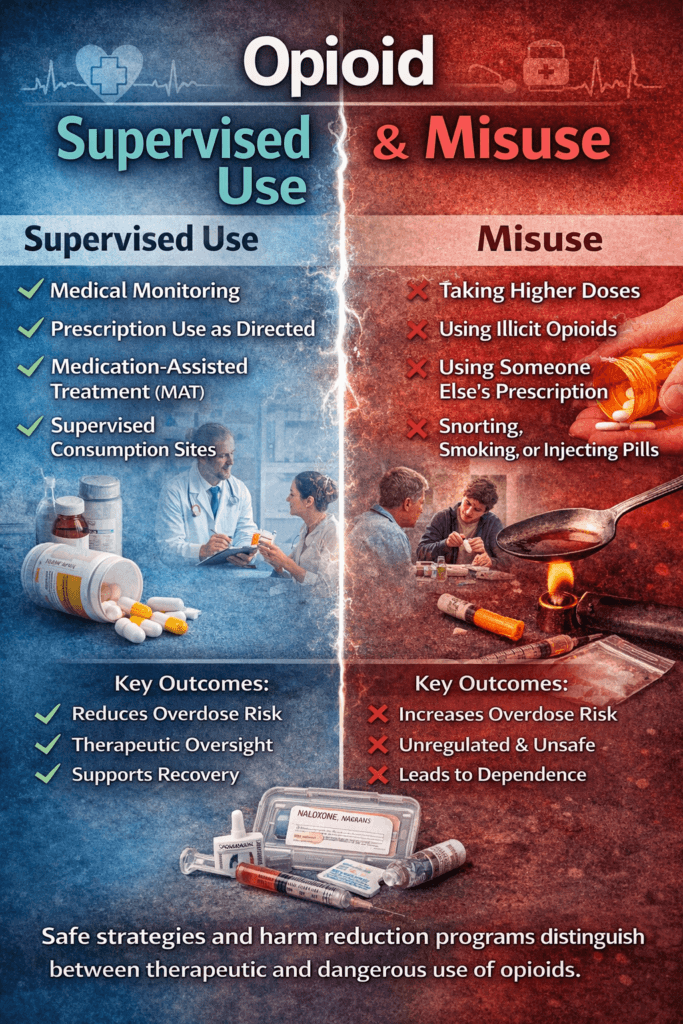
Understanding the difference between supervised opioid use and misuse is essential because context determines whether opioids help or harm. When prescribed and monitored by healthcare professionals, opioids can safely treat pain and support addiction treatment through careful dosing, monitoring, and adjustment. Misuse occurs when they are taken outside medical guidance, increasing the risk of dependence, overdose, and serious health complications. Recognizing this distinction promotes safer use, reduces stigma, and helps individuals and families make informed decisions about treatment and health.
Opioids Under Supervision vs. Misuse: Understanding the Critical Difference
Opioids occupy a unique space in medicine and public health because they can be both life-saving treatments and highly addictive substances. The difference between supervised use and misuse often determines whether opioids function as therapeutic tools or catalysts for harm. Understanding this distinction is essential for clinicians, policymakers, and individuals navigating pain management or recovery.
Supervised opioid use refers to medically monitored administration under structured conditions. This includes hospital pain control, prescription use as directed, medication-assisted treatment (MAT) such as buprenorphine or methadone, and supervised consumption programs. In these settings, dosage, frequency, and patient response are carefully tracked. Monitoring reduces overdose risk, identifies adverse effects early, and integrates counseling or behavioral therapy. Research consistently shows that structured supervision improves safety, treatment retention, and overall health outcomes.
Misuse, by contrast, occurs when opioids are taken outside medical guidance—such as using higher doses, taking someone else’s prescription, or using illicit opioids. Misuse disrupts brain reward pathways, increases tolerance, and raises overdose risk. Without supervision, individuals lack safeguards such as dose regulation, drug purity testing, and rapid emergency response. This is why unsupervised use is strongly associated with respiratory depression, infections, and long-term dependence.
Importantly, supervised environments do not encourage drug use; they aim to reduce harm while building pathways to recovery. Programs that combine medical oversight, sterile supplies, and access to treatment services have been shown to decrease fatal overdoses and increase engagement with addiction care. They act as bridges—meeting people where they are while guiding them toward stabilization and rehabilitation.
The central takeaway is this: opioids themselves are not inherently good or bad. Their impact depends on context, monitoring, and intent. When used under professional supervision, they can relieve suffering and support recovery. When misused, they can rapidly escalate into life-threatening conditions. Distinguishing between these realities helps shift the conversation from stigma to science, allowing more effective responses to the opioid crisis.
Self-Management Strategies: Understanding Opioid Supervised Use vs. Misuse
Self-management plays a powerful role in preventing opioid misuse and promoting safe, effective treatment. Whether opioids are prescribed for pain or used in recovery treatment, individuals who understand the difference between supervised use and misuse are better equipped to protect their health, recognize warning signs, and make informed decisions. Education, awareness, and intentional habits can dramatically reduce risk while supporting recovery or medical stability.
Supervised opioid use occurs when medication is taken exactly as prescribed or administered within a monitored setting. Self-management in this context means tracking doses, understanding side effects, communicating honestly with providers, and recognizing when medication is helping versus harming. Practical strategies include keeping a medication log, setting reminders to prevent accidental overuse, storing medications securely, and never adjusting dosage without professional guidance. These steps create a personal safety framework that complements medical oversight.
Understanding misuse is equally important. Misuse often begins subtly—taking an extra dose for uncontrolled pain, using medication to cope with stress, or saving pills “just in case.” Self-awareness helps individuals identify these patterns early. Recognizing emotional triggers, stress responses, and environmental influences can prevent escalation. Building alternative coping skills, such as relaxation techniques, structured routines, physical activity, and social support, reduces reliance on medication for non-medical needs.
Another key strategy is overdose preparedness. Individuals prescribed opioids or in recovery should learn overdose signs, keep naloxone accessible, and inform trusted people how to respond in emergencies. This is not a sign of failure—it is a safety measure, similar to wearing a seatbelt. Preparedness empowers individuals and families to act quickly in the event of a crisis.
Ultimately, self-management transforms patients from passive recipients of care into active participants in their own safety. When individuals understand how supervised opioid use differs from misuse—and apply daily strategies to maintain that boundary—they strengthen both their physical health and long-term recovery outcomes. Knowledge, structure, and support together create the foundation for safe opioid use and lasting wellness.
Family Support Strategies: Understanding Opioid Supervised Use vs. Misuse
Family involvement can be one of the most protective factors in preventing opioid misuse and supporting safe, supervised use. When loved ones understand how opioids work, why they are prescribed, and what misuse looks like, they become allies in safety rather than bystanders to risk. Education and communication help families support treatment goals while reducing stigma, fear, and misunderstanding.
A key strategy is learning the difference between supervised and unsupervised use. Supervised use means medication is taken exactly as directed, often under the supervision of healthcare providers. Families can reinforce this by encouraging adherence to dosing schedules, helping organize medications, and supporting follow-up appointments. Gentle check-ins, such as asking how pain or cravings are being managed, can open conversations without sounding accusatory. The goal is collaboration, not control.
Families should also recognize early warning signs of misuse. These may include running out of medication early, mood changes, secrecy, or using medication for emotional relief rather than medical need. Observing patterns without judgment allows concerns to be addressed early. Approaching the topic with empathy—using phrases like “I’m worried about you” rather than “You’re doing something wrong”—helps maintain trust and reduce defensiveness.
Creating a safe home environment is another practical step. This includes storing medications securely, properly disposing of unused prescriptions, and ensuring naloxone is available and that family members know how to use it. Preparedness is not an accusation; it is a proactive safety measure that can save lives in emergencies.
Emotional support is just as important as practical support. Individuals managing pain or recovery often experience fear, shame, or frustration. Families who listen, validate feelings, and celebrate progress help build resilience and motivation. Encouraging healthy coping skills—such as counseling, exercise, peer support groups, or stress-management techniques—can reduce reliance on opioids for emotional relief.
In the end, families cannot control another person’s choices, but they can shape the environment in which those choices are made. When relatives understand the distinction between supervised opioid use and misuse, they become partners in prevention, healing, and recovery. Through knowledge, compassion, and consistent support, families can help protect their loved ones while strengthening trust and long-term well-being.
Community Resource Strategies: Understanding Opioid Supervised Use vs. Misuse
Communities play a decisive role in shaping how opioids are used, understood, and managed. While individuals and families influence daily decisions, community systems determine access to care, education, and safety resources. When communities provide strong support networks and accessible services, they help people distinguish between supervised opioid use for legitimate medical or recovery purposes and misuse that can lead to harm. Effective community strategies create environments where safety, treatment, and prevention work together.
One of the most impactful approaches is expanding access to supervised care services. Community clinics, pain management centers, and medication-assisted treatment programs offer structured environments where opioid use is monitored by trained professionals. These settings ensure correct dosing, monitor side effects, and provide counseling support. When communities invest in these services and make them affordable and accessible, they reduce the likelihood that individuals will turn to unsafe or unsupervised sources.
Education initiatives are equally vital. Public workshops, school programs, and local health campaigns can teach residents how opioids affect the brain, what safe use looks like, and how misuse develops. When accurate information replaces myths and stigma, people are more likely to seek help early. Community education also empowers neighbors, coworkers, and friends to recognize warning signs and respond compassionately rather than judgmentally.
Harm-reduction resources strengthen safety even further. Programs that distribute naloxone, provide drug-checking tools, or offer safe disposal sites for unused medications directly lower overdose risk and prevent diversion. These services do not encourage misuse; instead, they acknowledge real-world risks and prioritize survival and stabilization. Many individuals who engage with harm-reduction programs eventually transition into treatment, making these services important entry points into recovery.
Peer support networks also contribute significantly. Recovery groups, faith-based initiatives, and community mentorship programs provide connection, accountability, and shared experience. Isolation is a major risk factor for misuse, while belonging is a powerful protective factor. Communities that foster inclusive, nonjudgmental support spaces help individuals feel safe discussing struggles and seeking assistance.
Ultimately, understanding opioid supervised use versus misuse is not solely an individual responsibility—it is a collective one. Communities that combine accessible treatment, public education, harm-reduction tools, and supportive social networks create a safety net that protects residents and promotes recovery. When communities lead with knowledge and compassion, they transform from passive observers of the opioid crisis into active agents of prevention, healing, and hope.
Frequently Asked Questions
Here are some common questions:
1. What is supervised opioid use?
Supervised use means opioids are taken exactly as prescribed or administered in a medically monitored setting. Healthcare professionals track dosage, response, and side effects to ensure safety and effectiveness.
2. What qualifies as opioid misuse?
Misuse occurs when opioids are used outside medical direction. This includes taking higher doses than prescribed, using someone else’s medication, using illicit opioids, or using them for emotional relief rather than medical need.
3. Can someone misuse opioids even if they have a prescription?
Yes. Misuse can happen if a person changes their dose, frequency, or method of use without medical guidance, even if the medication was originally prescribed.
4. Why is supervision important?
Medical supervision reduces risks such as overdose, drug interactions, dependence, and untreated side effects. It also allows providers to adjust treatment plans quickly if problems arise.
5. Do supervised opioid programs encourage drug use?
No. Structured programs are designed to reduce harm, stabilize health, and connect individuals with treatment and recovery services. Evidence shows they can lower overdose deaths and increase treatment engagement.
6. What are the signs of possible misuse?
Common warning signs include running out of medication early, cravings, mood changes, secrecy about use, doctor shopping, or using medication for stress relief instead of medical symptoms.
7. How can patients prevent misuse?
Strategies include following prescriptions strictly, keeping a medication log, using one pharmacy, communicating honestly with providers, and avoiding alcohol or sedatives unless approved.
8. What role does naloxone play?
Naloxone is a medication that reverses opioid overdoses. Keeping it accessible and knowing how to use it can save lives, especially for individuals prescribed opioids or those in recovery.
9. Are all opioid users at risk of addiction?
Not everyone who uses opioids develops addiction, but risk increases with higher doses, longer duration, personal or family history of substance use disorders, and certain mental health conditions.
10. When should someone seek help?
Help should be sought immediately if a person notices loss of control over use, increasing tolerance, withdrawal symptoms, or using opioids despite negative consequences. Early support greatly improves outcomes.
Conclusion
Ultimately, opioids themselves are not inherently harmful or beneficial—their impact depends on how they are used. Supervised use emphasizes safety, structure, and therapeutic purpose, while misuse reflects loss of control and heightened risk. Education, awareness, and access to supportive resources empower individuals to stay within safe boundaries and seek help when needed. By promoting understanding rather than judgment, society can better prevent misuse, support recovery, and ensure opioids are used responsibly as part of effective medical care.
Video: Opioids Supervised vs Misuse — Understanding the Critical Difference