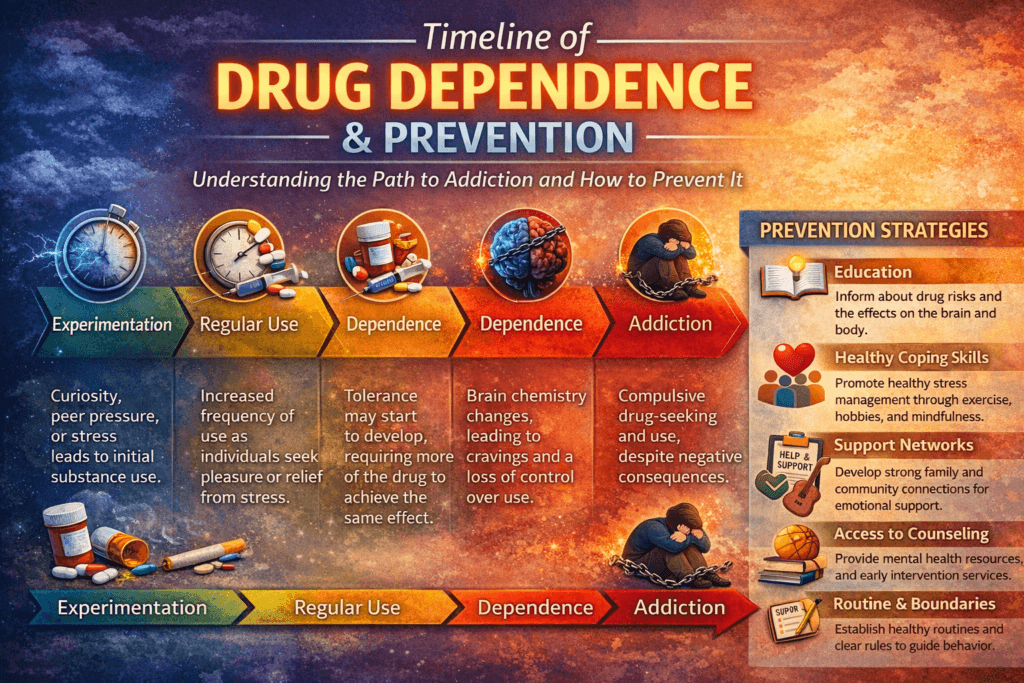
The timeline of drug dependence varies widely from person to person, shaped by factors such as genetics, mental health, environment, frequency of use, and the pharmacologic properties of the substance itself. Some individuals may develop signs of psychological attachment after only a few exposures, while others may use intermittently for longer periods before dependence appears. Understanding this variability is essential for prevention, because addiction is not defined by duration alone but by how rapidly the brain’s reward, motivation, and self-control systems adapt to a substance. Recognizing early warning signs—such as cravings, tolerance, or using substances to cope with stress—allows individuals, families, and healthcare professionals to intervene before patterns become entrenched.
How Fast Can Addiction Happen? Understanding the Timeline of Drug Dependence
One of the most common misconceptions about substance use is the belief that addiction takes years to develop. In reality, the timeframe for becoming addicted to a drug varies widely and can range from a single exposure to months or years, depending on biological, psychological, and environmental factors. Addiction is not defined solely by how long someone uses a substance, but by how quickly the brain’s reward system adapts to it.
Some drugs can begin altering brain chemistry after the first use. Substances that rapidly increase dopamine—such as nicotine, opioids, or stimulants—can create powerful reinforcement signals that encourage repeated use. For certain individuals, especially those with genetic vulnerability, trauma history, or underlying mental health conditions, this reinforcement can lead to cravings and loss of control surprisingly fast. This is why some people report feeling “hooked” after only a few experiences.
Short-acting, fast-onset drugs tend to carry the highest addiction risk because they create an intense but brief reward, prompting repeated dosing. The faster a drug reaches the brain and produces euphoria, the stronger the conditioning effect. Conversely, substances with slower onset or milder reward signals may take longer to produce dependence, though they can still become addictive with repeated exposure.
Frequency and pattern of use matter as much as time. Daily use accelerates neuroadaptation, while binge patterns can rapidly sensitize reward pathways. Psychological dependence—craving the emotional relief a drug provides—can develop before physical dependence appears. Over time, tolerance may form, requiring higher doses to achieve the same effect, which increases both addiction risk and medical danger.
The environmental context also shapes addiction speed. Stress, social environment, access to substances, and learned coping behaviors influence whether experimentation progresses to compulsive use. Supportive environments and early intervention can slow or prevent this progression, while isolation and chronic stress often accelerate it.
Ultimately, addiction is not a fixed timeline but a process. For some, it unfolds gradually; for others, it can emerge quickly. Understanding that vulnerability differs from person to person helps reduce stigma and highlights why early education, prevention, and prompt treatment are critical. The key takeaway is simple: addiction is less about how long someone has used a drug and more about how the brain and life circumstances respond to it.
Staying in Control: Self-Management Strategies to Prevent Drug Addiction
Preventing drug addiction is not simply about willpower—it is about building a lifestyle, mindset, and support structure that protects your brain’s reward system and emotional resilience. Self-management strategies empower individuals to recognize risk early, regulate impulses, and maintain healthy coping habits before substance use becomes a problem. These approaches are especially important because addiction often begins subtly, with occasional use that gradually turns into reliance.
One of the most effective strategies is self-awareness. Understanding personal triggers—such as stress, boredom, social pressure, trauma reminders, or emotional distress—helps individuals anticipate vulnerable moments. Keeping a journal, using mood-tracking apps, or reflecting daily can reveal patterns between emotions and urges. Once triggers are identified, they can be addressed proactively instead of reactively.
Healthy coping skills are another essential protective factor. Exercise, creative hobbies, mindfulness, structured routines, and social connection stimulate the brain’s natural reward pathways without the use of substances. These activities regulate dopamine and serotonin levels in healthier ways, reducing the appeal of artificial chemical highs. People who intentionally build routines around sleep, nutrition, and physical activity often develop stronger emotional regulation and resilience.
Setting clear personal boundaries is also critical. This may include limiting exposure to environments where substances are present, confidently declining offers, or choosing social circles aligned with one’s goals. Practicing refusal skills in advance—such as rehearsing what to say—can make it easier to respond calmly in real-life situations.
Another powerful strategy is education. Understanding how drugs affect the brain, body, and behavior reduces curiosity fueled by myths or peer influence. Knowledge transforms impulsive decisions into informed ones. Individuals who learn about tolerance, dependence, and long-term health risks are more likely to pause and evaluate consequences before experimenting.
Stress management also plays a central role. Chronic stress is one of the strongest predictors of substance misuse. Techniques such as deep breathing, progressive muscle relaxation, meditation, or structured problem-solving help reduce physiological arousal and emotional overload. When stress is managed effectively, the urge to escape through substances decreases significantly.
Finally, accountability and support systems strengthen prevention. Trusted friends, mentors, therapists, or support groups provide encouragement, perspective, and early feedback if risky behaviors appear. Prevention is rarely a solo effort; it thrives in environments where people feel seen, supported, and valued.
In the end, avoiding addiction is less about resisting temptation and more about building a life where substances are unnecessary for coping or fulfillment. Self-management strategies create a foundation of stability, self-confidence, and purpose—making healthy choices not just possible, but natural.
Strong Families, Strong Protection: How Family Support Helps Prevent Drug Addiction
Family support is one of the most powerful protective factors against drug addiction. Research consistently shows that individuals who grow up or live in supportive, communicative, and emotionally safe family environments are less likely to experiment with substances or develop dependence. Prevention does not begin when a problem appears—it begins with daily interactions, modeling behaviors, and relationships that build resilience long before substances enter the picture.
One of the most important strategies families can use is open communication. When family members feel safe discussing emotions, stress, mistakes, and curiosity without fear of judgment or punishment, they are more likely to seek guidance instead of turning to substances for relief or escape. Honest conversations about peer pressure, mental health, and substance risks create trust and normalize asking for help.
Modeling healthy behavior is equally essential. Family members—especially parents or caregivers—serve as powerful examples. Demonstrating responsible coping skills, emotional regulation, and balanced stress management is taught by observation. When adults handle conflict calmly, prioritize wellness, and avoid unhealthy substance habits, younger or more vulnerable members internalize those behaviors as normal and achievable.
Another key protective factor is consistent structure and boundaries. Clear expectations about behavior, curfews, responsibilities, and consequences provide stability and reduce impulsive risk-taking. Structure communicates care and involvement, while also helping individuals develop self-discipline and decision-making skills that protect against experimentation driven by boredom or peer influence.
Families can also strengthen prevention through emotional support and validation. Feeling valued, understood, and accepted lowers the likelihood that someone will seek external relief through drugs. Simple actions—such as active listening, expressing encouragement, celebrating progress, and acknowledging struggles—build self-esteem and emotional security, both of which reduce addiction vulnerability.
Shared activities and connection time further reinforce resilience. Regular family meals, outings, hobbies, or traditions foster a sense of belonging and reduce isolation. Strong relational bonds make it easier for family members to notice behavioral changes early and intervene supportively if concerns arise.
Finally, families benefit from early education and proactive awareness. Learning together about substance risks, mental health, and coping skills transforms prevention into a team effort. Families who discuss these topics before exposure occurs create a protective knowledge base that helps individuals make informed decisions when faced with real-world situations.
In essence, family support does not just reduce the risk of addiction—it builds the emotional, social, and psychological foundation that makes substance misuse less appealing in the first place. When families cultivate trust, structure, empathy, and connection, they create an environment where healthy choices can thrive, and vulnerability to addiction is significantly reduced.
Prevention Through Connection: Community Resource Strategies to Avoid Drug Addiction
Drug addiction prevention is most effective when it extends beyond the individual and family into the broader community. Community resources provide education, structure, support, and opportunity—key protective factors that reduce vulnerability to substance misuse. When people feel connected, informed, and supported within their environment, they are far less likely to rely on drugs as a coping mechanism or escape.
One of the most impactful strategies communities offer is accessible education programs. Schools, health departments, and local organizations often provide workshops, seminars, and outreach campaigns that teach the science of addiction, decision-making skills, and emotional resilience. Early exposure to accurate information helps individuals recognize risks, resist peer pressure, and make informed choices before experimentation begins.
Youth and adult enrichment programs also play a major preventive role. After-school activities, sports leagues, arts programs, job training initiatives, and volunteer opportunities give individuals a sense of purpose, belonging, and achievement. These positive outlets activate natural reward pathways in the brain, reducing the desire for artificial stimulation from substances.
Another essential community strategy is access to mental health and counseling services. Many people turn to substances to cope with untreated anxiety, depression, trauma, or stress. Communities that provide affordable or free counseling, crisis lines, peer-support groups, and wellness clinics address root causes rather than waiting for addiction to develop. Early intervention often prevents experimentation from progressing into dependence.
Safe social environments also matter. Community centers, faith-based groups, libraries, recreation facilities, and sober events create spaces where individuals can connect without exposure to substances. These environments normalize healthy socializing and show that meaningful connection does not require alcohol or drugs.
Communities can further strengthen prevention through mentorship and peer leadership programs. Positive role models—coaches, teachers, counselors, or trained peers—offer guidance, accountability, and encouragement. Mentors help individuals set goals, navigate stress, and build confidence, all of which reduce susceptibility to risky behaviors.
Finally, public awareness and stigma reduction initiatives are crucial. When communities openly discuss addiction as a health condition rather than a moral failing, people are more willing to seek help early. Public campaigns, recovery events, and educational panels foster understanding and compassion, making prevention a shared responsibility rather than an individual burden.
In the end, strong communities act as protective ecosystems. They provide knowledge, support, opportunity, and connection—the very elements that decrease the likelihood of substance misuse. Prevention is not just about avoiding drugs; it is about creating environments where people feel empowered, valued, and supported enough that they do not need them.
Frequently Asked Questions
Here are some common questions:
1. How quickly can someone become addicted to a drug?
Addiction can develop at very different speeds. Some substances can trigger strong reinforcement after only one or a few uses, especially fast-acting drugs that rapidly affect brain chemistry. For others, dependence develops gradually over weeks or months of repeated use.
2. What factors affect how fast dependence develops?
Several variables influence addiction timelines, including genetics, mental health status, trauma history, frequency of use, drug potency, method of administration, stress levels, and social environment. These factors interact to determine vulnerability.
3. Is experimentation the same as addiction?
No. Experimentation refers to initial or occasional use, while addiction involves compulsive use despite negative consequences, cravings, and loss of control. However, experimentation can progress if risk factors are present and protective factors are absent.
4. What are the early warning signs of developing dependence?
Early signs may include increasing tolerance, cravings, using substances to cope with emotions, prioritizing use over responsibilities, and feeling uncomfortable or irritable when not using.
5. Can someone become dependent without daily use?
Yes. Binge patterns or intermittent heavy use can still lead to dependence. Addiction is determined by behavioral and neurological changes, not just frequency.
6. Why do some people become addicted faster than others?
Individual brain chemistry, personality traits, stress exposure, and environmental influences all play roles. People with underlying anxiety, depression, or trauma histories may be more susceptible because substances temporarily relieve distress.
7. What is the difference between psychological and physical dependence?
Psychological dependence involves emotional cravings and perceived need for a substance, while physical dependence involves the body adapting to the drug and experiencing withdrawal symptoms when use stops. Both can occur together or separately.
8. Can prevention really stop addiction before it starts?
Yes. Education, healthy coping skills, supportive relationships, and structured routines significantly reduce the likelihood of substance misuse. Prevention works best when started early and reinforced consistently.
9. What are the most effective prevention strategies?
Strong prevention approaches include stress-management skills, emotional-regulation training, mentorship, physical activity, access to mental health care, and supportive family or community environments.
10. Is it ever too late to prevent addiction?
No. Prevention is beneficial at any stage. Even if someone has begun experimenting or using regularly, early intervention and support can interrupt progression and reduce long-term harm.
11. How does stress influence the timeline of dependence?
Chronic stress increases vulnerability by activating brain systems involved in reward and relief. People under prolonged stress may turn to substances for coping, which can accelerate the transition from use to dependence.
12. What role does education play in prevention?
Education provides realistic expectations about the effects, risks, and long-term consequences of substance use. Informed individuals are more likely to recognize warning signs early and make safer decisions.
13. Can the social environment speed up addiction risk?
Yes. Environments where substance use is normalized or easily accessible can increase exposure and reduce perceived risk, which may accelerate progression toward dependence.
14. Do all drugs carry the same addiction timeline?
No. Drugs that reach the brain quickly and produce intense reward signals typically carry higher addiction potential. Slower-acting substances may still cause dependence, but often over longer periods.
15. What is the most important takeaway about addiction timelines?
There is no single timeline. Addiction is a process influenced by biology, behavior, and environment. Understanding risk factors and strengthening prevention strategies is the most effective way to protect long-term health.
Conclusion
Awareness of how quickly dependence can develop reinforces the importance of early prevention strategies at personal, family, and community levels. Education, emotional support, stress-management skills, and access to healthy coping outlets all serve as protective barriers that slow or halt progression toward addiction. Rather than focusing solely on how long someone has used a substance, effective prevention emphasizes understanding risk factors, strengthening resilience, and promoting informed decision-making. When people are equipped with knowledge and support early, the trajectory toward dependence can often be interrupted, making prevention one of the most powerful tools in reducing substance-related harm.
Video: How Fast Addiction Actually Happens #addiction #facts #health