Methamphetamine use disorder is a chronic and multifaceted condition that profoundly impacts brain function, especially in regions involved in impulse control, decision-making, and reward processing. Unlike opioid use disorder, there are currently no widely approved medications specifically tailored to treat meth addiction, highlighting the need for new and innovative interventions. One promising approach is transcranial magnetic stimulation (TMS), a non-invasive technique that uses targeted magnetic pulses to stimulate the prefrontal cortex, helping to regulate cravings and strengthen cognitive control. By directly addressing the underlying neurobiological changes associated with addiction, TMS represents a shift toward brain-focused treatment strategies that may improve recovery outcomes when combined with behavioral therapies and supportive care.
Rewiring Recovery: How TMS Is Changing Meth Addiction Treatment
Methamphetamine use disorder remains one of the most challenging substance use disorders to treat. Unlike opioid use disorder—which has several FDA-approved medications—there are currently no widely approved pharmacological treatments specifically for meth addiction. This gap has prompted researchers and clinicians to explore alternative approaches, including transcranial magnetic stimulation (TMS), a non-invasive brain stimulation technique gaining attention in addiction medicine.
What Is TMS?
TMS uses magnetic pulses to stimulate specific areas of the brain—most commonly the prefrontal cortex, which plays a key role in decision-making, impulse control, and craving regulation. During treatment, a coil is placed on the scalp to deliver repeated pulses (repetitive TMS, or rTMS) that modulate neural activity.
In individuals with methamphetamine use disorder, this region is often dysregulated, contributing to intense cravings and impaired self-control. TMS aims to “rebalance” these circuits.
Why TMS for Meth Addiction?
Meth use profoundly alters the brain’s reward system, particularly dopamine pathways. Over time, natural rewards become less meaningful, while drug-related cues become overpowering.
TMS may help by:
- Reducing cravings through modulation of reward-related circuits
- Improving executive function, including impulse control
- Enhancing treatment engagement by stabilizing mood and cognition
- Potentially reducing relapse risk, especially when combined with behavioral therapy
Early studies suggest that targeting the dorsolateral prefrontal cortex (DLPFC) can significantly decrease craving intensity in some patients.
What Does the Treatment Process Look Like?

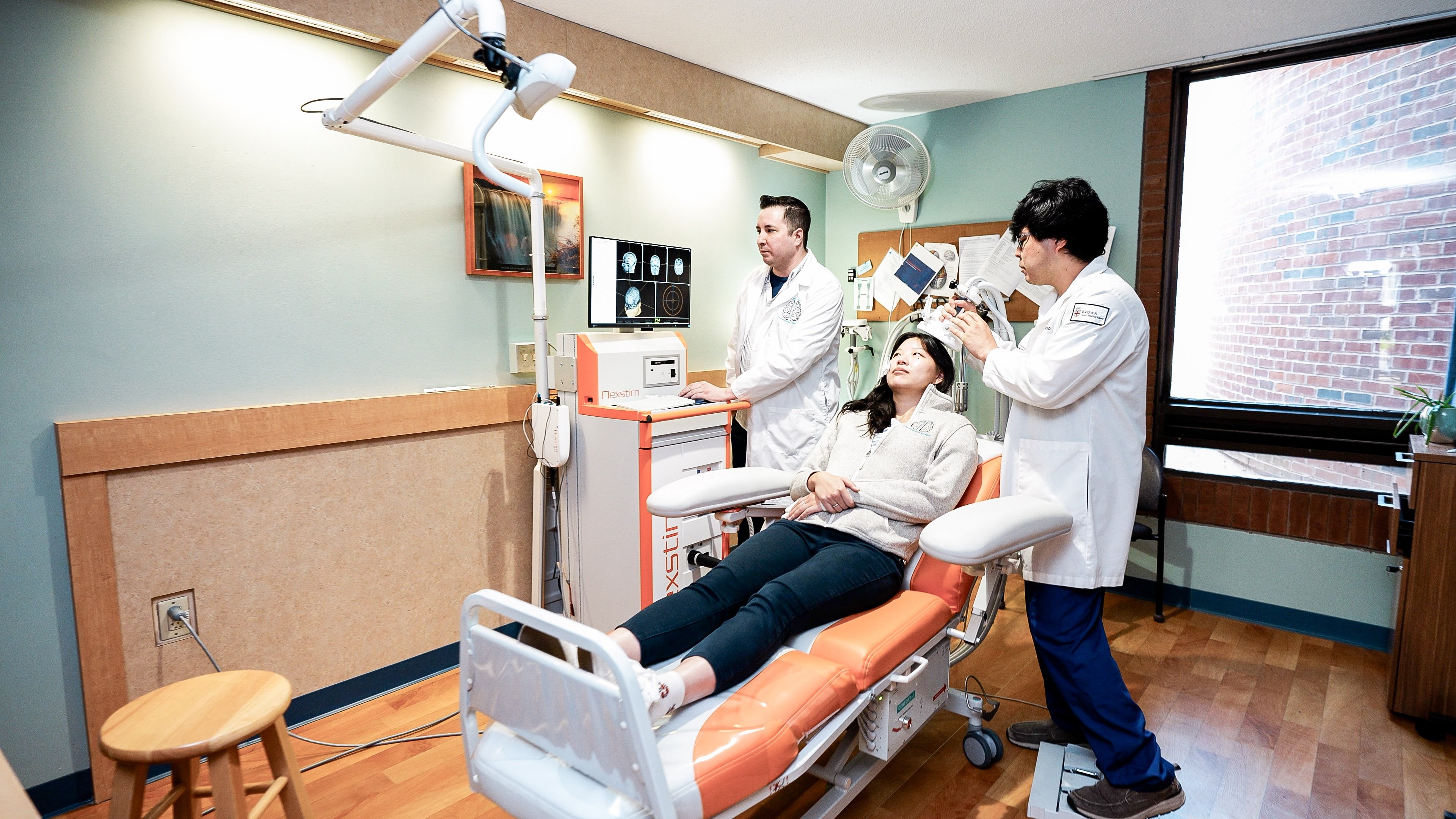
A typical TMS treatment course includes:
- Outpatient sessions (no anesthesia required)
- 20–40 minute treatments, usually 5 days per week
- A course lasting 4–6 weeks, sometimes longer
Patients remain awake and alert during the procedure and can resume normal activities immediately afterward.
Benefits and Limitations
Potential Benefits
- Non-invasive and generally well tolerated
- No systemic side effects from medications
- May address both addiction and co-occurring depression
Limitations
- Still considered emerging/experimental for methamphetamine use disorder
- Not universally accessible or covered by insurance for this indication
- Results vary—some patients respond more than others
The Future of TMS in Addiction Treatment
TMS represents a shift toward neuroscience-based treatments for addiction. Rather than only focusing on behavior or medication, it directly targets the brain circuits underlying craving and relapse.
Ongoing research is exploring:
- Optimal stimulation protocols
- Combination with therapies like cognitive behavioral therapy (CBT)
- Long-term outcomes and relapse prevention
While it is not a standalone cure, TMS may become a valuable part of a comprehensive treatment plan—especially for individuals who have not responded to traditional approaches.
Final Thoughts
Meth addiction is deeply rooted in brain changes that make recovery difficult—but not impossible. TMS offers a promising new pathway by helping the brain “reset,” giving individuals a better chance of regaining control.
As research continues to evolve, treatments like TMS may redefine how we approach addiction—moving from purely behavioral models to integrated brain-based care.
Taking Control of Recovery: Self-Management Strategies for Understanding TMS in Meth Addiction Treatment
Recovering from methamphetamine use disorder is not just about stopping drug use—it’s about rebuilding how the brain responds to stress, cravings, and decision-making. As newer treatments like transcranial magnetic stimulation (TMS) emerge, individuals are not only participants in care but active partners in understanding and managing their recovery.
Self-management strategies can help people better understand TMS, maximize its benefits, and stay engaged throughout the treatment process.
What Is TMS and Why Does It Matter?
TMS is a non-invasive treatment that uses magnetic pulses to stimulate brain regions involved in craving, impulse control, and decision-making—especially the prefrontal cortex.
For individuals with meth addiction, these brain areas can become dysregulated. TMS aims to help “reset” these circuits, making it easier to manage urges and think more clearly.
But understanding how and why it works is key to staying motivated and committed.
Why Self-Management Matters in TMS Treatment
TMS is not a passive cure. Its effectiveness often improves when combined with:
- Behavioral therapy
- Lifestyle changes
- Active engagement in recovery
Self-management empowers individuals to:
- Track their progress
- Recognize triggers and cravings
- Stay consistent with treatment
- Advocate for their needs in clinical settings
Key Self-Management Strategies
1. 📝 Learn the Basics of Your Treatment
Understanding TMS reduces fear and uncertainty. Ask questions like:
- What part of my brain is being targeted?
- How many sessions will I need?
- What changes should I expect—and when?
Keeping a notebook or digital log of what you learn can improve retention and confidence.
2. 📊 Track Cravings and Mood Changes
TMS often works gradually. Keeping track of daily experiences can help you notice subtle improvements.
Try logging:
- Craving intensity (1–10 scale)
- Mood and stress levels
- Sleep quality
- Triggers or high-risk situations
This information can also help your provider adjust treatment if needed.
3. 🧘 Build Complementary Coping Skills
TMS supports brain function—but coping skills reinforce it. Helpful strategies include:
- Mindfulness and breathing exercises
- Journaling thoughts and cravings
- Attending therapy or support groups
- Regular physical activity
These tools strengthen the same brain systems that TMS targets.
4. 📅 Stay Consistent with Treatment
TMS requires repeated sessions to be effective. Missing appointments can disrupt progress.
Tips:
- Set reminders or alarms
- Pair sessions with a routine (e.g., before work)
- Plan transportation ahead of time
Consistency is one of the strongest predictors of success.
5. 🗣️ Communicate with Your Care Team
Be open about:
- Side effects (even mild ones)
- Changes in cravings or mood
- Concerns or confusion
TMS protocols can often be adjusted, and your feedback is essential.
Challenges to Expect
Even with TMS and strong self-management:
- Cravings may not disappear immediately
- Progress can feel slow or uneven
- Motivation may fluctuate
This is normal. Recovery is a process—not a straight line.
The Bigger Picture: Empowered Recovery
TMS represents a shift toward brain-based treatment, but recovery still depends on the individual’s engagement. Self-management bridges that gap—helping people move from feeling controlled by addiction to actively shaping their recovery.
By understanding the treatment, tracking progress, and building coping skills, individuals can get the most out of TMS and create a more sustainable path forward.
Final Thoughts
TMS offers hope—but knowledge and self-management turn that hope into action. When individuals take an active role in their treatment, they don’t just receive care—they become partners in their own recovery.
Supporting Recovery Together: Family Strategies for Understanding TMS in Meth Addiction Treatment
Methamphetamine use disorder affects more than the individual—it impacts families, relationships, and entire support systems. As new treatments like transcranial magnetic stimulation (TMS) emerge, families often find themselves asking, “How can we help?” and What does this treatment actually do?
Understanding TMS and adopting supportive strategies can make a meaningful difference in a loved one’s recovery journey. Family involvement doesn’t just provide emotional support—it can improve treatment engagement, consistency, and long-term outcomes.
What Is TMS and Why Should Families Understand It?
TMS is a non-invasive treatment that uses magnetic pulses to stimulate brain regions involved in cravings, impulse control, and decision-making. For individuals with meth addiction, these brain circuits can become dysregulated.
When families understand that addiction involves real brain changes, it can shift perspectives from blame to support. TMS represents a biological approach to treatment—helping the brain regain balance.
Why Family Support Matters in TMS Treatment
TMS is most effective when combined with consistency and a stable environment. Families can play a key role by:
- Encouraging attendance at treatment sessions
- Reducing stressors at home
- Reinforcing healthy behaviors
- Providing accountability without judgment
Supportive involvement can increase motivation and reduce the risk of relapse.
Key Family Support Strategies
1. 📘 Educate Yourself About TMS and Addiction
Take time to learn:
- How TMS works
- What the treatment schedule looks like
- What changes to expect (and what not to expect)
This helps reduce misunderstandings and allows you to provide informed support.
2. 🗣️ Communicate Without Judgment
Recovery is often accompanied by setbacks, mood changes, or frustration. Supportive communication includes:
- Listening more than lecturing
- Avoiding blame or criticism
- Using encouraging, non-stigmatizing language
For example, instead of “Why can’t you just stop?” try “How can I support you right now?”
3. 🚗 Support Treatment Consistency
TMS requires frequent sessions over several weeks. Families can help by:
- Providing transportation
- Helping manage schedules
- Offering reminders and encouragement
Consistency is critical for TMS to be effective.
4. 🏡 Create a Stable, Low-Stress Environment
Stress is a major trigger for cravings. Families can support recovery by:
- Reducing conflict when possible
- Establishing routines
- Encouraging healthy habits (sleep, meals, structure)
A calm environment reinforces the brain changes that TMS is trying to support.
5. 🤝 Encourage Holistic Recovery
TMS works best alongside other supports:
- Therapy or counseling
- Support groups
- Healthy lifestyle changes
Families can gently encourage participation without forcing it.
6. ⚖️ Set Healthy Boundaries
Support does not mean enabling. It’s important to:
- Set clear, consistent boundaries
- Avoid covering up harmful behaviors
- Protect your own well-being
Healthy boundaries create accountability and sustainability.
Challenges Families May Face
Supporting someone through addiction treatment can be emotionally complex:
- Progress may be slow or inconsistent
- There may be relapses or setbacks
- Family members may feel burnout or frustration
Seeking support for yourself—through counseling or family groups—can help you stay strong and effective.
The Bigger Picture: Recovery as a Shared Effort
TMS offers a promising, brain-based approach to meth addiction—but it doesn’t replace the need for human connection. Family support provides the emotional foundation that allows treatments like TMS to work more effectively.
When families are informed, compassionate, and consistent, they become a powerful part of the recovery process.
Final Thoughts
You don’t need to be an expert to make a difference. Simply showing up, learning, and offering steady support can help your loved one stay engaged in treatment and move toward recovery.
TMS may help “reset” the brain—but family support helps rebuild a life.
Building Recovery Networks: Community Resource Strategies for Understanding TMS in Meth Addiction Treatment
Methamphetamine use disorder is not just an individual challenge—it’s a community issue that requires coordinated support systems. As innovative treatments like transcranial magnetic stimulation (TMS) become more visible, communities play a critical role in helping individuals access, understand, and benefit from these services.
Community resources—ranging from clinics and support groups to outreach programs—can bridge the gap between cutting-edge treatment and real-world recovery.
What Is TMS and Why Community Awareness Matters
TMS is a non-invasive brain stimulation therapy that targets areas involved in craving, impulse control, and decision-making. While it is FDA-approved for conditions like depression, its use in methamphetamine addiction is still emerging.
Because of this, many individuals—and even providers—may not be fully aware of:
- Where TMS is available
- Who qualifies for treatment
- How it fits into addiction recovery plans
Community-level education helps close this gap.
Why Community Resources Matter
Access to TMS is not just about availability—it’s about connection. Community resources can:
- Increase awareness of treatment options
- Reduce stigma around addiction and brain-based therapies
- Help individuals navigate healthcare systems
- Provide ongoing support beyond clinical treatment
Strong community networks improve both access and outcomes.
Key Community Resource Strategies
1. 🏥 Partner with Local Treatment Providers
Community organizations can collaborate with:
- Mental health clinics offering TMS
- Addiction treatment centers
- Primary care providers
These partnerships help ensure individuals are referred appropriately and receive coordinated care.
2. 📢 Increase Public Education and Awareness
Educational efforts can include:
- Community workshops or seminars
- Informational brochures at clinics or community centers
- Social media campaigns
Clear, accessible information helps people understand that TMS is a medical, evidence-based approach, not an experimental last resort.
3. 🚍 Address Transportation and Access Barriers
TMS requires frequent outpatient visits, which can be a barrier. Communities can help by:
- Offering transportation services
- Providing gas vouchers or ride assistance
- Coordinating volunteer driver programs
Improving access increases treatment consistency and success.
4. 🤝 Integrate Peer Support and Recovery Groups
Peer support programs can:
- Help individuals share experiences with TMS
- Normalize treatment participation
- Provide encouragement and accountability
Hearing from others who are in or have completed TMS can reduce fear and uncertainty.
5. 📋 Provide Navigation and Case Management Support
Navigating treatment can be overwhelming. Community-based case managers can assist with:
- Scheduling appointments
- Understanding insurance or payment options
- Coordinating care across providers
This support is especially important for individuals with complex needs.
6. 🏫 Reduce Stigma Through Community Engagement
Stigma remains a major barrier to treatment. Communities can:
- Promote addiction as a health condition, not a moral failure
- Highlight recovery success stories
- Encourage open conversations about mental health and treatment
Reducing stigma makes individuals more likely to seek help—including newer options like TMS.
Challenges to Consider
Even with strong community support:
- TMS may not be widely available in all areas
- Insurance coverage can be limited for addiction-specific use
- Awareness among providers may vary
Addressing these gaps requires continued advocacy and collaboration.
The Bigger Picture: A Community-Based Approach to Recovery
TMS represents innovation in addiction treatment—but innovation alone is not enough. Community resources ensure that individuals can access, understand, and sustain treatment.
When communities invest in education, access, and support, they transform TMS from a specialized service into a realistic recovery option.
Final Thoughts
Recovery doesn’t happen in isolation. It happens in clinics, homes, and communities, working together.
By strengthening community resource strategies, we can make treatments like TMS more accessible, more understood, and more effective—giving individuals struggling with meth addiction a stronger chance at lasting recovery.
Frequently Asked Questions
Here are some common questions:
1. What is TMS?
Answer:
Transcranial Magnetic Stimulation (TMS) is a non-invasive treatment that uses magnetic pulses to stimulate specific brain regions, particularly the prefrontal cortex, which is involved in decision-making, impulse control, and craving regulation.
2. How does TMS help with meth addiction?
Answer:
TMS targets brain circuits that are disrupted by meth use. It may help:
- Reduce cravings
- Improve self-control
- Restore more normal brain activity
By “rebalancing” these circuits, individuals may find it easier to resist urges and engage in recovery.
3. Is TMS FDA-approved for methamphetamine use disorder?
Answer:
Currently, TMS is FDA-approved for depression, not specifically for meth addiction. Its use for methamphetamine use disorder is considered off-label and still being researched, though early results are promising.
4. What does a TMS session feel like?
Answer:
Most people feel a tapping or tingling sensation on the scalp during treatment. It is generally not painful, and patients remain awake and alert throughout the session.
5. How long does TMS treatment take?
Answer:
A typical course includes:
- 20–40 minute sessions
- 5 days per week
- 4–6 weeks (or longer)
Consistency is important for effectiveness.
6. Are there side effects?
Answer:
TMS is generally well tolerated. Common side effects include:
- Mild headache
- Scalp discomfort
- Temporary fatigue
Serious side effects are rare.
7. Can TMS cure meth addiction?
Answer:
No. TMS is not a cure, but it can be a helpful tool in reducing cravings and supporting recovery. It works best when combined with:
- Therapy (e.g., CBT)
- Support systems
- Lifestyle changes
8. Who is a good candidate for TMS?
Answer:
TMS may be considered for individuals who:
- Struggle with persistent cravings
- Have not responded well to traditional treatments
- Are able to attend regular sessions
A healthcare provider determines eligibility.
9. Is TMS safe?
Answer:
Yes, TMS is considered safe and non-invasive. It does not require anesthesia and does not involve medications that affect the whole body.
10. Will insurance cover TMS for meth addiction?
Answer:
Coverage varies. While insurance often covers TMS for depression, it may not cover it for meth addiction because it is still considered experimental for this use.
11. Can TMS be combined with other treatments?
Answer:
Yes—and it should be. TMS is most effective when used alongside:
- Behavioral therapies
- Support groups
- Case management and recovery services
12. How quickly will I see results?
Answer:
Some individuals notice improvements in cravings or mood within a few weeks, but results vary. TMS works gradually, and progress may be subtle at first.
13. Does TMS help with relapse prevention?
Answer:
It may help reduce relapse risk by improving impulse control and decreasing craving intensity, but long-term success depends on ongoing recovery efforts.
14. Is TMS painful or invasive?
Answer:
No. TMS is non-invasive and does not involve surgery, needles, or sedation.
15. What happens after TMS treatment ends?
Answer:
Some individuals may:
- Transition to maintenance sessions
- Continue therapy and recovery programs
- Use learned coping strategies to maintain progress
Follow-up care is important for sustained recovery.
Conclusion
TMS offers a novel and potentially impactful approach to treating methamphetamine use disorder by focusing on the underlying brain circuitry that drives cravings and relapse. While research is still evolving, early findings suggest that TMS can reduce craving intensity and support improved self-regulation, especially when integrated into a comprehensive treatment plan. However, it is not a standalone solution—long-term recovery continues to depend on consistent engagement, psychosocial support, and access to resources. As understanding of TMS grows, it may become an important component of modern addiction treatment, providing new hope for individuals seeking recovery from meth addiction.
Video:

