This setting can:
- Help identify patterns of suppression
- Provide structured ways to express emotions
- Offer feedback in a controlled, supportive environment
It bridges the gap between individual therapy and peer support, combining both professional insight and shared experience.
3. Community Mental Health Services
Local clinics, outreach programs, and nonprofit organizations often provide:
- Counseling services
- Psychoeducation workshops
- Crisis support
These resources are especially important for individuals who may not otherwise have access to care.
They also help connect emotional suppression to broader mental health patterns, making it easier to understand what’s happening internally.
4. Recovery-Focused Programs and Centers
Recovery centers often integrate emotional awareness into their programs, offering:
- Relapse prevention strategies
- Emotional regulation skills training
- Structured daily routines
These environments reinforce the idea that recovery isn’t just about abstaining—it’s about learning how to experience and manage emotions safely.
5. Educational Workshops and Skill-Building Spaces
Workshops focused on topics like:
- Emotional regulation
- Stress management
- Mindfulness
can help individuals develop tools to recognize and process suppressed emotions.
These are often more accessible and less intimidating than therapy, making them a useful entry point for many.
6. Online Communities and Digital Support
Not everyone has immediate access to in-person resources. Online communities can provide:
- Anonymity, which reduces fear of judgment
- Flexible access to support
- Exposure to diverse experiences and coping strategies
While not a replacement for professional care, they can be a valuable supplement—especially in the early stages of awareness.
7. Reducing Barriers to Access
Understanding emotional suppression in addiction isn’t just about having resources—it’s about being able to use them.
Communities play a role in:
- Reducing stigma around addiction and mental health
- Increasing affordability and availability of services
- Promoting awareness of existing support systems
The more accessible these resources are, the more likely individuals are to engage with them.
A Shift from Isolation to Connection
Emotional suppression often convinces people that:
- Their feelings are too much
- Their experiences are unique
- Their struggles should be handled alone
The community challenges these beliefs.
It shows that emotions—no matter how complex—are part of a shared human experience.
Closing Thought
You don’t have to fully understand your emotions to begin connecting with others.
Sometimes, understanding comes because of connection.
Community resources don’t just provide support—
They create spaces where suppressed emotions can finally be recognized, named, and slowly brought into the open.
Because healing doesn’t happen in isolation.
It happens where people feel seen.
Frequently Asked Questions
Here are some common questions:
1. What is emotional suppression in addiction?
Emotional suppression in addiction refers to the habit of avoiding, ignoring, or pushing away feelings—often unconsciously—and using substances or behaviors to cope instead. Rather than processing emotions, the individual numbs or distracts from them, which can reinforce addictive patterns.
2. Why do people with addiction suppress their emotions?
Emotional suppression is usually a learned coping strategy. It can develop from:
- Trauma or overwhelming experiences
- Environments where emotions weren’t safe or accepted
- Fear of vulnerability or loss of control
In many cases, suppression began as a way to protect oneself, but later contributed to unhealthy coping mechanisms.
3. Is emotional suppression the same as emotional control?
No. Emotional control (or regulation) involves recognizing and managing emotions in a healthy way.
Emotional suppression, on the other hand, involves avoiding or denying emotions altogether.
Suppression reduces awareness, while regulation builds understanding.
4. How does emotional suppression contribute to addiction?
When emotions are suppressed, they don’t disappear—they build up internally. This can create:
- Anxiety or tension
- Emotional numbness
- Irritability or restlessness
Substances then become a means of relieving or escaping that discomfort, reinforcing a cycle of avoidance and use.
5. Can someone be unaware that they are suppressing emotions?
Yes. Many people don’t realize they are suppressing emotions because it has become automatic. Instead of feeling emotions clearly, they may experience:
- Feeling “off” without knowing why
- Difficulty identifying feelings
- Physical tension or fatigue
This is sometimes referred to as reduced emotional awareness.
6. What are the signs of emotional suppression in addiction?
Common signs include:
- Avoiding emotional conversations
- Saying “I’m fine” when clearly distressed
- Difficulty identifying or naming feelings
- Emotional numbness or detachment
- Increased reliance on substances during stress
7. Does emotional suppression affect recovery?
Yes, significantly. If emotions remain unprocessed, they can:
- Trigger cravings
- Increase relapse risk
- Make recovery feel overwhelming or unstable
Recovery often involves learning how to safely experience and regulate emotions.
8. What happens when suppressed emotions start to surface?
This can feel uncomfortable or even intense at first. People may experience:
- Sudden mood shifts
- Unexpected sadness, anger, or anxiety
- Emotional confusion
However, this is often a sign of progress—emotions are becoming accessible rather than avoided.
9. How can someone begin to address emotional suppression?
Some starting strategies include:
- Noticing and labeling feelings (even vaguely)
- Practicing pauses instead of immediate escape
- Journaling or talking with someone safe
- Learning emotional regulation skills (CBT, DBT)
The goal is gradual awareness—not overwhelming exposure.
10. Can emotional suppression ever be helpful?
In the short term, suppression can help someone function during overwhelming situations. However, long-term reliance on suppression is generally harmful, especially when it replaces healthy emotional processing.
11. How can families support someone dealing with emotional suppression and addiction?
Families can help by:
- Creating a non-judgmental environment
- Avoiding pressure to “open up.”
- Listening without trying to fix immediately
- Modeling healthy emotional expression
Support works best when it increases safety, not pressure.
12. Is professional help necessary to work through emotional suppression?
While some people can build awareness on their own, professional support is often beneficial—especially when suppression is tied to trauma or long-term addiction. Therapies like CBT, DBT, and trauma-informed care provide structured guidance.
13. Does emotional suppression affect physical health, too?
Yes. Chronic suppression is associated with:
- Increased stress hormones
- Tension in the body
- Sleep disturbances
- Higher overall stress load
Emotions that aren’t processed psychologically often show up physically.
14. What is the long-term goal in recovery regarding emotions?
The goal is not to feel everything intensely all the time.
It’s to:
- Recognize emotions
- Tolerate discomfort
- Respond rather than react
- Use healthier ways to cope
In short: from avoidance → to awareness → to regulation
Conclusion
Addressing emotional suppression is a critical part of meaningful recovery from addiction. It involves more than simply stopping substance use—it requires developing the ability to recognize, tolerate, and process emotions in healthier ways. This process takes time, support, and patience, as suppressed feelings may surface gradually and sometimes unpredictably. However, as emotional awareness increases, the need to rely on substances for relief often decreases. By shifting from avoidance to understanding, individuals can begin to replace cycles of suppression and escape with patterns of awareness and resilience, creating a more stable foundation for long-term recovery.
Video: