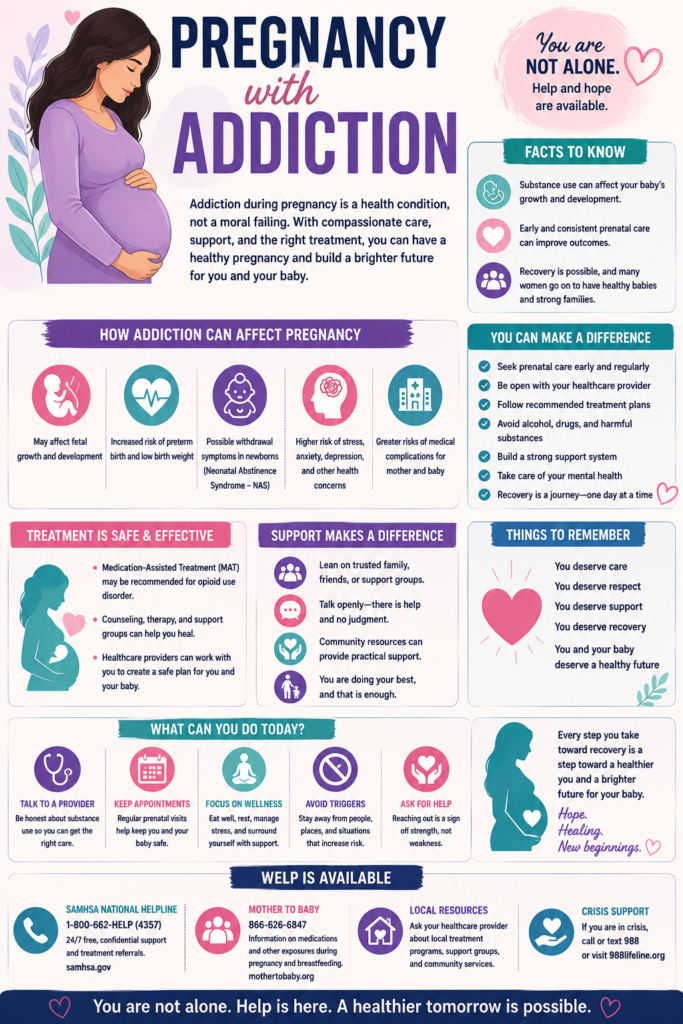
Pregnancy combined with addiction presents a unique and complex challenge, impacting both the expectant mother and her unborn child. The intertwining of addiction and pregnancy requires a comprehensive understanding of its pathology and specialized care. This exploration delves into the delicate balance that must be struck between the health of the mother and the well-being of the developing fetus. It addresses treatment options tailored to this specific population, highlighting the importance of self-care practices. Additionally, the vital roles of family support and community resources are emphasized in navigating this critical juncture, ultimately aiming for the best possible outcomes for both mother and child.
The Impact of Addiction During Pregnancy: Challenges and Support
Addiction during pregnancy can have serious and potentially life-altering effects on both the mother and the developing fetus. Understanding these impacts is essential for fostering awareness and providing effective support to those in need. Below are key ways addiction affects pregnancy:
Fetal Development
Teratogenic Effects: Substance use, particularly drugs like alcohol, nicotine, and certain illicit substances, can lead to teratogenic effects. These effects cause physical and developmental abnormalities in the fetus, including congenital disabilities and delayed development.
Complications for the Mother
Increased Risk of Maternal Health Issues: Substance use during pregnancy can exacerbate health conditions such as high blood pressure, anemia, and infections. These complications pose significant risks to both maternal and fetal health.
Neonatal Abstinence Syndrome (NAS)
Opioid Use: Babies born to mothers who use opioids during pregnancy may develop NAS. This condition causes newborns to experience withdrawal symptoms, requiring specialized medical care and extended hospital stays.
Low Birth Weight and Prematurity
Stunted Growth: Substance use during pregnancy can result in intrauterine growth restriction, leading to low birth weight and a higher likelihood of preterm delivery. These outcomes increase the risk of long-term health challenges for the child.
Cognitive and Behavioral Problems
Long-Term Cognitive Impairments: Prenatal exposure to substances can lead to cognitive and behavioral difficulties that may persist into adolescence and adulthood. These include challenges with learning, attention, and emotional regulation.
Emotional and Behavioral Challenges for the Mother
Guilt and Shame: Mothers struggling with addiction often experience intense guilt and shame. These emotions can affect their mental health and impede their ability to care for their newborns effectively.
Attachment and Bonding Difficulties
Attachment Issues: Addiction may hinder a mother’s ability to bond with her newborn, potentially leading to long-term emotional and psychological effects for the child.
Financial and Social Stressors
Strain on Resources: Addiction can create financial challenges, making it difficult to provide adequate care and support for both the mother and the child.
Legal Issues
Legal Consequences: In some jurisdictions, substance use during pregnancy may lead to legal consequences, including custody issues or criminal charges, further complicating the mother’s situation.
Stigmatization and Social Isolation
Social Stigma: Mothers facing addiction often encounter stigma, which can lead to social isolation and barriers to accessing necessary resources and support.
Seeking Help and Support
It is crucial for pregnant individuals struggling with addiction to seek professional help as early as possible. A comprehensive treatment plan that includes medical, psychological, and social support can significantly improve outcomes for both mother and baby. Creating a non-judgmental and supportive environment is essential to fostering recovery and promoting well-being.
By understanding these challenges, society can better support pregnant individuals dealing with addiction, ensuring healthier futures for both mothers and their children.
The Pathology of Addiction in Pregnant Mothers and Their Babies
The pathology of addiction in a pregnant mother and her baby involves a series of complex physiological and psychological processes. Below is a breakdown of the key factors and effects:
For the Pregnant Mother
Chemical Dependence: Addiction alters the brain’s chemistry, leading to chemical dependence. The body adapts to the presence of the substance, resulting in withdrawal symptoms when it is not consumed.
Compromised Decision-Making: Addiction can impair the mother’s ability to make rational decisions, often resulting in continued substance use despite awareness of its harmful effects.
Placental Barrier: Many substances, including drugs and alcohol, can cross the placental barrier, directly affecting the developing fetus.
Impaired Prenatal Care: Substance addiction may result in inadequate prenatal care, as the mother may be less likely to seek or follow medical advice and attend regular check-ups.
Stress and Mental Health Issues: Addiction often coexists with mental health conditions, leading to chronic stress and emotional instability. These stressors can negatively impact both the mother and the developing fetus.
For the Developing Fetus
Fetal Exposure: Substances consumed by the mother, including drugs, alcohol, and nicotine, cross the placenta and directly affect fetal development.
Intrauterine Growth Restriction (IUGR): Substance use during pregnancy can lead to IUGR, where the fetus does not grow at the expected rate. This condition may result in low birth weight and developmental challenges.
Neonatal Abstinence Syndrome (NAS): When the mother is addicted to opioids, the baby may experience withdrawal symptoms after birth, known as NAS. This condition requires specialized care and monitoring.
Neurodevelopmental Effects: Substance exposure can lead to altered brain development, potentially causing cognitive and behavioral issues that may persist into childhood.
Organ Damage: Certain substances have the potential to cause direct damage to the developing organs of the fetus.
Long-Term Effects: The effects of prenatal substance exposure may not always be immediately apparent. Cognitive, behavioral, and physical challenges can manifest later in childhood or adolescence.
Risk of Sudden Infant Death Syndrome (SIDS): Prenatal substance exposure is associated with an increased risk of SIDS, posing an additional threat to the newborn’s survival.
Influencing Factors
The specific effects of addiction during pregnancy depend on:
- Type of Substance: Different substances have varied impacts on the mother and fetus.
- Dosage: Higher doses of substances generally result in greater risks.
- Timing of Exposure: Exposure at different stages of pregnancy affects different aspects of development.
- Individual Factors: Genetic and environmental factors can influence outcomes.
Importance of Early Intervention
Early intervention is crucial to minimizing harm. Comprehensive prenatal care combined with substance use treatment can significantly improve outcomes for both the mother and the baby. A supportive and non-judgmental approach is essential in helping pregnant individuals access the care they need.
By understanding the pathology of addiction in pregnancy, healthcare providers and society can work towards creating safer, healthier futures for mothers and their children.
Treatment Management Strategies for Pregnant Women with Addiction
The treatment management strategies for pregnant women with addiction involve a comprehensive and multidisciplinary approach to ensure the health and well-being of both the mother and the developing fetus. Below are the key components of such a strategy:
Specialized Prenatal Care
Pregnant women with addiction should receive specialized prenatal care that addresses the unique challenges they face. This care may involve more frequent check-ups, additional monitoring, and specific assessments related to substance use.
Medically-Assisted Treatment (MAT)
For opioid addiction, medically-assisted treatment using substances like methadone or buprenorphine may be recommended. These medications help stabilize the mother’s addiction while minimizing harm to the fetus.
Behavioral Therapy
Cognitive-behavioral therapy (CBT) and other forms of behavioral therapy are highly effective in treating addiction. They help the mother identify triggers, develop coping strategies, and modify addictive behaviors.
Support Groups and Counseling
Engaging in support groups, such as 12-step programs or other addiction-focused counseling, provides a sense of community and peer support. This can be invaluable during the recovery process.
Nutritional Support
Proper nutrition is crucial for the health of both the mother and the developing fetus. A dietitian can help ensure the mother receives essential nutrients to support a healthy pregnancy.
Mental Health Support
Addressing co-occurring mental health conditions is vital. This may involve therapy, counseling, or, in severe cases, medication under careful medical supervision to ensure the safety of both mother and baby.
Screening for Infectious Diseases
Pregnant women with addiction are at higher risk for certain infections. Regular screening and appropriate treatment are essential to prevent complications and protect both the mother and the fetus.
Fetal Monitoring
Monitoring the growth and development of the fetus through ultrasounds and other medical tests helps ensure that any issues are identified and addressed promptly.
Safe Environment
Creating a safe and stable living environment for the pregnant woman is crucial. It should be free from triggers or sources of stress that could lead to relapse.
Social Support and Networking
Encouraging the mother to build a strong support network—including family, friends, and community resources—can provide essential assistance during the recovery process.
Education and Skill-Building
Providing education on parenting, stress management, and addiction recovery empowers the mother to make positive choices for herself and her child. Skills training can also help prepare her for the challenges of parenthood.
Postpartum Planning
Planning for the postpartum period is essential. This includes:
- Discussing breastfeeding options, as some medications used in treatment may not be compatible with breastfeeding.
- Ensuring continued addiction support to maintain recovery.
Individualized Treatment Plans
Every case is unique, and individualized treatment plans are crucial. Close collaboration between healthcare providers, addiction specialists, mental health professionals, and obstetricians is essential for achieving the best possible outcomes for both mother and baby.
By adopting a comprehensive approach, pregnant women with addiction can receive the support they need to achieve healthier futures for themselves and their children.
Self-Care Strategies for Pregnant Women with Addiction
Self-care is an integral part of the treatment management for pregnant women with addiction. It helps support their physical, emotional, and mental well-being, which in turn benefits the health of both the mother and the developing fetus. Here are some self-care strategies for pregnant women with addiction:
Healthy Nutrition
Eating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients for both the mother and the baby. A dietitian can help create a personalized meal plan.
Regular Exercise
Engaging in regular, moderate exercise, under the guidance of a healthcare provider, can improve mood, reduce stress, and promote overall well-being.
Adequate Rest and Sleep
Getting enough rest is crucial for physical and emotional health. Practicing good sleep hygiene can help improve the quality of sleep.
Stress Reduction Techniques
Techniques such as deep breathing exercises, meditation, yoga, and mindfulness can help reduce stress levels and promote relaxation.
Avoiding Triggers
Identifying and avoiding situations, places, or people that may trigger cravings or relapse is important for maintaining sobriety.
Hydration
Staying well-hydrated is important for overall health. Water helps support bodily functions and can also help manage cravings.
Regular Medical Check-ups
Attending all prenatal appointments and follow-up visits with healthcare providers is crucial for monitoring the health of both the mother and the baby.
Mindfulness and Self-reflection
Engaging in practices that promote self-awareness and self-reflection can help the mother understand her emotions and thought patterns, making it easier to address any challenges that may arise.
Creative Expression
Engaging in creative activities like art, writing, or music can be therapeutic and provide an outlet for emotional expression.
Educational Pursuits
Engaging in educational activities or hobbies that the mother enjoys can help boost confidence and provide a sense of accomplishment.
Social Support
Maintaining connections with supportive friends and family members can help alleviate feelings of isolation and provide emotional support.
Engaging in Relaxation Techniques
Practices like progressive muscle relaxation, guided imagery, or taking warm baths can help the mother relax and reduce tension.
Setting Realistic Goals
Establishing achievable short-term and long-term goals can provide a sense of purpose and direction.
In summary, remember, self-care is not selfish; it’s an essential part of maintaining overall health and well-being, especially during pregnancy and addiction recovery. It’s important for the mother to prioritize her own health to be in the best position to care for her baby.
The Role of Family Support in Supporting Pregnant Women with Addiction
Family support is crucial for pregnant women with addiction, as it can provide the necessary encouragement, understanding, and assistance needed during this challenging time. Here are some family support management strategies:
Open Communication
Maintain open and honest communication with the pregnant woman. Listen without judgment and express empathy and understanding.
Education and Awareness
Learn about addiction and its effects on pregnancy. Understanding the challenges the woman is facing can help family members offer more effective support.
Accompany to Medical Appointments
Offer to accompany the pregnant woman to prenatal and addiction treatment appointments. This provides emotional support and helps ensure that all medical advice is understood and followed.
Provide a Stable Environment
Create a stable and nurturing home environment that minimizes stressors and triggers that could contribute to relapse.
Assist with Daily Tasks
Help with daily responsibilities, such as grocery shopping, meal preparation, and household chores, to reduce the woman’s stress and workload.
Offer Encouragement
Provide positive reinforcement for milestones and achievements in both addiction recovery and pregnancy. Celebrate small victories.
Be a Source of Strength
Offer emotional support and be a source of strength during difficult moments. Remind the woman of her worth and capabilities.
Respect Boundaries
Understand that the pregnant woman may need space at times. Respect her boundaries and allow her to communicate her needs.
Participate in Family Therapy
Attend family therapy sessions or support groups together. This can provide a safe space for open communication and healing.
Encourage Healthy Habits
Encourage and participate in healthy activities together, such as exercise, mindfulness practices, or creative hobbies.
Learn Coping Strategies
Educate yourselves about healthy coping strategies for stress, anxiety, and triggers. This knowledge can be applied to support the pregnant woman.
Plan for the Future
Discuss and plan for the arrival of the baby. Consider practical matters like childcare, living arrangements, and financial stability.
Avoid Enabling Behaviors
While providing support, it’s important to avoid enabling addictive behaviors. Encourage healthy choices and offer alternatives.
Seek Professional Guidance
If the family is struggling to provide the necessary support, consider involving a therapist or counselor who specializes in addiction and family dynamics.
In summary, supporting a pregnant woman with addiction can be emotionally demanding. It’s important for family members to also take care of their own well-being and seek support when needed. By working together, families can play a crucial role in helping both the mother and the baby thrive.
Community Support Strategies for Pregnant Women with Addiction
Community resources play a vital role in supporting pregnant women with addiction. Below are some key treatment management strategies provided by communities:
Prenatal Care Programs
Communities often offer specialized prenatal care programs that cater to pregnant women struggling with addiction. These programs provide comprehensive medical care, addiction treatment, and support tailored to the unique needs of these women.
Addiction Treatment Centers
Access to addiction treatment centers equipped to handle pregnant women is crucial. These centers can provide a range of services, including detoxification, counseling, and medication-assisted treatment.
Support Groups for Pregnant Women
Community-based support groups specifically for pregnant women facing addiction can be immensely helpful. These groups offer a safe and non-judgmental space for sharing experiences, receiving encouragement, and accessing resources.
Parenting and Life Skills Classes
Many communities offer classes focused on parenting and life skills. These programs help pregnant women build important skills essential for both addiction recovery and parenting.
Transportation Assistance
Reliable transportation is crucial for attending medical appointments, treatment sessions, and support groups. Communities may offer transportation services or subsidies to ensure pregnant women can get where they need to go.
Housing and Shelter Services
Stable housing is a fundamental need for pregnant women dealing with addiction. Communities may provide resources for temporary or transitional housing, offering stability during this critical time.
Legal Aid and Advocacy Services
Some pregnant women with addiction may face legal challenges. Community resources can include legal aid services that help navigate issues such as custody arrangements or legal troubles related to addiction.
Nutrition and Food Assistance Programs
Ensuring that pregnant women have access to nutritious food is essential for both maternal and fetal health. Communities may have programs that provide food assistance to pregnant women in need.
Mental Health Services
Access to mental health services, including counseling and therapy, is crucial for pregnant women dealing with addiction. Communities may have clinics or organizations offering mental health support.
Childcare Services
Once the baby arrives, childcare support becomes essential. Communities may have resources for affordable childcare options, allowing the mother to attend treatment and support sessions.
Recovery Coaching and Peer Support
Connecting pregnant women with trained recovery coaches or peers who have overcome addiction themselves can provide invaluable support and motivation.
Substance-Free Activities and Events
Communities may organize substance-free activities and events that provide opportunities for pregnant women to socialize, engage in healthy activities, and build a supportive network.
In summary. by providing a range of comprehensive resources, communities can significantly enhance the chances of a healthy pregnancy for women struggling with addiction. These resources help create a supportive environment that empowers women to seek treatment, make positive choices, and ultimately provide the best start for their babies.
Frequently Asked Questions and Answers
What does “pregnancy with addiction” mean?
It refers to substance use or addiction occurring during pregnancy, including the misuse of alcohol, nicotine, opioids, prescription medications, or other drugs.
Can addiction affect pregnancy?
Yes. Substance use during pregnancy can affect both the pregnant person and the developing baby.
What substances are most commonly involved?
Common substances include alcohol, nicotine, opioids, methamphetamine, cocaine, marijuana, and prescription drug misuse.
Can addiction during pregnancy harm the baby?
Yes. Risks may include premature birth, low birth weight, developmental problems, and withdrawal symptoms after birth.
What is Neonatal Abstinence Syndrome (NAS)?
NAS occurs when a baby experiences withdrawal symptoms after exposure to certain substances, especially opioids, during pregnancy.
Can alcohol use during pregnancy be dangerous?
Yes. Alcohol exposure during pregnancy can lead to fetal alcohol spectrum disorders (FASDs), affecting growth, learning, and development.
Does smoking or vaping affect pregnancy?
Yes. Nicotine use may increase the risk of premature birth, low birth weight, and breathing problems in newborns.
Why do some pregnant individuals struggle with addiction?
Addiction is a medical condition influenced by mental health, trauma, stress, genetics, and environmental factors.
Can stress and trauma increase substance use during pregnancy?
Yes. Anxiety, depression, trauma, domestic violence, and emotional distress may increase the risk of substance use.
Is it safe to stop substances suddenly during pregnancy?
Not always. Some substances should only be stopped under medical supervision because withdrawal can be dangerous.
Can treatment during pregnancy help?
Yes. Early medical care and addiction treatment can improve health outcomes for both parent and baby.
What treatments are available?
Treatment may include prenatal care, counseling, therapy, medication-assisted treatment (MAT), support groups, and mental health services.
What is medication-assisted treatment (MAT)?
MAT combines medications with counseling and behavioral support to help manage opioid addiction safely during pregnancy.
Can pregnant individuals recover from addiction?
Yes. Recovery is possible with healthcare support, treatment, family encouragement, and community resources.
Why is prenatal care important?
Regular prenatal care helps monitor the health of both parent and baby while supporting safer pregnancy outcomes.
Can mental health care help during recovery?
Yes. Treating anxiety, depression, trauma, and stress can improve emotional wellness and recovery success.
How can loved ones support someone pregnant and struggling with addiction?
Offer compassion, avoid judgment, encourage treatment, and help connect them with healthcare and support services.
Can addiction increase emotional challenges during pregnancy?
Yes. Individuals may experience guilt, fear, anxiety, depression, or isolation while navigating pregnancy and recovery.
What should someone do if they are pregnant and using substances?
Seek medical care as soon as possible and speak honestly with a healthcare provider to receive safe, supportive treatment.
Where can someone find help during pregnancy and addiction recovery?
People can contact healthcare providers, treatment centers, or the SAMHSA National Helpline for confidential support and treatment resources.
Conclusion
Navigating pregnancy while dealing with addiction demands a multifaceted approach, recognizing the intricate interplay between maternal well-being and fetal health. Understanding the underlying pathology is key, enabling tailored treatments that prioritize the safety of both mother and child. The significance of self-care practices cannot be overstated, offering a foundation for healthier outcomes. Equally crucial is the unwavering support of family members, and the availability of community resources provides an essential safety net. By synergizing these elements, we strive for the best possible start in life for both mother and baby, setting the stage for a brighter future.
Video: