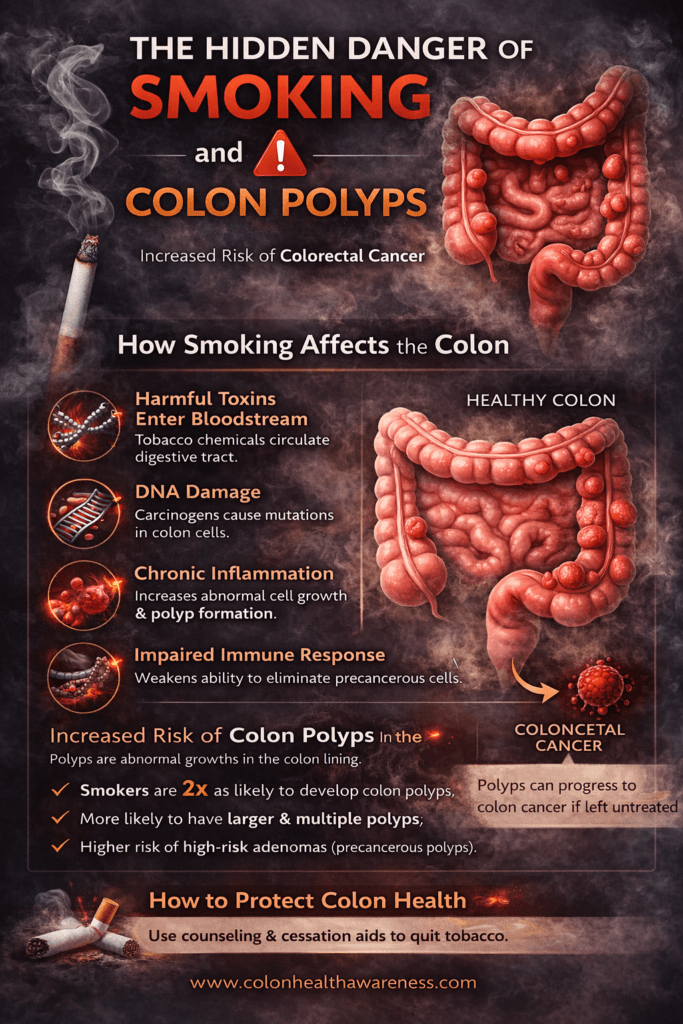
Smoking affects more than the lungs and can lead to colon polyps. Although many polyps are noncancerous, some can develop into colorectal cancer. Because polyps often have no early symptoms, quitting smoking and regular screenings are important for prevention.
The Hidden Danger of Smoking and Colon Polyps
How Tobacco Use Quietly Increases Colorectal Cancer Risk
When people think of smoking-related diseases, lung cancer and heart disease usually come to mind. However, one lesser-known but significant risk involves the digestive system — particularly the development of colon polyps. The connection between smoking and colon polyps is often overlooked, yet it carries serious implications for colorectal cancer prevention.
Understanding this hidden danger can empower individuals to make informed health decisions and reduce long-term cancer risk.
What Are Colon Polyps?
Colon polyps are abnormal growths that form on the inner lining of the colon or rectum. While many polyps are benign (noncancerous), some can develop into colorectal cancer over time.
There are different types of polyps, including:
- Adenomatous polyps (adenomas) – These have the highest potential to become cancerous.
- Hyperplastic polyps – Usually low risk but may signal increased susceptibility in certain cases.
- Sessile serrated polyps – Often harder to detect and can carry a significant cancer risk.
The progression from polyp to cancer can take years, which makes early detection through colonoscopy highly effective in prevention.
How Smoking Contributes to Colon Polyp Formation
Smoking affects far more than the lungs. When tobacco smoke is inhaled, harmful chemicals enter the bloodstream and circulate throughout the body, including the digestive tract.
Research suggests smoking contributes to polyp development through several mechanisms:
1. DNA Damage
Tobacco contains carcinogens that damage cellular DNA, increasing mutation rates in colon cells.
2. Chronic Inflammation
Smoking promotes systemic inflammation, which can disrupt normal cell growth and repair processes.
3. Altered Gut Microbiome
Tobacco exposure may influence gut bacteria, affecting colon health and immune response.
4. Impaired Immune Surveillance
The immune system plays a role in eliminating abnormal cells. Smoking weakens this protective function.
Over time, these effects increase the likelihood of abnormal cell growth in the colon.
Increased Risk of Advanced and Multiple Polyps
Studies show that smokers are more likely to:
- Develop multiple polyps
- Develop larger polyps
- Develop high-risk adenomas
- Experience recurrence of polyps after removal
Long-term smokers, particularly those who began smoking at a young age or who smoke heavily, face a significantly elevated risk.
Even former smokers may carry a higher risk compared to individuals who have never smoked, although quitting reduces long-term cancer risk substantially.
The Link to Colorectal Cancer
In many cases, colon polyps are considered precancerous lesions. Smoking not only increases polyp formation but also raises the risk that these polyps will progress to colorectal cancer.
Colorectal cancer is one of the most common cancers worldwide, yet it is also one of the most preventable through screening and lifestyle changes.
Smoking is a modifiable risk factor — meaning it is one that individuals can change.
Additional Risk Factors That Compound the Danger
Smoking combined with other risk factors increases concern:
- Family history of colorectal cancer
- Obesity
- A diet high in processed meats
- Sedentary lifestyle
- Excessive alcohol consumption
- Type 2 diabetes
When smoking overlaps with these factors, the cumulative risk rises significantly.
The Importance of Screening
Regular screening — particularly colonoscopy — can:
- Detect polyps early
- Remove precancerous growths
- Prevent progression to cancer
- Reduce mortality rates
Screening is generally recommended beginning at age 45 for average-risk adults, though earlier testing may be advised for those with additional risk factors such as smoking.
Individuals with a history of smoking may benefit from discussing personalized screening timelines with their healthcare provider.
Benefits of Quitting Smoking
Quitting smoking offers immediate and long-term health benefits:
- Reduced systemic inflammation
- Improved immune function
- Lower cancer risk over time
- Better surgical and recovery outcomes
- Improved overall gastrointestinal health
While past smoking cannot be undone, cessation significantly lowers future risk.
Final Reflection
The hidden connection between smoking and colon polyps highlights the far-reaching impact of tobacco use. Beyond the well-known risks to the lungs and heart, smoking quietly damages the digestive system, increasing the likelihood of precancerous growths and colorectal cancer.
Awareness is a powerful preventive tool. By understanding this connection, prioritizing screening, and considering smoking cessation, individuals can dramatically reduce their long-term cancer risk.
Sometimes the most dangerous effects of smoking are not the ones we see immediately — but the silent changes happening inside the body over time.
Self-Management Strategies to Avoid the Hidden Danger of Smoking and Colon Polyps
Protecting Colon Health Through Intentional Lifestyle Change
Smoking is widely known for its impact on lung and heart health, but fewer people recognize its connection to colon polyps — abnormal growths in the colon that can develop into colorectal cancer over time. Tobacco-related toxins circulate through the bloodstream, increasing inflammation, DNA damage, and abnormal cell growth in the digestive tract.
The good news is that smoking-related colon cancer risk is a modifiable risk factor. Through structured self-management strategies, individuals can significantly reduce their risk of developing colon polyps and their progression to colorectal cancer.
Below are practical, evidence-informed approaches for prevention.
1. Commit to Smoking Cessation
The most impactful strategy is quitting smoking.
Self-Management Techniques:
- Set a quit date and create a written plan.
- Use nicotine replacement therapy (patches, gum, lozenges).
- Consult a healthcare provider about medications.
- Track triggers (stress, social situations, boredom).
- Join support groups or cessation programs.
- Use digital quit-tracking apps.
Even long-term smokers benefit significantly from quitting. Over time, inflammation decreases and cancer risk declines.
2. Increase Screening Awareness
Early detection prevents cancer.
Action Steps:
- Begin colorectal cancer screening at age 45 (or earlier if high risk).
- Discuss smoking history with your physician.
- Follow recommended colonoscopy intervals.
- Do not delay follow-up appointments after polyp removal.
Colonoscopy allows for the removal of precancerous polyps before they progress.
3. Adopt an Anti-Inflammatory Diet
Smoking increases systemic inflammation. Nutrition can help counteract this effect.
Focus on:
- High-fiber foods (vegetables, fruits, legumes, whole grains)
- Leafy greens
- Omega-3 fatty acids (fish, flaxseed, walnuts)
- Limited processed meats
- Reduced red meat consumption
- Minimized ultra-processed foods
Fiber improves gut health and supports a balanced microbiome, which plays a role in colon protection.
4. Increase Physical Activity
Regular physical activity lowers the risk of colorectal cancer.
Recommendations:
- Aim for at least 150 minutes of moderate exercise per week.
- Incorporate strength training twice weekly.
- Reduce prolonged sitting time.
- Take short walking breaks during work hours.
Exercise reduces inflammation, improves insulin sensitivity, and supports immune function.
5. Maintain a Healthy Weight
Obesity is an independent risk factor for colon polyps and colorectal cancer.
Self-Management Focus:
- Track body mass index (BMI).
- Monitor waist circumference.
- Set gradual weight-loss goals if needed.
- Combine diet and exercise consistently.
Weight management enhances metabolic and immune health.
6. Limit Alcohol Consumption
Excessive alcohol intake increases colorectal cancer risk.
Guidelines:
- Limit to moderate levels (up to one drink per day for women, two for men).
- Consider abstaining if multiple risk factors are present.
- Replace alcohol with non-alcoholic alternatives during social events.
Combining smoking and heavy alcohol use significantly compounds risk.
7. Strengthen Emotional Regulation Skills
Many individuals smoke as a stress-management tool. Addressing emotional triggers reduces relapse risk.
Alternative Coping Tools:
- Deep breathing exercises
- Progressive muscle relaxation
- Journaling
- Counseling or therapy
- Social support networks
Stress reduction supports long-term cessation success.
8. Monitor Gastrointestinal Symptoms
Be proactive about digestive health.
Watch for:
- Rectal bleeding
- Persistent abdominal pain
- Changes in bowel habits
- Unexplained weight loss
- Ongoing fatigue
Report symptoms promptly to a healthcare provider.
9. Understand Your Personal Risk Profile
Risk increases with:
- Family history of colorectal cancer
- Long-term smoking history
- Sedentary lifestyle
- High processed meat intake
- Type 2 diabetes
Discuss personalized prevention strategies with a healthcare professional.
The Long-Term Perspective
Smoking-related colon damage often develops silently over the years. Self-management is about consistent daily habits rather than short-term changes.
Every positive health decision — quitting smoking, scheduling screenings, improving diet, increasing physical activity — reduces cumulative risk.
Final Reflection
The connection between smoking and colon polyps may not be widely discussed, but it represents a serious and preventable health concern. Self-management strategies empower individuals to interrupt the progression from tobacco exposure to precancerous growth.
Quitting smoking is the single most protective step. Combined with screening, nutrition, physical activity, and stress management, individuals can dramatically reduce the hidden risks affecting their digestive health.
Prevention is not dramatic — it is deliberate. And small, consistent actions today protect the colon for years to come.
Family Support Strategies to Avoid the Hidden Danger of Smoking and Colon Polyps
How Families Can Protect Colon Health and Reduce Cancer Risk
Smoking is commonly associated with lung disease and heart problems, but many families are unaware of its connection to colon polyps — abnormal growths in the colon that can develop into colorectal cancer over time. Tobacco toxins circulate throughout the body, contributing to DNA damage, chronic inflammation, and impaired immune function, all of which increase the risk of precancerous colon changes.
Prevention does not rest solely on the individual. Families play a powerful role in reducing smoking-related health risks and encouraging early detection. Below are structured family support strategies that promote long-term colon health and lower cancer risk.
1. Support Smoking Cessation Without Shame
Quitting smoking is the most effective way to reduce colon polyp risk.
Family Strategies:
- Offer encouragement rather than criticism.
- Avoid guilt-based pressure.
- Celebrate small milestones (one week, one month smoke-free).
- Help identify triggers and create healthier coping alternatives.
- Encourage medical support or cessation programs.
Shame increases stress and relapse risk. Support increases motivation and accountability.
2. Encourage Regular Colorectal Screening
Screening is one of the most effective cancer prevention tools available.
Family Strategies:
- Remind loved ones to schedule screenings starting at age 45 (or earlier if high risk).
- Discuss family medical history openly.
- Offer transportation or attend appointments for support.
- Encourage follow-up if polyps are detected.
Early removal of polyps prevents progression to cancer.
3. Create a Smoke-Free Home Environment
Even secondhand smoke exposes family members to harmful toxins.
Family Strategies:
- Establish clear no-smoking policies inside the home and vehicles.
- Remove smoking paraphernalia.
- Model non-smoking behavior for children.
- Educate younger family members about long-term risks.
Smoke-free homes reduce exposure and normalize healthier habits.
4. Promote a Colon-Healthy Diet as a Family
Smoking increases inflammation; nutrition can help counterbalance this effect.
Family Nutrition Strategies:
- Increase fiber-rich foods (vegetables, fruits, whole grains, legumes).
- Limit processed and red meats.
- Reduce ultra-processed food consumption.
- Prepare balanced meals together.
- Encourage hydration.
Shared meals reinforce both health and connection.
5. Encourage Physical Activity Together
Exercise lowers colorectal cancer risk and reduces relapse triggers for smoking.
Family Strategies:
- Schedule weekly family walks.
- Engage in active hobbies together.
- Reduce sedentary time.
- Set shared fitness goals.
Physical activity improves immune function and reduces inflammation.
6. Address Emotional Triggers as a Family
Many individuals smoke as a stress-management tool. Family conflict or chronic stress can increase relapse risk.
Supportive Approaches:
- Maintain open communication.
- Practice calm problem-solving.
- Encourage healthy stress outlets (exercise, journaling, therapy).
- Reduce household tension where possible.
Emotional stability strengthens cessation success.
7. Share Health Education Openly
Knowledge reduces denial.
Families can:
- Discuss how smoking affects not only the lungs but also the digestive system.
- Review credible health information together.
- Normalize medical checkups as preventive care.
When families understand the full scope of smoking’s impact, motivation increases.
8. Recognize and Respond to Warning Signs
Encourage loved ones to seek medical care if they experience:
- Persistent abdominal discomfort
- Rectal bleeding
- Changes in bowel habits
- Unexplained weight loss
- Ongoing fatigue
Prompt medical evaluation can prevent serious complications.
The Long-Term Family Perspective
Colon polyps and colorectal cancer often develop silently over years. Family support provides continuity — reinforcing healthy habits consistently rather than sporadically.
When families create environments that promote:
- Smoking cessation
- Preventive screening
- Balanced nutrition
- Physical activity
- Emotional support
They reduce cumulative health risks significantly.
Final Reflection
The hidden danger of smoking extends beyond visible respiratory damage. Its effects on the colon can quietly increase cancer risk over time. Families are uniquely positioned to interrupt this trajectory.
Through encouragement, structure, and shared commitment to health, families can transform prevention into a collective effort. Supporting smoking cessation and proactive screening today protects not only one individual but the long-term well-being of the entire family system.
Prevention is strongest when it is practiced together.
Community Resource Strategies to Avoid the Hidden Danger of Smoking and Colon Polyps
Strengthening Public Health Efforts to Prevent Colorectal Cancer
Smoking is widely recognized as a cause of lung disease and cardiovascular illness, yet its connection to colon polyps and colorectal cancer remains under-discussed in many communities. Tobacco toxins circulate throughout the body, contributing to inflammation, DNA damage, and abnormal cell growth in the colon, increasing the risk of precancerous polyps.
Preventing smoking-related colon disease requires more than individual effort. Community-level interventions play a crucial role in education, prevention, access to screening, and long-term health promotion. Below are structured community strategies designed to reduce the hidden risks associated with smoking and colon polyps.
1. Public Smoking Cessation Programs
Accessible smoking cessation resources significantly reduce cancer risk across populations.
Community Initiatives:
- Free or low-cost nicotine replacement therapy (patches, gum).
- Local support groups and behavioral counseling.
- Mobile health clinics offering cessation services.
- Public awareness campaigns about long-term cancer risks.
- Partnerships with pharmacies and healthcare providers.
Communities that invest in cessation services reduce both smoking rates and future colorectal cancer incidence.
2. Expand Access to Colorectal Cancer Screening
Screening prevents cancer by detecting and removing polyps early.
Community Strategies:
- Host local screening awareness events.
- Provide transportation assistance for colonoscopy appointments.
- Offer low-cost or subsidized screening programs.
- Partner with employers to promote preventive health benefits.
- Educate high-risk populations, including current and former smokers.
Screening beginning at age 45 for average-risk adults has proven effective in reducing mortality.
3. Community Education Campaigns
Many individuals are unaware that smoking affects digestive health.
Educational Focus Areas:
- The link between tobacco use and colon polyps.
- Early warning signs of colorectal cancer.
- Benefits of smoking cessation.
- The importance of fiber-rich diets and physical activity.
Community education reduces stigma and increases proactive health behaviors.
4. Promote Healthy Lifestyle Programs
Smoking risk compounds with poor diet, obesity, and sedentary behavior.
Community-Based Health Programs:
- Nutrition workshops focused on fiber-rich diets.
- Farmers’ market partnerships to increase access to fresh produce.
- Community walking clubs or fitness initiatives.
- Workplace wellness programs.
- School-based nutrition education.
Addressing multiple lifestyle factors amplifies prevention efforts.
5. Policy and Environmental Interventions
Policy-level changes shape community norms.
Examples:
- Smoke-free public spaces.
- Tobacco taxation and regulation.
- Restrictions on advertising targeting youth.
- Funding for preventive health services.
- Health insurance coverage mandates for screening.
Policy changes create long-term population-level impact.
6. Target High-Risk and Underserved Populations
Certain groups experience higher smoking rates and lower screening access.
Community outreach may include:
- Mobile clinics in rural areas.
- Multilingual health education materials.
- Culturally tailored prevention programs.
- Collaboration with faith-based organizations.
- Employer-sponsored health outreach for high-risk industries.
Equitable access reduces health disparities.
7. Healthcare System Collaboration
Primary care providers and gastroenterologists can partner with community programs to:
- Screen for smoking history during routine visits.
- Refer patients to cessation services.
- Educate patients about colon cancer risk.
- Track follow-up compliance for polyp removal.
Integrated care improves continuity and outcomes.
Why Community Strategies Matter
Colon polyps and colorectal cancer often develop silently over years. Without structured prevention, high-risk individuals may remain unaware until the disease is advanced.
Community-level interventions provide:
- Early detection
- Accessible cessation resources
- Health literacy improvement
- Reduced stigma
- Population-wide risk reduction
Collective action strengthens preventive health outcomes.
Final Reflection
The hidden danger of smoking extends beyond the lungs. Its role in colon polyp formation and colorectal cancer highlights the need for comprehensive prevention strategies.
When communities invest in cessation programs, screening access, education, and policy change, they protect not just individuals — but entire populations. Preventing smoking-related colon disease is not solely a personal responsibility; it is a shared public health mission.
Long-term health improves when prevention becomes a community priority rather than an afterthought.
Frequently Asked Questions
Here are some common questions:
1. What are colon polyps?
Colon polyps are abnormal growths that develop on the inner lining of the colon or rectum. Most polyps are initially benign (noncancerous), but some types — particularly adenomatous and certain serrated polyps — can develop into colorectal cancer over time if not removed.
2. How is smoking connected to colon polyps?
Smoking exposes the body to carcinogens that travel through the bloodstream and reach the digestive tract. These toxins can:
- Damage to DNA in colon cells
- Increase chronic inflammation
- Weaken immune surveillance
- Promote abnormal cell growth
Over time, these effects raise the likelihood of polyp formation.
3. Does smoking increase the risk of colorectal cancer?
Yes. Smoking not only increases the risk of developing colon polyps but also raises the likelihood that those polyps will become cancerous. Long-term smokers face a higher risk of colorectal cancer compared to non-smokers.
4. Are former smokers still at risk?
Former smokers may continue to have an elevated risk compared to individuals who never smoked. However, quitting smoking significantly reduces long-term cancer risk over time. The earlier someone quits, the greater the health benefit.
5. Are colon polyps dangerous?
Not all polyps are dangerous, but some can become precancerous. Because polyps often produce no symptoms, they can grow silently for years before detection. That is why routine screening is essential.
6. What are the warning signs of colon polyps?
Most colon polyps cause no symptoms. However, potential warning signs may include:
- Rectal bleeding
- Changes in bowel habits
- Persistent abdominal discomfort
- Unexplained fatigue (from blood loss)
Many people only discover polyps during routine colonoscopy screening.
7. At what age should screening begin?
For average-risk adults, colorectal cancer screening is generally recommended starting at age 45. Individuals with additional risk factors — such as long-term smoking or family history — may need earlier screening. A healthcare provider can recommend personalized timelines.
8. How does smoking cause damage in the colon if smoke is inhaled into the lungs?
When tobacco smoke is inhaled, harmful chemicals enter the bloodstream. These toxins circulate throughout the body, including the colon. The digestive system is therefore exposed indirectly through systemic circulation.
9. Does secondhand smoke increase colon cancer risk?
Secondhand smoke contains many of the same carcinogens as direct smoking. While research primarily focuses on active smokers, reducing exposure to secondhand smoke is still important for overall cancer prevention.
10. Are e-cigarettes or vaping safer for colon health?
While vaping may reduce exposure to some combustion-related toxins, it still exposes users to chemicals that may have inflammatory and cellular effects. Long-term data regarding colon cancer risk is still developing. Avoiding tobacco and nicotine products altogether is the safest option.
11. What lifestyle changes reduce colon polyp risk?
In addition to quitting smoking, protective lifestyle changes include:
- Eating a high-fiber diet
- Limiting processed and red meats
- Maintaining a healthy weight
- Exercising regularly
- Limiting alcohol consumption
- Attending regular screenings
These strategies reduce inflammation and support colon health.
12. Can colon polyps be removed?
Yes. During a colonoscopy, doctors can often remove polyps immediately. Removing precancerous polyps significantly reduces the risk of developing colorectal cancer.
13. Is colorectal cancer preventable?
In many cases, yes. Because colorectal cancer often develops slowly from polyps, early detection and removal make it one of the most preventable cancers when screening guidelines are followed.
14. Why is this danger considered “hidden”?
The risk is considered hidden because:
- Smoking’s digestive effects are less publicly discussed.
- Colon polyps often cause no symptoms.
- Cancer may not develop until years after exposure.
The damage can progress silently, making awareness essential.
Conclusion
The hidden connection between smoking and colon polyps highlights the far-reaching effects of tobacco use beyond the respiratory system. While colon polyps may begin as benign growths, some can progress silently into colorectal cancer if left undetected. Fortunately, this risk is modifiable. Smoking cessation, routine colorectal screening, and healthy lifestyle choices significantly reduce long-term complications. By recognizing this often-overlooked danger, individuals can take proactive steps to protect their digestive health and lower their risk of cancer. Prevention begins with awareness — and awareness saves lives.
Video: