Genetic risk plays a significant role in understanding addiction and the cycle of relapse, yet it is often misunderstood or overlooked. Individuals with a family history of substance use may inherit biological traits that affect how their brains respond to stress, reward, and cravings. These inherited vulnerabilities can complicate the recovery process, particularly when faced with emotional triggers or high-stress situations. Recognizing that relapse is not simply a matter of willpower, but rather a combination of biological, psychological, and environmental factors, allows for a more informed and compassionate approach to recovery.
Genetic Risk and the Cycle of Relapse: Understanding the Biological Connection
Introduction: More Than Just Willpower
Relapse is often misunderstood as a lack of discipline or motivation, but research shows it is far more complex. One of the most important—and often overlooked—factors is genetic risk. Individuals with a family history of addiction may inherit biological vulnerabilities that influence how their brains respond to stress, reward, and substances. Understanding this genetic component helps shift the perspective from blame to awareness, allowing for more effective and compassionate recovery strategies.
What Is Genetic Risk in Addiction?
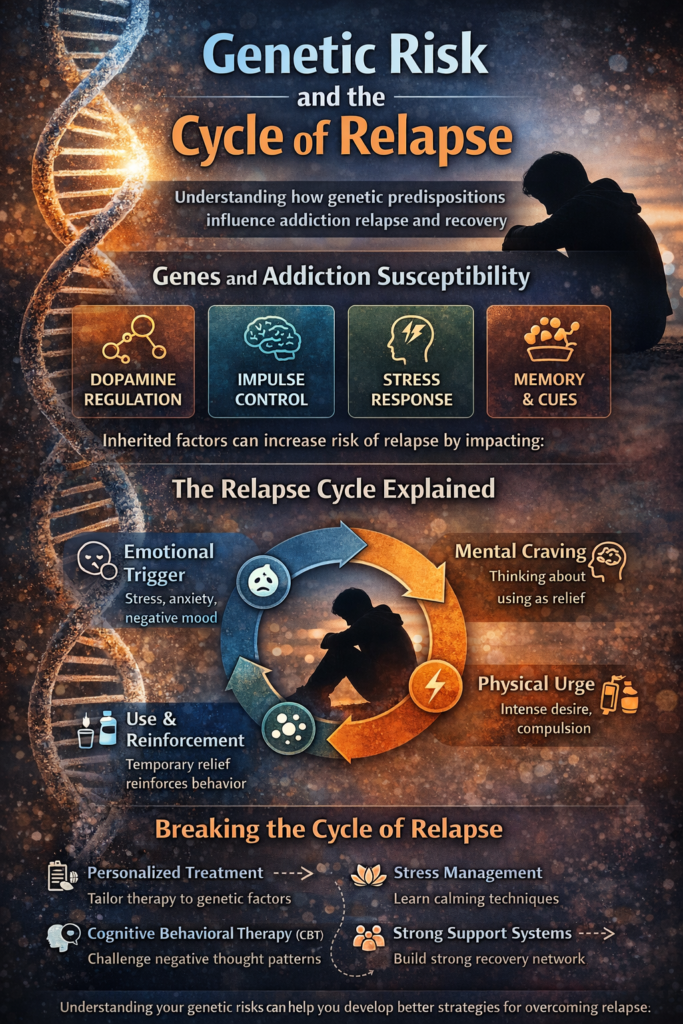
Genetic risk refers to inherited traits that increase the likelihood of developing substance use disorders. These traits can affect:
- Dopamine regulation, influencing how strongly someone experiences pleasure or reward
- Stress response systems, making some individuals more sensitive to anxiety or distress
- Impulse control impacts decision-making and risk-taking behaviors
While genetics do not determine destiny, they can create a predisposition that makes recovery more challenging without proper support.
How Genetics Influence the Cycle of Relapse
1. Heightened Reward Sensitivity
Some individuals are genetically wired to experience stronger reinforcement from substances. This makes cravings more intense and increases the likelihood of returning to use after periods of abstinence.
2. Increased Stress Reactivity
Genetic predisposition can amplify the body’s response to stress. Since stress is a major trigger for relapse, individuals with higher reactivity may struggle more during difficult situations.
3. Slower Emotional Regulation
Genetic factors can impact the brain’s ability to regulate emotions effectively. This can lead to:
- Difficulty coping with anxiety or depression
- Increased reliance on substances for relief
- Greater vulnerability during emotional distress
4. Memory and Cue Sensitivity
The brain’s reward system forms strong associations between substances and environmental cues. For some, genetic factors strengthen these associations, making triggers (people, places, emotions) more powerful.
The Relapse Cycle Explained
The cycle of relapse often follows a pattern:
- Emotional Trigger (stress, anxiety, or negative mood)
- Mental Craving (thoughts about using as relief)
- Physical Urge (intense desire or compulsion)
- Use and Reinforcement (temporary relief reinforces the behavior)
Genetic risk can intensify each stage of this cycle, making it harder to interrupt without targeted strategies.
Breaking the Cycle: Strategies That Work
1. Personalized Treatment Approaches
Understanding genetic risk allows for tailored interventions, including therapy and, when appropriate, medication-assisted treatment.
2. Stress Management Skills
Since stress is a major trigger, learning techniques like mindfulness, breathing exercises, and structured routines can reduce vulnerability.
3. Cognitive Behavioral Therapy (CBT)
CBT helps individuals recognize and challenge thought patterns that lead to relapse, strengthening mental resilience.
4. Strong Support Systems
Family, peers, and recovery communities provide accountability and emotional support, which can counterbalance biological vulnerabilities.
5. Education and Awareness
Knowing that relapse risk may be influenced by genetics can reduce shame and encourage proactive coping strategies.
Reframing Relapse: From Failure to Feedback
Relapse should not be viewed as a failure, but as a signal that something in the recovery plan needs adjustment. For individuals with higher genetic risk, this may mean increasing support, refining coping strategies, or addressing underlying mental health conditions more directly.
Conclusion: Knowledge as a Tool for Recovery
Genetic risk does not guarantee relapse, but it can shape the path of recovery. By understanding how biology interacts with behavior, individuals can take a more informed and compassionate approach to their healing process. Recovery is not about overcoming genetics—it’s about working with that knowledge to build stronger, more effective strategies. With the right tools and support, even those with higher genetic vulnerability can achieve lasting sobriety.—
Understanding Genetic Risk and the Cycle of Relapse: Self-Management Strategies for Lasting Recovery
Introduction: Taking Control of What You Can
Genetic risk can play a significant role in addiction and relapse, influencing how the brain responds to stress, reward, and cravings. While you cannot change your genetic makeup, you can change how you respond to it. Self-management strategies empower individuals to better understand their vulnerabilities and actively interrupt the cycle of relapse. By combining awareness with practical tools, recovery becomes more intentional, personalized, and sustainable.
Understanding Your Genetic Risk
Genetic predisposition does not guarantee relapse—it simply means there may be a heightened sensitivity to certain triggers, such as stress, emotional discomfort, or environmental cues. Recognizing this risk allows you to:
- Anticipate high-risk situations
- Respond proactively instead of reactively
- Reduce shame by understanding the biological component of addiction
Awareness transforms genetic risk from a limitation into a guide for smarter recovery strategies.
How the Relapse Cycle Connects to Self-Management
The relapse cycle—emotional triggers, cravings, urges, and use—can be intensified by genetic factors. Self-management focuses on interrupting this cycle early, especially at the emotional and cognitive stages where change is most effective.
Self-Management Strategies to Break the Cycle
1. Identify Personal Triggers Early
Pay attention to patterns:
- When do cravings increase?
- What emotions are present (stress, boredom, anxiety)?
- Are certain people or environments involved?
Tracking these patterns helps you intervene before cravings escalate.
2. Strengthen Emotional Regulation Skills
Since genetic risk may heighten emotional reactivity, building regulation skills is essential:
- Practice mindfulness to observe emotions without reacting
- Use breathing techniques to calm the nervous system
- Label emotions clearly (“I’m feeling anxious, not in danger”)
This reduces impulsive responses linked to relapse.
3. Reframe Cravings as Temporary Signals
Cravings are not commands—they are temporary brain responses. Try:
- Reminding yourself that cravings pass within minutes
- Distracting yourself with a healthy activity
- Viewing cravings as information, not failure
This mindset reduces the power cravings hold.
4. Use Cognitive Strategies to Challenge Thoughts
Genetic vulnerability can amplify negative thinking patterns. Counter them by asking:
- Is this thought accurate or exaggerated?
- What evidence do I have?
- What would I tell someone else in this situation?
This interrupts the mental stage of relapse.
5. Build Structured Routines
Routine creates stability, which is especially important for individuals with higher biological sensitivity to stress:
- Consistent sleep and meal schedules
- Planned daily activities
- Regular recovery meetings or check-ins
Structure reduces uncertainty and emotional overwhelm.
6. Develop a Personalized Coping Plan
Prepare for high-risk moments in advance:
- List coping strategies you can use when triggered
- Identify people you can reach out to
- Create a “pause plan” before acting on urges
Having a plan reduces impulsive decision-making.
7. Prioritize Physical Health
Biology plays a key role in recovery, so supporting your body matters:
- Regular exercise improves mood regulation
- Balanced nutrition stabilizes energy and brain function
- Sleep supports emotional control and stress resilience
Physical health strengthens your ability to manage genetic risk.
8. Stay Connected to Support Systems
Even with strong self-management, connection is critical:
- Peer support groups
- Therapy or counseling
- Trusted friends or family
Support adds accountability and perspective during vulnerable moments.
From Vulnerability to Strength
Understanding genetic risk can feel overwhelming at first, but it also provides clarity. Instead of asking “Why is this so hard?”, you can ask “What strategies work best for me?” This shift encourages self-compassion and proactive problem-solving.
Conclusion: Empowerment Through Awareness and Action
Genetic risk may influence the relapse cycle, but it does not determine your outcome. Through self-management strategies—such as emotional regulation, cognitive awareness, and structured routines—you can interrupt the relapse cycle and build resilience over time. Recovery is not about eliminating vulnerability; it’s about learning how to navigate it effectively. With knowledge, preparation, and consistent effort, long-term sobriety is not only possible—it is sustainable.—
Family Strategies for Understanding Genetic Risk and the Cycle of Relapse
Introduction: The Family’s Role in Recovery
Addiction does not only affect the individual—it impacts the entire family system. When genetic risk is part of the picture, families may struggle with questions like “Did we pass this down?” or “Why does relapse keep happening?” Understanding that addiction and relapse can be influenced by inherited biological factors helps shift the focus away from blame and toward support. Families who recognize these dynamics are better equipped to respond with empathy, structure, and effective strategies that promote long-term recovery.
Understanding Genetic Risk as a Family
Genetic risk means that certain individuals may be more vulnerable to addiction and relapse due to inherited traits affecting stress response, reward sensitivity, and emotional regulation. For families, this understanding can:
- Reduce guilt and shame on both sides
- Normalize repeated struggles in recovery
- Encourage proactive, informed support strategies
It’s important to remember: genetics increases risk, but they do not determine outcomes.
How Families Can Recognize the Cycle of Relapse
Relapse is often a gradual process, not a single event. Families may notice:
- Emotional changes (irritability, anxiety, withdrawal)
- Mental preoccupation (talking about past use, romanticizing substances)
- Behavioral shifts (isolation, breaking routines, avoiding support)
Recognizing these early warning signs allows families to intervene with support before relapse occurs.
Family Strategies to Support Recovery and Reduce Relapse Risk
1. Educate Yourself About Addiction and Genetics
Understanding the biological aspects of addiction helps families move away from blame-based thinking. Learning about how genetics influences cravings, stress, and relapse creates a more compassionate and realistic perspective.
2. Replace Blame With Empathy
Instead of asking “Why can’t you just stop?”, try:
- “I see you’re struggling—how can I support you?”
- “We’re in this together.”
Empathy reduces shame, which is a major trigger for relapse.
3. Support Early Intervention
If you notice warning signs of relapse:
- Gently bring up your observations
- Encourage open conversation without accusation
- Suggest reconnecting with support systems (therapy, meetings)
Early support can interrupt the relapse cycle before it escalates.
4. Encourage Healthy Coping Strategies
Families can reinforce positive behaviors by:
- Participating in stress-reducing activities together (walks, routines)
- Supporting therapy or counseling attendance
- Encouraging healthy structure in daily life
This helps counteract biological vulnerabilities.
5. Set and Maintain Healthy Boundaries
Support does not mean enabling. Clear boundaries:
- Protect family well-being
- Encourage accountability
- Reduce patterns that may unintentionally support relapse
For example, avoiding covering up the consequences of substance use is crucial.
6. Promote Consistency and Stability
A predictable environment can reduce stress and anxiety:
- Maintain routines at home
- Communicate clearly and calmly
- Minimize unnecessary conflict
Stability helps regulate emotional responses linked to relapse risk.
7. Address Family-Wide Patterns
Genetic risk often overlaps with learned behaviors and family dynamics. Consider:
- Family therapy
- Open discussions about patterns of coping and communication
- Breaking cycles of avoidance or conflict
Healing the system supports the individual.
8. Take Care of Your Own Well-Being
Supporting someone in recovery can be emotionally demanding. Family members should:
- Seek their own support (e.g., Al-Anon or counseling)
- Practice self-care
- Avoid neglecting their own needs
Healthy families provide stronger support.
Reframing Relapse as Part of the Process
For families, relapse can feel discouraging or even personal. However, understanding genetic risk helps reframe relapse as part of a complex process rather than a failure. Each setback can provide insight into triggers, coping gaps, and areas needing more support.
Conclusion: Strengthening Recovery Through Family Understanding
Families play a critical role in shaping recovery outcomes. By understanding genetic risk and the cycle of relapse, they can shift from frustration to informed support. Through education, empathy, boundaries, and consistency, families become a stabilizing force that helps interrupt relapse patterns and promote long-term healing. Recovery is not just an individual journey—it’s a shared process, and when families are equipped with the right tools, everyone moves forward together.
Community Resource Strategies for Understanding Genetic Risk and the Cycle of Relapse
Introduction: Recovery Is Stronger With Community Support
Understanding genetic risk in addiction can feel overwhelming—for individuals and their families alike. Knowing that biology may increase vulnerability to relapse can raise concerns about long-term success. However, recovery is not determined by genetics alone. Community resources play a critical role in helping individuals understand these risks and develop effective strategies to manage them. Through education, connection, and structured support, communities provide the tools needed to break the cycle of relapse and build sustainable recovery.
Why Community Resources Matter in Genetic Risk and Relapse
Genetic predisposition can influence how strongly someone reacts to stress, cravings, and environmental triggers. Community resources help by:
- Providing education about the biological aspects of addiction
- Offering support systems that reduce isolation
- Teaching coping strategies to manage triggers
- Creating accountability and structure
These resources bridge the gap between biological vulnerability and practical recovery tools.
Community Strategies to Address Genetic Risk and Relapse
1. Access to Dual-Diagnosis Treatment Programs
Many community-based programs specialize in treating both substance use and mental health conditions. These programs:
- Address anxiety, depression, and stress linked to relapse
- Provide integrated care tailored to individual risk factors
- Help individuals understand how genetics and mental health interact
2. Peer Support and Recovery Groups
Groups such as 12-step programs or recovery communities offer:
- Shared experiences that normalize relapse struggles
- Insight into how others manage cravings and triggers
- Consistent support and accountability
Hearing others with similar vulnerabilities can reduce shame and increase motivation.
3. Educational Workshops and Seminars
Community organizations often host sessions on:
- The science of addiction and genetic risk
- Understanding the relapse cycle
- Practical coping and prevention strategies
Education empowers individuals to make informed decisions and recognize early warning signs.
4. Access to Counseling and Therapy Services
Local clinics and mental health centers provide evidence-based treatments like:
- Cognitive Behavioral Therapy (CBT)
- Relapse prevention therapy
- Trauma-informed care
Professional guidance helps individuals develop personalized strategies based on their risk level.
5. Recovery Community Centers
These centers create a structured environment where individuals can:
- Participate in group activities and workshops
- Build healthy social connections
- Practice coping strategies in real-life settings
They offer a sense of belonging that counteracts isolation—a key trigger for relapse.
6. Digital and Online Support Platforms
Online communities and apps expand access to support:
- Virtual meetings and forums
- Educational content on addiction and genetics
- Immediate connection during high-risk moments
These tools are especially helpful when in-person resources are limited.
7. Crisis Support and Hotlines
Community-based crisis services provide immediate assistance during intense cravings or emotional distress. They:
- Offer real-time support
- Help de-escalate high-risk situations
- Connect individuals to additional local resources
Overcoming Barriers to Community Support
Despite their value, some individuals may hesitate to use community resources due to:
- Stigma surrounding addiction
- Fear of judgment or vulnerability
- Lack of awareness or accessibility
Addressing these barriers—through education and gradual engagement—can open the door to meaningful support.
From Genetic Risk to Informed Action
Community resources help reframe genetic risk from a fixed limitation into something manageable. By learning how biology interacts with the environment and behavior, individuals can take proactive steps to reduce the risk of relapse.
Instead of asking “Am I destined to relapse?”, the focus shifts to “What tools and support systems can help me succeed?”
Conclusion: Community as a Protective Factor
While genetic risk can influence the cycle of relapse, it does not define the outcome of recovery. Community resources provide the education, structure, and connection needed to navigate these challenges effectively. By engaging with supportive networks and evidence-based programs, individuals can interrupt relapse patterns and build resilience over time. Recovery is not just an individual effort—it is strengthened by community, where shared knowledge and support turn vulnerability into opportunity for lasting change.
Frequently Asked Questions
Here are some common questions:
1. What does “genetic risk” mean in addiction?
Genetic risk refers to inherited traits that increase a person’s likelihood of developing substance use disorders. These traits can affect how the brain processes reward, stress, and impulse control. It does not mean someone is destined to develop addiction—it simply indicates a higher vulnerability.
2. Does having a family history of addiction mean I will relapse?
No. A family history increases risk but does not determine outcomes. Many people with genetic vulnerability maintain long-term recovery. Environmental factors, coping skills, support systems, and treatment all play a major role in reducing the risk of relapse.
3. How do genetics influence the relapse cycle?
Genetics can intensify key parts of the relapse cycle by:
- Increasing sensitivity to stress
- Strengthening cravings and reward responses
- Making emotional regulation more difficult
- Enhancing memory of substance-related cues
These factors can make triggers feel more intense and harder to manage without proper strategies.
4. What is the “cycle of relapse”?
The relapse cycle is a process that typically includes:
- Emotional triggers (stress, anxiety, negative mood)
- Mental cravings (thinking about using)
- Physical urges (strong desire or compulsion)
- Use and reinforcement (temporary relief reinforces behavior)
Understanding this cycle helps individuals intervene earlier.
5. Can genetic risk be tested?
There are some genetic tests that claim to assess addiction risk, but they are not widely used as standalone tools in clinical practice. Family history remains one of the most reliable indicators. Genetics is complex and involves many interacting factors, not a single “addiction gene.”
6. Why do some people relapse more easily than others?
Differences in genetics, mental health, environment, and coping skills all contribute. Individuals with higher genetic sensitivity to stress or reward may experience stronger cravings or emotional reactions, increasing relapse vulnerability.
7. Can the relapse cycle be prevented if you have a genetic risk?
It cannot always be completely prevented, but it can be managed and interrupted. Strategies like therapy, stress management, structured routines, and strong support systems significantly reduce relapse risk—even for those with higher genetic vulnerability.
8. How does stress relate to genetic risk and relapse?
Many individuals with a genetic predisposition have a heightened stress response. Since stress is a major trigger in the relapse cycle, this increased sensitivity can make it more difficult to cope without substances unless effective coping strategies are developed.
9. What role does treatment play in managing genetic risk?
Treatment helps tailor strategies to individual needs. This may include:
- Cognitive Behavioral Therapy (CBT)
- Medication-assisted treatment (when appropriate)
- Relapse prevention planning
- Mental health support
Personalized treatment is especially important when genetic risk is present.
10. Is relapse a failure if genetics are involved?
No. Relapse is not a failure—it is a signal that something in the recovery plan needs adjustment. Understanding genetic risk helps reframe relapse as part of a complex process rather than a personal weakness.
11. Can lifestyle changes reduce genetic risk?
Yes. While genetics cannot be changed, lifestyle factors can influence how genes are expressed (a concept known as epigenetics). Healthy habits such as exercise, sleep, nutrition, and stress management can improve resilience and reduce the risk of relapse.
12. How can I use knowledge of genetic risk to strengthen my recovery?
You can use this knowledge to:
- Be more proactive about triggers
- Develop strong coping strategies early
- Stay consistent with treatment and support
- Practice self-compassion instead of blame
Awareness allows you to plan ahead rather than react in the moment.
Conclusion
While genetic risk can increase susceptibility to relapse, it does not determine an individual’s outcome. Understanding the connection between biology and behavior provides an opportunity to develop targeted strategies that interrupt the cycle of relapse. With awareness, proper support, and effective coping skills, individuals can manage their vulnerabilities and build resilience over time. Recovery is not about overcoming genetics, but about working with that knowledge to create a sustainable path forward—one that emphasizes growth, adaptability, and long-term stability.
Video: