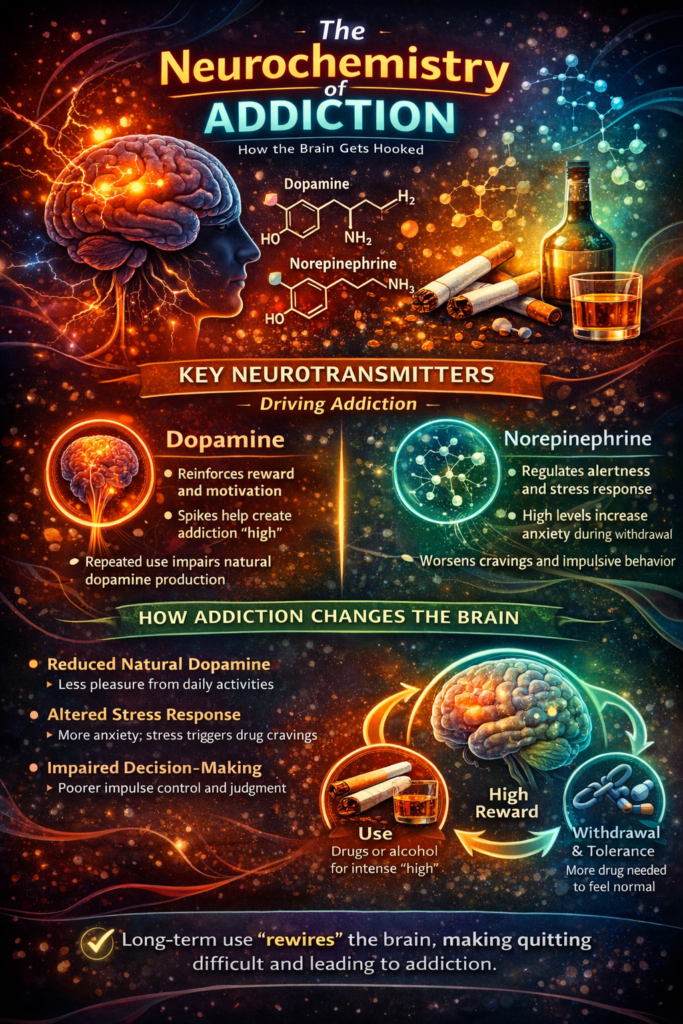
The neurochemistry of addiction provides a scientific framework for understanding why substance use can become compulsive and difficult to control. Rather than being a simple matter of choice, addiction involves significant changes in brain function—particularly in systems that regulate reward, motivation, and stress. Neurotransmitters such as dopamine and norepinephrine play central roles in reinforcing substance use and shaping behavioral patterns over time. As these systems become altered through repeated exposure, the brain begins to prioritize substance use over natural rewards, making quitting both physically and psychologically challenging. Exploring the neurochemical basis of addiction helps shift the perspective from blame to biology, offering a more informed approach to treatment and recovery.
The Neurochemistry of Addiction: How the Brain Becomes Dependent
Addiction is not simply a matter of willpower—it is a complex brain-based condition shaped by changes in neurochemistry. Substances like nicotine, alcohol, and stimulants alter the brain’s communication systems, particularly those involved in reward, motivation, and stress. At the center of this process are key neurotransmitters such as dopamine, which reinforces pleasurable behaviors, and norepinephrine, which influences arousal and alertness. Over time, repeated substance use reshapes these systems, making the brain increasingly reliant on the substance to feel normal. Understanding the neurochemistry of addiction provides critical insight into why quitting is so difficult and why relapse is common, even after periods of abstinence.
The Brain’s Reward System
The brain is wired to repeat behaviors that promote survival, such as eating and social bonding. This is largely controlled by the dopamine reward pathway, particularly in regions such as the nucleus accumbens. When a person uses an addictive substance, dopamine is released in much higher amounts than natural rewards, creating a powerful sense of pleasure and reinforcement.
Over time:
- The brain reduces its natural dopamine production
- Receptors become less sensitive
- Every day activities feel less rewarding
This leads to a cycle where the substance is needed just to feel “normal.”
Dopamine: The Reinforcement Chemical
Dopamine is often misunderstood as the “pleasure chemical,” but it is more accurately tied to motivation and learning. It teaches the brain to repeat behaviors associated with reward.
In addiction:
- Dopamine spikes strengthen the association between substance use and reward
- Environmental cues (like stress or certain places) trigger cravings
- The brain prioritizes the substance over other needs
Norepinephrine and Stress
Norepinephrine plays a key role in the body’s stress response and alertness. During withdrawal, levels of norepinephrine can become dysregulated, leading to:
- Anxiety
- Irritability
- Increased heart rate
- Difficulty concentrating
This stress response is a major driver of relapse, as individuals may use substances to relieve these uncomfortable symptoms.
Neuroadaptation and Dependence
With repeated use, the brain undergoes neuroadaptation—it adjusts to the presence of the substance. This includes:
- Tolerance (needing more to achieve the same effect)
- Dependence (needing the substance to function normally)
- Withdrawal symptoms when the substance is absent
These changes are not temporary; they can persist long after substance use stops.
The Role of the Prefrontal Cortex
Addiction also affects the prefrontal cortex, the area responsible for decision-making, impulse control, and judgment.
As addiction progresses:
- Impulse control weakens
- Decision-making becomes impaired
- Long-term consequences are undervalued
This helps explain why individuals may continue using despite knowing the risks.
Recovery and Brain Plasticity
The brain is not permanently damaged—it can heal through neuroplasticity. With sustained abstinence and supportive interventions:
- Dopamine systems can gradually recover
- Stress responses become more regulated
- Cognitive control improves
However, this process takes time, which is why early recovery can feel especially difficult.
Conclusion
The neurochemistry of addiction reveals that substance dependence is rooted in real, measurable changes in brain function. Dopamine-driven reinforcement, stress-related neurotransmitters like norepinephrine, and impaired decision-making all contribute to the persistence of addictive behaviors. Recognizing addiction as a neurobiological condition—not a moral failing—shifts the focus toward effective, compassionate treatment approaches. Ultimately, understanding how the brain adapts to addiction is key to developing strategies that support long-term recovery and resilience.
Understanding the Neurochemistry of Addiction: Self-Management Strategies for Change
Addiction is rooted in powerful changes within the brain’s chemistry, particularly involving neurotransmitters like dopamine and norepinephrine. These systems influence reward, motivation, stress, and habit formation—making it difficult to simply “choose” to stop using a substance. However, understanding these neurochemical processes can empower individuals to take a more strategic, self-management approach to recovery. By aligning daily behaviors with the brain’s healing and adaptation, it becomes possible to gradually restore balance and reduce dependence.
Why Self-Management Matters
Recovery is not a single event but an ongoing process of retraining the brain. Because addiction alters reward pathways and stress responses, self-management strategies help:
- Stabilize brain chemistry
- Reduce triggers and cravings
- Strengthen new, healthier neural pathways
These strategies work by supporting neuroplasticity, the brain’s ability to reorganize and recover over time.
1. Regulating Dopamine Naturally
Since addiction overstimulates dopamine, recovery involves rebuilding the brain’s natural reward system.
- Engage in regular physical activity (boosts dopamine gradually)
- Set small, achievable goals to create consistent rewards
- Limit overstimulating behaviors (e.g., excessive screen time, junk food)
This helps the brain relearn how to experience pleasure from everyday activities.
2. Managing Stress and Norepinephrine
Heightened stress responses can trigger cravings and relapse. Regulating norepinephrine is key.
- Practice deep breathing or mindfulness techniques
- Maintain a consistent sleep schedule
- Use grounding strategies during moments of anxiety
Lowering stress reduces the brain’s urge to seek relief through substances.
3. Rewiring Habit Loops
Addiction creates strong associations between cues and behaviors.
- Identify triggers (people, places, emotions)
- Replace old habits with healthier alternatives
- Interrupt automatic behaviors with conscious pauses
Over time, new neural pathways weaken the old addiction cycle.
4. Strengthening the Prefrontal Cortex
The prefrontal cortex supports decision-making and impulse control, which are often impaired in addiction.
- Practice delayed gratification (waiting before acting on cravings)
- Use journaling to reflect on choices and consequences
- Develop structured daily routines
These strategies improve self-control and long-term thinking.
5. Building Consistency Over Intensity
The brain responds best to repeated, consistent behaviors.
- Focus on small daily improvements rather than drastic changes
- Track progress to reinforce motivation
- Accept setbacks as part of the learning process
Consistency helps solidify new neural connections.
6. Supporting Brain Recovery Holistically
Physical health directly impacts brain chemistry.
- Eat a balanced diet to support neurotransmitter production
- Stay hydrated
- Prioritize sleep and recovery
These foundational habits create the conditions for neurological healing.
Important Considerations
While self-management is powerful, it is not always sufficient on its own.
- Severe addiction may require professional treatment
- Withdrawal symptoms can be intense and should be monitored
- Support systems (therapy, groups, family) improve outcomes
Combining self-management with external support often leads to the best results.
A Brain-Based Approach to Recovery
Understanding the neurochemistry of addiction shifts the focus from blame to biology. Instead of asking, “Why can’t I stop?” a more effective question becomes, “How can I support my brain in healing?” This perspective encourages practical, science-based strategies that align with how the brain actually works.
Conclusion
Self-management strategies grounded in the neurochemistry of addiction offer a practical path toward recovery. By regulating dopamine, managing stress, and consistently reinforcing healthier behaviors, individuals can gradually reshape their brain’s reward system and regain control. Recovery is not about instant change—it is about steady, intentional progress that allows the brain to heal and adapt over time.
Family Support and the Neurochemistry of Addiction: Strategies for Understanding and Healing
Addiction is not simply a behavioral issue—it is a condition rooted in changes to brain chemistry, particularly in systems involving dopamine, norepinephrine, and stress regulation. For families, understanding these neurochemical processes can transform how they respond to a loved one struggling with addiction. Rather than viewing substance use as a lack of willpower, families can recognize it as a brain-based condition that requires patience, structure, and informed support. By aligning their approach with the science of addiction, family members can play a powerful role in recovery.
Why Family Understanding Matters
When addiction is misunderstood, responses often include frustration, blame, or attempts to control behavior. However, these reactions can increase stress and worsen the cycle of addiction. Understanding the neurochemistry helps families:
- Recognize cravings as biologically driven, not purely voluntary
- Respond with empathy rather than judgment
- Support long-term brain recovery rather than short-term compliance
This shift in perspective creates a more supportive and effective environment for change.
1. Reducing Stress and Supporting Regulation
Because addiction disrupts stress systems (involving norepinephrine), high-conflict environments can intensify cravings and relapse risk.
- Maintain a calm, predictable home environment
- Avoid escalating arguments during emotional moments
- Encourage healthy coping strategies like breathing or taking breaks
Lower stress supports stabilization of the brain’s chemistry.
2. Reinforcing Healthy Dopamine Pathways
Addiction hijacks the brain’s reward system, making substances feel more rewarding than everyday life.
Families can help by:
- Encouraging positive activities (exercise, hobbies, social connection)
- Celebrating small achievements to reinforce natural rewards
- Participating in healthy routines together
These actions help rebuild the brain’s natural reward system.
3. Avoiding Shame and Blame
Shame can worsen addiction by increasing stress and lowering self-worth, which are both linked to relapse.
- Use supportive language instead of criticism
- Focus on behavior, not personal character
- Acknowledge effort, even when progress is slow
This approach aligns with how the brain responds to reinforcement and stress.
4. Supporting the Prefrontal Cortex (Decision-Making)
Addiction weakens the brain’s ability to make controlled, long-term decisions.
Families can support this by:
- Encouraging structured routines
- Helping set realistic goals
- Offering reminders without controlling or micromanaging
Structure strengthens cognitive control over time.
5. Encouraging Consistency and Patience
Neurochemical recovery takes time. The brain does not reset overnight.
- Understand that mood swings and irritability are part of recovery
- Avoid expecting immediate or perfect change
- Reinforce consistency rather than perfection
Patience supports long-term neural healing.
6. Seeking Education and External Support
Families benefit from learning more about addiction science and accessing resources.
- Attend family therapy or educational programs
- Join support groups for families (e.g., Al-Anon or similar)
- Consult professionals when needed
Education reduces confusion and improves communication.
Important Considerations
While family support is powerful, it has limits.
- Families cannot “fix” addiction alone
- Professional treatment may be necessary
- Boundaries are essential to prevent burnout and codependency
Healthy support includes both compassion and appropriate limits.
A Brain-Based Approach to Family Support
Understanding the neurochemistry of addiction allows families to shift from reacting emotionally to responding strategically. Instead of asking, “Why are they doing this?” families can begin to ask, “What is their brain going through, and how can we support recovery?”
Conclusion
Family support, when grounded in an understanding of brain chemistry, becomes a powerful tool in addiction recovery. By reducing stress, reinforcing healthy behaviors, and responding with empathy rather than judgment, families can help create the conditions necessary for healing. Addiction may change the brain, but with informed, consistent support, recovery is possible—and families can be a vital part of that process.
Community Resources and the Neurochemistry of Addiction: Strategies for Education and Support
Understanding the neurochemistry of addiction—how substances alter dopamine, norepinephrine, and brain function—can be a powerful tool in recovery. However, this knowledge is often difficult to apply without support. Community resources play a critical role in bridging the gap between scientific understanding and real-world change. By providing education, structure, and accessible services, communities help individuals and families translate brain-based knowledge into effective recovery strategies.
Why Community Resources Matter
Addiction affects not only individuals but entire communities. Access to reliable resources helps people:
- Understand addiction as a brain-based condition, not a moral failure
- Learn practical strategies aligned with how the brain heals
- Build supportive networks that reduce isolation
Community-based support strengthens both knowledge and long-term recovery outcomes.
1. Educational Programs and Workshops
Community education is key to understanding the neurochemistry of addiction.
- Local health departments and nonprofits often offer workshops on addiction science
- Universities and clinics may host seminars on brain function and substance use
- Online community courses can provide accessible, evidence-based information
These programs help individuals and families better understand cravings, withdrawal, and relapse from a biological perspective.
2. Support Groups and Peer Networks
Peer support reinforces learning through shared experience.
- Groups like Narcotics Anonymous (NA) or SMART Recovery
- Community-led discussion groups focused on addiction education
- Peer mentorship programs
Hearing others’ experiences helps connect neurochemical concepts (like dopamine-driven cravings) to real-life situations.
3. Access to Mental Health Services
Professional services help individuals apply neurochemical knowledge to behavior change.
- Therapists trained in addiction and cognitive-behavioral therapy (CBT)
- Counselors who incorporate neuroscience-informed approaches
- Community clinics offering low-cost or sliding-scale services
These resources support the regulation of stress systems and the development of coping skills.
4. Public Health Initiatives
Community-wide efforts can reduce addiction triggers and improve recovery environments.
- Smoking cessation programs and quitlines
- Awareness campaigns about addiction as a medical condition
- Policies promoting smoke-free or substance-free environments
These initiatives align with neurochemical recovery by reducing exposure to cues and reinforcing healthier norms.
5. Harm Reduction and Outreach Services
Harm reduction programs meet individuals where they are while promoting safety.
- Education on substance effects and risks
- Access to safe-use information and support services
- Outreach programs connecting individuals to treatment options
These services acknowledge the realities of addiction while supporting gradual change.
6. Creating Supportive Community Environments
Communities can foster conditions that support brain healing.
- Access to recreational spaces, exercise programs, and wellness activities
- Community centers offering structured routines and social engagement
- Programs that reduce stressors like unemployment or housing instability
Stable environments help regulate stress-related neurochemistry and reduce relapse risk.
Important Considerations
While community resources are valuable, challenges remain:
- Access may be limited in some areas
- Not all programs are equally evidence-based
- Individuals may need to try multiple resources to find the right fit
Combining community support with professional care often leads to the best outcomes.
A Community-Based Perspective on Addiction
Understanding the neurochemistry of addiction shifts the narrative from blame to biology. Community resources extend this understanding beyond individuals, creating a culture of informed support, empathy, and effective intervention. When communities are educated, they become better equipped to respond to addiction in ways that promote healing rather than stigma.
Conclusion
Community resource strategies are essential for translating the science of addiction into meaningful change. Through education, peer support, mental health services, and supportive environments, communities can help individuals understand and manage the neurochemical processes underlying addiction. Recovery is not just an individual effort—it is a collective process shaped by the knowledge, resources, and support systems available within the community.
Frequently Asked Questions
Here are some common questions:
1. What is the neurochemistry of addiction?
It refers to how repeated substance use alters brain chemicals (neurotransmitters) and neural pathways, leading to changes in behavior, motivation, and control.
2. Which neurotransmitters are most involved in addiction?
The key ones include:
- Dopamine – linked to reward and motivation
- Norepinephrine – involved in stress and arousal
- Serotonin – affects mood and emotional regulation
- GABA and glutamate regulate brain activity and learning
3. Why is dopamine so important in addiction?
Dopamine reinforces behaviors by signaling reward. Addictive substances cause large dopamine spikes, teaching the brain to repeat substance use and prioritize it over natural rewards.
4. How does addiction change the brain over time?
Repeated use leads to:
- Reduced natural dopamine production
- Decreased receptor sensitivity
- Stronger habit pathways
- Impaired decision-making
These changes make quitting difficult and increase relapse risk.
5. What role does norepinephrine play in addiction?
Norepinephrine regulates stress and alertness. During withdrawal, it can become overactive, causing anxiety, irritability, and physical symptoms that drive relapse.
6. Why do people experience cravings?
Cravings are driven by:
- Learned associations (triggers like places or emotions)
- Dopamine signaling that “remembers” the reward
- Stress-related brain activity
The brain essentially “reminds” the person to seek the substance.
7. Is addiction a disease or a choice?
Addiction is considered a chronic brain disorder. While initial use may be voluntary, repeated use changes brain chemistry, reducing control over time.
8. What is tolerance?
Tolerance occurs when the brain adapts to a substance, requiring larger amounts to achieve the same effect due to neurochemical changes.
9. What is withdrawal?
Withdrawal happens when the substance is removed, and the brain struggles to function normally. Symptoms can include:
- Anxiety
- Irritability
- Cravings
- Physical discomfort
10. How does addiction affect decision-making?
It weakens the prefrontal cortex, which controls impulse regulation and judgment. This makes it harder to resist urges despite negative consequences.
11. Can the brain recover from addiction?
Yes, through neuroplasticity:
- Dopamine systems can gradually rebalance
- Brain function can improve over time
- New, healthier habits can form
However, recovery takes time and consistent effort.
12. Why is relapse common?
Relapse occurs because:
- Brain changes persist after stopping use
- Triggers and stress can reactivate cravings
- The reward system remains sensitive to the substance
13. How does stress influence addiction?
Stress activates brain systems that increase craving and reduce self-control, making individuals more likely to return to substance use.
14. What helps restore brain chemistry during recovery?
Helpful strategies include:
- Healthy routines (sleep, nutrition, exercise)
- Therapy and support groups
- Stress management techniques
- Avoiding triggers
15. Why is understanding neurochemistry important?
It helps:
- Reduce stigma and blame
- Improve treatment approaches
- Empower individuals with science-based strategies
Conclusion
Understanding the neurochemistry of addiction highlights that substance dependence is rooted in real, measurable changes within the brain. These changes affect not only how individuals experience pleasure and stress but also how they make decisions and regulate behavior. Recognizing addiction as a brain-based condition underscores the importance of evidence-based interventions, long-term support, and patience in the recovery process. While the brain can gradually heal through neuroplasticity, this process takes time and consistent effort. Ultimately, a neurochemical perspective not only deepens our understanding of addiction but also supports more compassionate, effective strategies for helping individuals achieve and maintain recovery.
Video: Why Addiction Feels Impossible to Break (Science Explains) #psychology #addiction #brainfacts