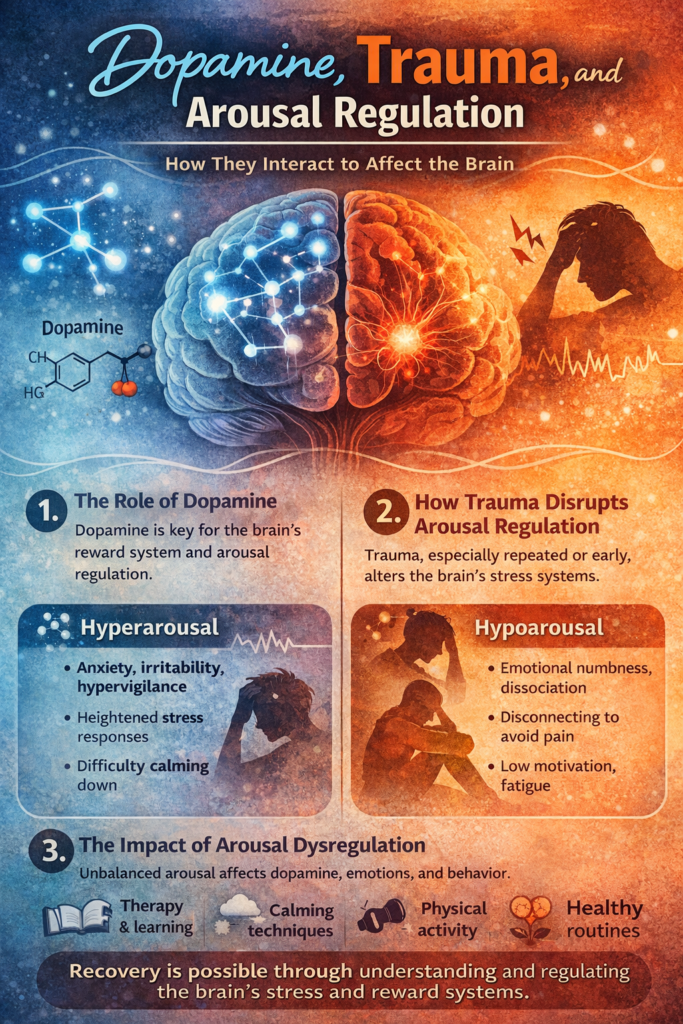
Dopamine, trauma, and arousal regulation are closely linked processes that influence how people experience motivation, stress, and emotional stability. Dopamine is essential for reward and goal-directed behavior, while trauma can interfere with the brain’s ability to regulate arousal, resulting in states of hyperarousal (such as anxiety and irritability) or hypoarousal (such as numbness and low motivation). These effects go beyond psychological responses and reflect deeper neurobiological adaptations shaped by stress and past experiences. Understanding the interaction of these systems helps explain patterns like emotional reactivity, difficulty focusing, and increased risk for addiction, offering a more informed and compassionate view of mental health.
Dopamine, Trauma, and Arousal Regulation: Understanding the Brain’s Stress and Reward Systems
The human brain is constantly working to maintain balance between states of calm and alertness, a process known as arousal regulation. Central to this system are neurotransmitters like dopamine, which influence motivation and reward, and stress-related systems shaped by life experiences—especially trauma. When trauma occurs, particularly in early or repeated forms, it can disrupt how the brain regulates arousal, leading to patterns of hyperarousal (anxiety, irritability) or hypoarousal (numbness, disconnection). Understanding how dopamine and trauma interact provides important insight into emotional regulation, mental health, and behaviors such as addiction.
The Role of Dopamine in Arousal
Dopamine is often associated with pleasure, but its primary role is in motivation, attention, and goal-directed behavior. It helps the brain determine what is important and worth pursuing.
In a balanced system:
- Dopamine supports focus and engagement
- It reinforces positive, adaptive behaviors
- It contributes to a stable sense of reward and motivation
However, when arousal systems are dysregulated, dopamine signaling can become inconsistent—either overactive or underactive—affecting mood and behavior.
How Trauma Disrupts Arousal Regulation
Trauma can significantly alter the brain’s stress response systems, particularly those involving the amygdala (fear processing) and the nervous system.
Common effects include:
- Hyperarousal: heightened anxiety, irritability, hypervigilance
- Hypoarousal: emotional numbness, low motivation, dissociation
- Difficulty returning to a calm baseline after stress
These states are not choices—they are the result of the brain adapting to perceived threats.
The Dopamine–Trauma Connection
Trauma doesn’t just affect fear and stress—it also impacts the brain’s reward system.
- Chronic stress can reduce dopamine sensitivity
- Natural rewards may feel less satisfying
- Individuals may seek intense stimuli (e.g., substances, risky behaviors) to compensate
This connection helps explain why trauma is strongly linked to addiction and difficulties with motivation.
Arousal Dysregulation in Daily Life
When dopamine and stress systems are out of balance, individuals may experience:
- Difficulty concentrating or staying motivated
- Emotional highs and lows
- Increased reactivity to stress
- Reliance on external stimuli to feel “normal.”
These patterns reflect a nervous system struggling to regulate itself.
Strategies for Regulating Arousal
Understanding the brain allows for more targeted approaches to regulation:
- Grounding techniques: help bring the nervous system back to baseline
- Physical activity: supports dopamine balance and reduces stress
- Consistent routines: stabilize brain and body rhythms
- Mindfulness practices: improve awareness and emotional control
These strategies work by gradually retraining the brain’s regulatory systems.
Healing Through Neuroplasticity
The brain has the ability to adapt and recover through neuroplasticity. With consistent support:
- Stress responses can become less reactive
- Dopamine systems can rebalance
- Emotional regulation can improve
This process takes time, but it is possible.
Conclusion
Dopamine, trauma, and arousal regulation are deeply interconnected aspects of brain function that shape how individuals experience motivation, stress, and emotional balance. Trauma can disrupt these systems, leading to patterns of dysregulation that affect daily life and behavior. By understanding these neurobiological processes, individuals and professionals can develop more effective, compassionate strategies for healing. Ultimately, restoring balance in the brain’s reward and stress systems is key to improving well-being and resilience.
Self-Management Strategies for Dopamine, Trauma, and Arousal Regulation
Understanding the relationship between dopamine, trauma, and arousal regulation provides a powerful foundation for personal change. When trauma disrupts the brain’s stress and reward systems, individuals may experience cycles of anxiety, numbness, low motivation, or emotional reactivity. These patterns are not signs of weakness—they reflect a nervous system that has adapted to past experiences. Self-management strategies focus on helping the brain regain balance by stabilizing arousal levels and supporting healthy dopamine function over time.
Why Self-Management Matters
Because these systems operate automatically, change requires intentional, repeated actions that gradually retrain the brain. Self-management helps:
- Regulate emotional highs and lows
- Restore motivation and focus
- Reduce reliance on unhealthy coping behaviors
The goal is to move toward a balanced state of arousal, where you feel calm, alert, and in control.
1. Stabilizing Arousal Through Grounding
When the nervous system becomes overwhelmed (hyperarousal) or shut down (hypoarousal), grounding techniques help bring it back to baseline.
- Focus on sensory input (what you can see, hear, feel)
- Practice slow, controlled breathing
- Use physical contact (holding an object, feet on the ground)
These techniques signal safety to the brain and reduce stress responses.
2. Supporting Healthy Dopamine Levels
Trauma can disrupt dopamine, making it harder to feel motivated or rewarded by everyday activities.
- Break tasks into small, achievable steps
- Celebrate small wins to reinforce progress
- Engage in activities that provide natural rewards (exercise, hobbies, social connection)
This helps rebuild the brain’s reward system gradually.
3. Creating Predictable Routines
Consistency is critical for regulating both dopamine and stress systems.
- Maintain regular sleep and wake times
- Structure your day with planned activities
- Reduce unpredictability when possible
Predictable routines signal safety and stability to the nervous system.
4. Managing Triggers and Stress Responses
Trauma can make the brain more sensitive to perceived threats.
- Identify personal triggers (situations, emotions, environments)
- Develop coping strategies before encountering them
- Use pause techniques (stop, breathe, respond) instead of reacting impulsively
This strengthens control over automatic responses.
5. Practicing Mindfulness and Awareness
Awareness helps you recognize shifts in arousal before they escalate.
- Notice early signs of stress or shutdown
- Label emotions without judgment
- Stay present rather than reacting to past experiences
Mindfulness builds a stronger connection between awareness and action.
6. Engaging the Body for Regulation
The body plays a key role in regulating brain chemistry.
- Regular physical activity helps balance dopamine and reduce stress
- Stretching or yoga can calm the nervous system
- Movement helps release built-up tension
Physical regulation supports mental and emotional balance.
7. Building Safe Connections
Healthy relationships help regulate both stress and reward systems.
- Spend time with supportive, trustworthy people
- Communicate needs and boundaries clearly
- Seek connection rather than isolation
Social interaction naturally supports dopamine and emotional regulation.
Important Considerations
Self-management is valuable, but it may not replace professional support.
- Trauma can be complex and deeply rooted
- Therapy (e.g., trauma-informed care) can provide additional tools
- Progress may be gradual, with setbacks along the way
Combining self-management with professional guidance often leads to the best outcomes.
A Brain-Based Approach to Healing
Understanding dopamine, trauma, and arousal regulation shifts the focus from “What’s wrong with me?” to “What does my brain need?” This perspective encourages patience and practical strategies that align with how the brain heals.
Conclusion
Self-management strategies offer a practical way to support recovery and emotional balance by working with the brain’s natural systems. Through grounding, routine, mindful awareness, and healthy reinforcement of dopamine pathways, individuals can gradually restore regulation and resilience. Healing is not immediate, but with consistent effort, the brain can relearn stability—creating a stronger foundation for long-term well-being.
Family Support for Dopamine, Trauma, and Arousal Regulation: Helping the Brain Heal Together
Understanding how dopamine, trauma, and arousal regulation shape behavior can transform the way families support a loved one. When someone has experienced trauma, their brain may struggle to maintain balance between stress and calm states, often leading to irritability, emotional withdrawal, or difficulty with motivation. These responses are not intentional—they reflect changes in the brain’s stress and reward systems. Family support, when informed by this understanding, becomes a powerful tool for regulating these systems and promoting long-term healing.
Why Family Support Matters
Trauma and dysregulated dopamine systems can make everyday life feel overwhelming or unrewarding. Family members who understand this can:
- Respond with empathy instead of frustration
- Help reduce stress triggers that worsen dysregulation
- Reinforce healthy patterns that support brain recovery
Supportive relationships can act as a stabilizing force for the nervous system.
1. Creating a Safe and Predictable Environment
The brain heals best in environments that feel safe and consistent.
- Maintain regular routines and structure
- Minimize chaos, conflict, and unpredictability
- Respect personal space and boundaries
A stable environment helps regulate the nervous system and reduces hyperarousal.
2. Responding to Behavior with Understanding
Trauma-related behaviors (e.g., irritability, withdrawal) are often misunderstood.
- Avoid taking reactions personally
- Recognize these behaviors as stress responses, not intentional actions
- Use calm, supportive communication
This reduces shame and prevents escalation.
3. Supporting Healthy Dopamine Activities
Trauma can reduce sensitivity to natural rewards, making motivation difficult.
Families can help by:
- Encouraging small, enjoyable activities
- Celebrating effort rather than perfection
- Participating in positive routines together
These actions help rebuild the brain’s reward system over time.
4. Helping Regulate Emotional States
Family members can help restore the nervous system to balance.
- Offer grounding support during stressful moments (e.g., calm voice, reassurance)
- Encourage breaks when emotions become overwhelming
- Model healthy coping strategies
Co-regulation—calming together—can be especially powerful.
5. Encouraging Open Communication
Understanding grows through safe, honest dialogue.
- Ask open-ended, nonjudgmental questions
- Listen without trying to immediately “fix” the problem
- Validate feelings, even when you don’t fully understand them
Feeling heard supports emotional regulation and trust.
6. Practicing Patience and Consistency
Healing from trauma and restoring dopamine balance takes time.
- Expect gradual progress rather than quick change
- Avoid reacting to setbacks with disappointment or pressure
- Reinforce consistency in routines and support
The brain responds best to steady, repeated experiences of safety.
7. Seeking Education and Support as a Family
Families benefit from learning together.
- Explore trauma-informed care resources
- Attend family therapy or support groups
- Learn about how the brain processes stress and reward
Education reduces confusion and strengthens support strategies.
Important Considerations
While family support is essential, it is not a replacement for professional care.
- Trauma may require specialized therapy
- Boundaries are important to avoid burnout
- Each individual’s healing process is unique
Healthy support balances compassion with realistic expectations.
A Shared Path Toward Healing
Understanding dopamine, trauma, and arousal regulation shifts the focus from blame to biology. Families can move from asking “Why are they acting this way?” to “What is their brain experiencing, and how can we help?”
Conclusion
Family support plays a vital role in helping regulate the brain’s stress and reward systems after trauma. By creating a safe environment, reinforcing healthy behaviors, and responding with empathy, families can help restore balance and resilience. Healing is not just an individual process—it is strengthened through connection, understanding, and consistent support.
Community Resource Strategies for Understanding Dopamine, Trauma, and Arousal Regulation
Understanding how dopamine, trauma, and arousal regulation shape behavior is essential for improving mental health and supporting recovery. However, this knowledge can be difficult to apply without access to education, support, and structured resources. Community-based strategies play a critical role in making neuroscience-informed care accessible, helping individuals and families translate complex brain processes into practical tools for daily life. By combining education, support networks, and accessible services, communities can foster environments that promote regulation, resilience, and healing.
Why Community Resources Matter
Trauma and dysregulated arousal systems often lead to cycles of stress, low motivation, and emotional instability. Community resources help by:
- Providing education about how the brain responds to trauma
- Offering support systems that reduce isolation
- Creating structured environments that promote stability
These resources bridge the gap between understanding brain science and applying it in real life.
1. Community Education and Awareness Programs
Education is the foundation of effective support.
- Workshops on trauma-informed care and brain function
- Public seminars on stress, dopamine, and emotional regulation
- School and workplace programs that teach coping strategies
These initiatives help normalize mental health challenges and reduce stigma.
2. Peer Support and Integration Groups
Shared experiences can reinforce learning and provide emotional support.
- Trauma-informed peer support groups
- Community mental health circles
- Groups focused on stress regulation and coping skills
These spaces allow individuals to connect their experiences with underlying brain processes.
3. Access to Mental Health Services
Professional guidance helps individuals apply neuroscience-based strategies effectively.
- Community clinics offering therapy and counseling
- Trauma-informed therapists trained in regulation techniques
- Programs that integrate mindfulness, CBT, or somatic approaches
Accessible care is essential for long-term regulation and recovery.
4. Stress-Reducing Community Environments
Communities can actively shape environments that support nervous system regulation.
- Safe public spaces and community centers
- Access to parks, exercise programs, and wellness activities
- Reduced exposure to high-stress or chaotic environments
These factors help stabilize arousal systems and support dopamine balance.
5. Youth and Prevention Programs
Early education can prevent long-term dysregulation.
- Programs teaching emotional regulation in schools
- Youth mentorship and structured activities
- Education on coping with stress and trauma
Supporting regulation early can reduce future mental health challenges.
6. Outreach and Accessibility Initiatives
Not everyone has equal access to resources, making outreach essential.
- Mobile mental health services
- Online support groups and virtual education
- Sliding-scale or free community programs
These efforts ensure broader access to support and knowledge.
Important Considerations
While community resources are valuable, challenges exist:
- Limited access in rural or underserved areas
- Variability in program quality
- Need for culturally informed and inclusive services
Combining community resources with individual and professional support leads to the best outcomes.
A Community-Based Approach to Brain Health
Understanding dopamine, trauma, and arousal regulation shifts how communities respond to mental health—from reacting to behaviors to supporting underlying brain processes. This approach promotes empathy, reduces stigma, and encourages proactive care.
Conclusion
Community resource strategies are essential for translating the science of dopamine, trauma, and arousal regulation into meaningful support. Through education, peer networks, mental health services, and supportive environments, communities can help individuals regulate their nervous systems and rebuild healthy patterns. Healing is not just an individual journey—it is strengthened by informed, connected, and supportive communities working together.
Frequently Asked Questions
Here are some common questions:
1. What is arousal regulation?
Arousal regulation refers to the brain’s ability to maintain a balanced state between alertness and calmness. It allows you to respond appropriately to stress and return to a baseline state afterward.
2. What role does dopamine play in arousal?
Dopamine helps regulate:
- Motivation
- Attention
- Reward-seeking behavior
Balanced dopamine supports focus and engagement, while dysregulation can lead to low motivation or impulsive behavior.
3. How does trauma affect the brain?
Trauma can alter the brain’s stress response systems, making it harder to regulate emotions and arousal. It often leads to heightened sensitivity to perceived threats.
4. What is hyperarousal?
Hyperarousal is a state of excessive activation of the nervous system, including:
- Anxiety
- Irritability
- Hypervigilance
- Difficulty relaxing
It’s commonly seen in individuals with trauma.
5. What is hypoarousal?
Hypoarousal is the opposite state, involving:
- Emotional numbness
- Low energy or motivation
- Disconnection or dissociation
It reflects an underactive nervous system.
6. How are dopamine and trauma connected?
Chronic stress and trauma can:
- Reduce dopamine sensitivity
- Make natural rewards feel less satisfying
- Increase the need for intense stimulation
This can contribute to behaviors like addiction or risk-taking.
7. Why do people with trauma struggle with motivation?
Disruptions in dopamine pathways can make everyday tasks feel less rewarding, leading to low motivation and difficulty initiating activities.
8. Can trauma cause mood swings?
Yes. Dysregulated arousal can lead to rapid shifts between hyperarousal (anxiety, anger) and hypoarousal (numbness, fatigue).
9. What is the “window of tolerance”?
It’s the optimal zone where a person can function effectively—calm, focused, and emotionally regulated. Trauma can narrow this window, making regulation harder.
10. How does stress affect dopamine?
Chronic stress can decrease dopamine function, reducing pleasure and increasing the likelihood of seeking external rewards (e.g., substances or risky behaviors).
11. Can the brain recover from trauma-related dysregulation?
Yes. Through neuroplasticity, the brain can:
- Rebalance stress responses
- Improve dopamine function
- Strengthen emotional regulation
This takes time and consistent support.
12. What are the signs of arousal dysregulation?
- Overreacting to stress
- Difficulty calming down
- Feeling emotionally numb
- Trouble focusing or staying motivated
13. How can someone regulate their arousal?
Helpful strategies include:
- Grounding techniques
- Deep breathing
- Physical activity
- Consistent routines
- Mindfulness practices
14. Why is understanding this topic important?
It helps:
- Reduce self-blame
- Improve emotional awareness
- Guide effective coping strategies
- Support trauma-informed care
15. How is this connected to addiction?
Dysregulated dopamine and stress systems can lead individuals to seek substances or behaviors that temporarily restore balance, reinforcing addictive patterns.
Conclusion
Recognizing the connection among dopamine, trauma, and arousal regulation highlights the importance of addressing both the brain’s reward system and its stress response in the healing process. Dysregulation in these systems can make everyday functioning challenging, but the brain’s capacity for neuroplasticity allows for gradual recovery with consistent support and effective strategies. By understanding these processes, individuals and those around them can move beyond blame and toward informed, supportive approaches that promote stability and resilience. Ultimately, restoring balance in arousal and dopamine systems is key to improving emotional well-being and long-term mental health.
Video: Your Arousal State Determines Everything #Performance #Focus #BrainPower